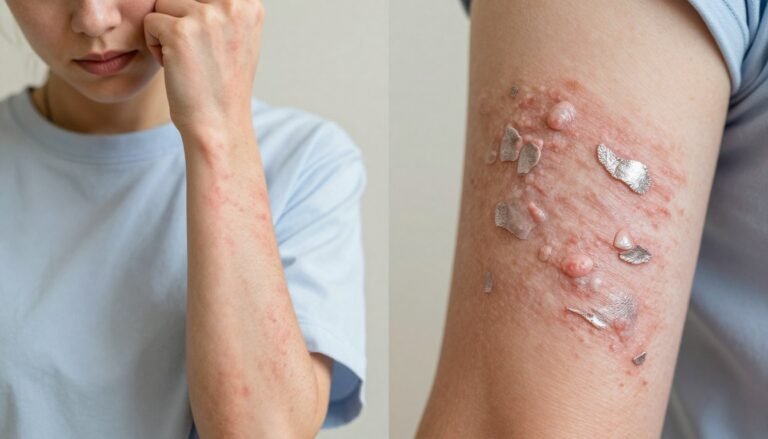
What Is Eczema? Types, Causes & Symptoms Explained
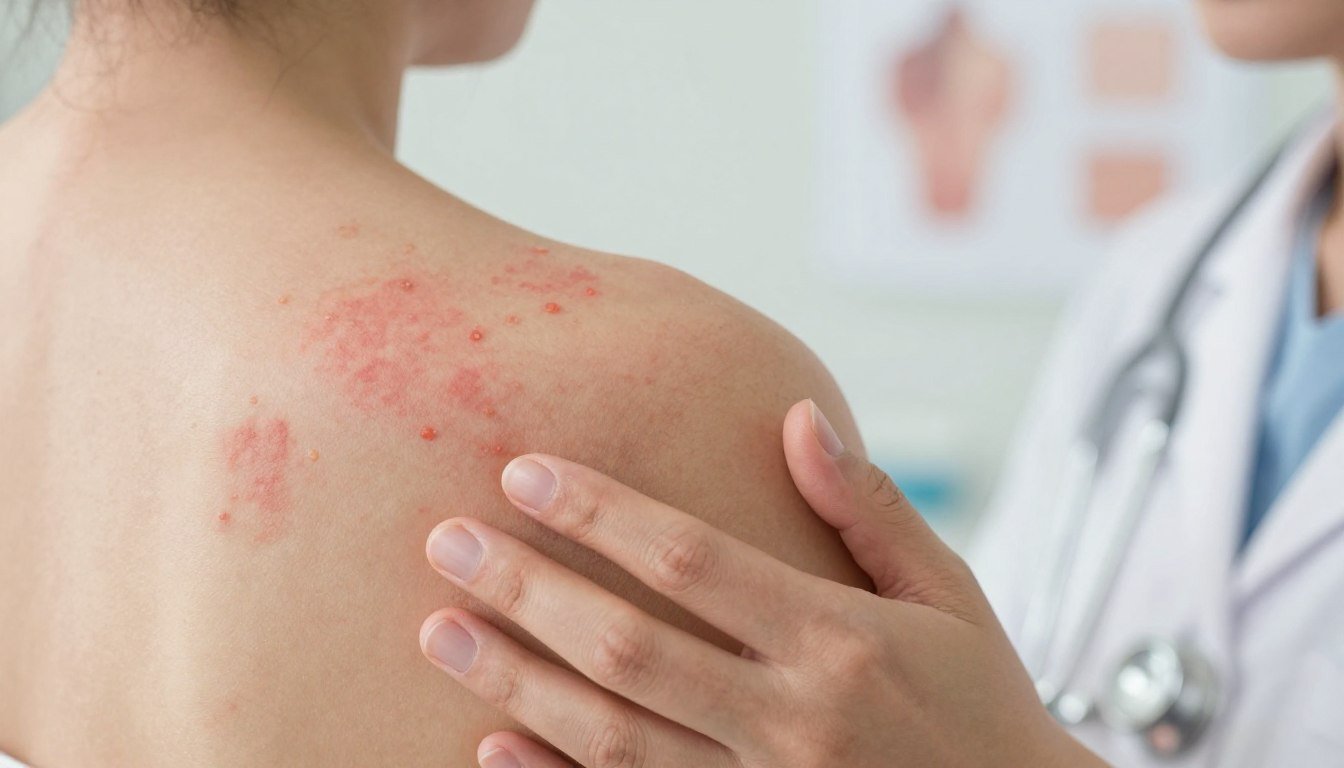
Have you ever wondered why a simple itch can turn into a flare that affects daily life? This common skin condition can feel unfair and confusing, yet understanding it helps you take control.
We explain atopic dermatitis as a chronic problem where the skin barrier weakens, causing dry, itchy skin and visible inflammation. The cycle of scratching often makes the rash worse, which is why people call it the “itch that rashes.”
Genetic factors and environmental triggers such as allergens, irritants, stress, and infections shape how this condition appears. Proper care blends daily skincare with medical oversight and tailored treatments.
Dr. Varsha D.V at Boss Multispeciality Hospital, Bangalore, helps patients identify triggers and set realistic treatment plans. With steady care, many adults and children can reduce flare-ups and protect their skin long term.
Understanding What Is Eczema
A weakened skin barrier lets moisture escape and invites irritation, leading to persistent redness and itching.
Atopic Dermatitis Explained
Atopic dermatitis is the most common type of this condition and causes chronic inflammation and dry skin. Genetic changes, especially in the filaggrin gene (FLG), reduce barrier strength.
Patients often have fewer beta-defensins, which lowers natural skin defenses and raises infection risk.
The Skin Barrier Function
The skin barrier is the outermost protective layer that keeps moisture in and blocks allergens and irritants.
- When the barrier fails, water loss makes dry skin and flares more likely.
- Allergens and irritants then penetrate more easily, worsening symptoms.
- Many adults need tailored care to break the cycle of dryness and scratching.
At Boss Multispeciality Hospital, Bangalore, we focus on restoring the skin barrier to improve long-term skin health and comfort for people living with this condition.
The Role of Genetics and Environment
Family history and daily exposures often shape how this skin condition appears across generations.
Genetic links include a family history of asthma, hay fever, and allergies. Mutations in the filaggrin gene weaken the skin barrier. This makes the skin more prone to irritation and inflammation.
Environmental triggers vary. Dust mites, pet dander, and some foods can prompt flare-ups. The immune system in many people with atopic dermatitis reacts too strongly to common allergens.
Stress also plays a clear role. Chronic stress can worsen symptoms for children and adults. We use this understanding to tailor care plans at Boss Multispeciality Hospital, Bangalore.
- Identify family risks and household triggers.
- Reduce exposure to known allergens where possible.
- Address stress and support the immune response with guidance.
| Factor | Typical effect | Action |
|---|---|---|
| Genetic (family, asthma) | Higher sensitivity, weaker barrier | Personalized management and monitoring |
| Environmental (dust, pets) | Trigger inflammation and symptoms | Allergen reduction and avoidance |
| Stress and lifestyle | Worsens flares and immune response | Stress reduction and supportive care |
Common Symptoms and Physical Signs
Skin changes may look different by age and tone, yet they share common warning signs we watch for.
Age-related patterns
Infants often develop lesions on the cheeks and face. These early signs help guide an early diagnosis.
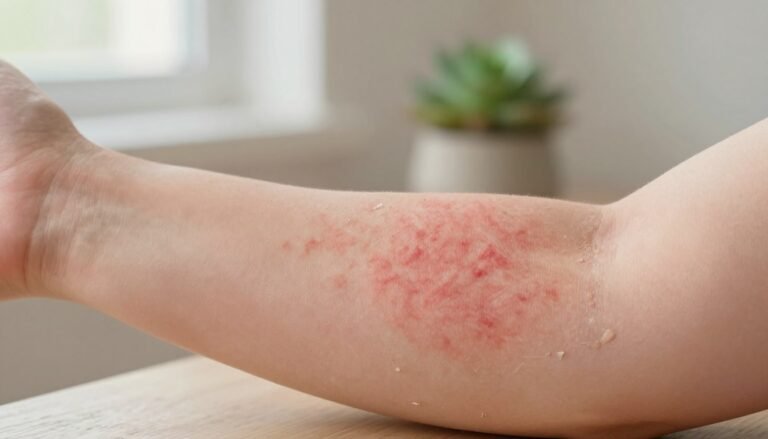
School-aged children more commonly show involvement at flexural surfaces such as the anticubital and popliteal fossae. These areas include the creases behind the knees and the inner elbows.
Variations by skin tone
People with darker skin may have purple, grey, or brown patches rather than bright red inflammation. Clinicians must read these subtle cues to avoid missed or delayed diagnosis.
Dennie‑Morgan lines (creases below the lower eyelid) and the allergic salute (a transverse crease across the nose) are classic signs we evaluate during examination.
- Common eczema symptoms include dry, itchy patches that appear in the creases of the elbows and behind the knees.
- Recognizing these signs early helps prevent progression and manage discomfort.
- Our dermatologists at Boss Multispeciality Hospital, Bangalore, are trained to spot varied presentations of this type eczema for accurate care.
| Age group | Typical locations | Key sign |
|---|---|---|
| Infants | Cheeks, face | Localized lesions |
| Children | Inner elbows, behind knees | Flexural rash |
| All ages | Hands, neck, eyelids | Dryness and itch |
Identifying Your Personal Triggers
Triggers often hide in plain sight — from a new soap to a warm afternoon — and spark sudden flares.
Start by noting daily exposures that precede a flare. Common irritants include harsh soaps, detergents, solvents and fragranced products. Contact with these can cause contact dermatitis in sensitive skin.
Allergens such as dust mites, pet dander and certain foods (peanuts, milk, soy) also play a strong role. We help patients track suspected food allergies and environmental allergens so you can test and reduce risks.

- Avoid overheating and heavy sweating during activity when possible.
- Manage stress with simple routines; stress often worsens symptoms.
- Watch for signs of infection and seek care early to stop worsening.
| Trigger | Typical effect | Quick action |
|---|---|---|
| Soaps & fragrances | Immediate irritation or delayed rash | Switch to fragrance-free products |
| Dust mites & pet dander | Repeated flares at home | Allergen reduction, cleaning, covers |
| Food allergies | Systemic flare or localized rash | Track intake, consult for testing |
Every person has a unique mix of triggers. We guide you through tracking and choosing gentle products to limit flare-ups and protect the skin long term.
The Scratch and Itch Cycle
An urge to rub or scratch may seem small, but it often fuels ongoing skin damage. Scratching breaks the surface, which increases inflammation and leads to more itching.
That repeated loop drives many eczema symptoms and can change how the skin looks and feels over time. Chronic scratching causes lichenification — thick, leathery patches that take longer to heal.
Nighttime itching is common and harms sleep. Poor sleep worsens daytime stress, which can make flares more likely for people already coping with this condition.
- Scratching increases inflammation and delays recovery.
- Good night routines help reduce itching and protect sleep.
- Breaking the cycle is central to our treatment plan at Boss Multispeciality Hospital, Bangalore.
| Issue | Effect | Action |
|---|---|---|
| Night itching | Sleep loss | Moisturize at bedtime; cool bedroom |
| Chronic scratching | Lichenification | Anti-inflammatory care; behavioral strategies |
| Ongoing inflammation | Worse symptoms | Targeted medical treatment |
Diagnostic Approaches for Skin Conditions
Accurate diagnosis starts with a careful review of your history and a close look at affected skin.
We usually make a clinical diagnosis for atopic dermatitis and related rashes by comparing the appearance of the lesion with your medical history. Routine blood tests are rarely needed for standard cases.
If signs are unclear, we may suggest allergy testing or patch testing to identify contact triggers. These tests help target treatments and reduce repeat flares.
- A clinical exam and history form the core of diagnosis.
- Allergy or patch testing helps when triggers are uncertain.
- Referral to a dermatologist is advised for severe or atypical presentations.
| Step | Purpose | Typical outcome |
|---|---|---|
| History & exam | Identify pattern and triggers | Clinical diagnosis, initial plan |
| Allergy/patch tests | Detect contact allergens | Targeted avoidance and treatments |
| Specialist referral | Complex or treatment‑resistant cases | Advanced care and tailored plan |
We believe an accurate diagnosis gives you the best chance for effective treatment. Our team at Boss Multispeciality Hospital, Bangalore, uses a stepwise method so you get clear answers and a practical plan.
Daily Skincare and Moisturizing Routines
A steady moisturizing routine helps skin stay resilient between episodes.
Moisturize at least two times each day to protect the skin barrier and reduce symptoms. Use thick, fragrance-free ointments rather than light creams for better moisture retention.
Avoid products with perfumes, dyes, or harsh chemical additives. Gentle, simple products lower the risk from common allergens and triggers.
- Apply an ointment after bathing while skin is damp to lock in moisture.
- Keep a small jar of ointment for hands and another for body use.
- Moisturize even when skin looks healthy to maintain the barrier and prevent flare-ups.
- Manage stress and follow gentle product advice as part of daily care.
| Routine step | Why it helps | Practical tip |
|---|---|---|
| Twice-daily moisturizing | Seals in hydration and soothes dry patches | Morning and bedtime applications |
| Use thick ointments | Higher oil content prevents water loss | Choose fragrance-free, preservative-light products |
| Avoid irritants | Reduces contact flares from allergens and chemicals | Test products on a small area first |
We offer personalized advice at Boss Multispeciality Hospital, Bangalore, to match products and treatment plans to your needs. Lifelong daily care helps many people keep skin comfortable and steady.
Medical Treatments for Flare Ups
Effective care for active flares aims to calm inflammation and protect the skin barrier. We tailor choices to the area affected, age, and severity so you get relief with safety in mind.

Topical Steroids
Topical steroids provide fast control of red, itchy lesions. Use them exactly as prescribed; short courses reduce flare intensity without daily long‑term use.
Possible side effects include skin thinning and rebound dermatitis if applied too often or stopped suddenly.
Non-Steroidal Alternatives
Pimecrolimus and tacrolimus offer steroid-free options for long‑term care or for sensitive areas. These products modulate the immune system locally to lower inflammation.
- Cold compresses soothe itching and lessen immediate discomfort.
- Oral antihistamines at bedtime can improve sleep during severe flares.
- We monitor progress and adjust treatments to limit side effects and protect skin.
| Treatment | Used for | Notes |
|---|---|---|
| Topical steroids | Acute flares | Short courses; watch for thinning, rebound |
| Pimecrolimus / Tacrolimus | Long‑term control | Good for sensitive sites; steroid‑sparing |
| Supportive care | Itching, sleep loss | Cold compresses, antihistamines at night |
At Boss Multispeciality Hospital, Bangalore, we guide you through safe use and follow up to keep flares brief and skin healthy.
Managing Severe Eczema Cases
Severe flare-ups demand coordinated care beyond creams and short courses of treatment.
We may use systemic therapies when inflammation remains uncontrolled. Oral or injectable medicines target the immune system to reduce widespread symptoms and protect the skin barrier.
Specialized dressings, such as wet wraps, help cool, rehydrate, and protect fragile areas like the elbows and folds. These techniques speed healing and lower the urge to scratch.
People with severe dermatitis face higher infection risk. Our team watches for signs such as blisters, spreading redness, or fever and treats infections promptly to prevent complications.
- We combine systemic treatments with skin care and trigger management.
- Wet dressings support barrier repair and ease acute discomfort.
- Interprofessional care — dermatology, allergy, and nursing — improves outcomes and life quality.
| Issue | Approach | Goal |
|---|---|---|
| Widespread inflammation | Systemic therapy (oral/injectable) | Reduce symptoms and immune overactivity |
| Broken skin or blisters | Wet dressings and infection control | Promote healing and prevent complications |
| Poor quality of life | Multidisciplinary support and trigger management | Restore daily function and sleep |
Potential Complications and Infections
Some infections begin subtly but progress rapidly in people with fragile skin. Early recognition helps avoid severe outcomes and guides prompt treatment.
Recognizing Eczema Herpeticum
Eczema herpeticum is a serious viral infection caused by herpes simplex virus‑1. It can present with sudden clusters of painful blisters and fever. We advise urgent assessment when you see rapid spread or systemic symptoms.
Patients with atopic dermatitis are more prone to bacterial infections such as Staphylococcus aureus. Eczema also raises the risk of viral infections like eczema coxsackie, which may mimic herpeticum.
- Watch for clusters of blisters, fever, increasing pain, or new pus — these may signal infection.
- Left untreated, infections can lead to secondary bacterial sepsis or, rarely, meningitis.
- If you suspect infection, seek immediate care at Boss Multispeciality Hospital, Bangalore.
| Infection | Typical signs | Urgent action |
|---|---|---|
| Eczema herpeticum | Rapid blisters, fever, pain | Immediate antiviral therapy and referral |
| Staphylococcal infection | Pus, warmth, localized redness | Antibiotics and wound care |
| Eczema coxsackie | Vesicles that resemble herpeticum | Clinical testing and supportive care |
We educate people on signs of complications and provide fast, evidence‑based care. Our team at Boss Multispeciality Hospital, Bangalore, has experience diagnosing and treating these serious problems to protect long‑term skin health.
Expert Dermatological Care at Boss Multispeciality Hospital
At Boss Multispeciality Hospital we combine clinical experience with modern therapies to help people regain comfortable skin.
Dr. Varsha D.V, a Consultant Dermatologist & Dermatosurgeon, leads a team that offers focused care for severe eczema and other complex skin conditions.
We design treatment plans that suit your age, skin type, and daily life. Our approach blends medical treatments, barrier repair, and practical advice to reduce flares and improve quality of life.
Consult Dr. Varsha at Boss Multispeciality Hospital, Bangalore — Call +91 9986607601 to Book an Appointment
- Individual assessment and evidence-based treatments tailored to you.
- Advanced options for persistent or widespread disease managed safely.
- Compassionate follow-up and patient education for long-term skin health.
- Easy appointment booking by phone for timely care and review.
| Service | Benefit | Typical goal |
|---|---|---|
| Specialist consultation | Accurate diagnosis and personalised plan | Reduce flares and prevent complications |
| Advanced medical treatments | Targeted control of inflammation | Improve skin function and comfort |
| Ongoing support | Education, follow-up, and lifestyle guidance | Long-term maintenance and better daily life |
Conclusion
Simple, consistent habits make managing this skin condition easier over time. We encourage steady daily care and practical steps to protect skin and reduce flare-ups.
Learn your triggers and note any allergens that raise itching or dry skin. Early diagnosis and prompt action cut flare length and lessen symptoms eczema people often face.
Effective treatment and suitable products help most people heal and stay comfortable. If your symptoms persist, call Boss Multispeciality Hospital, Bangalore to book a consultation with Dr. Varsha D.V. We will work with you to build a personalised plan and support every person on this journey.