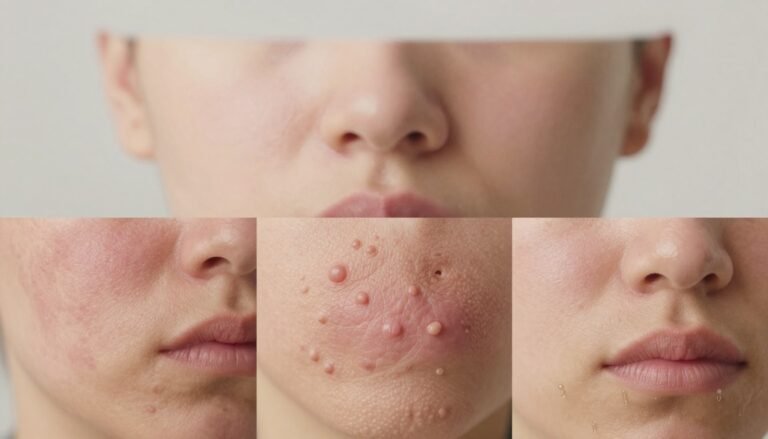
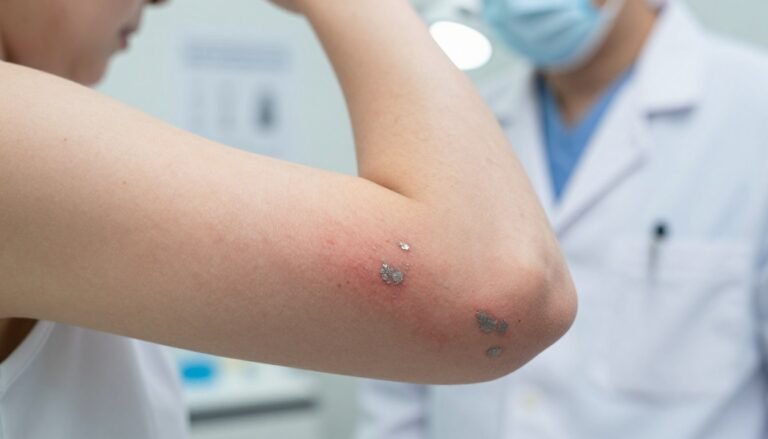
What Triggers Eczema Flare-Ups & How to Avoid Them
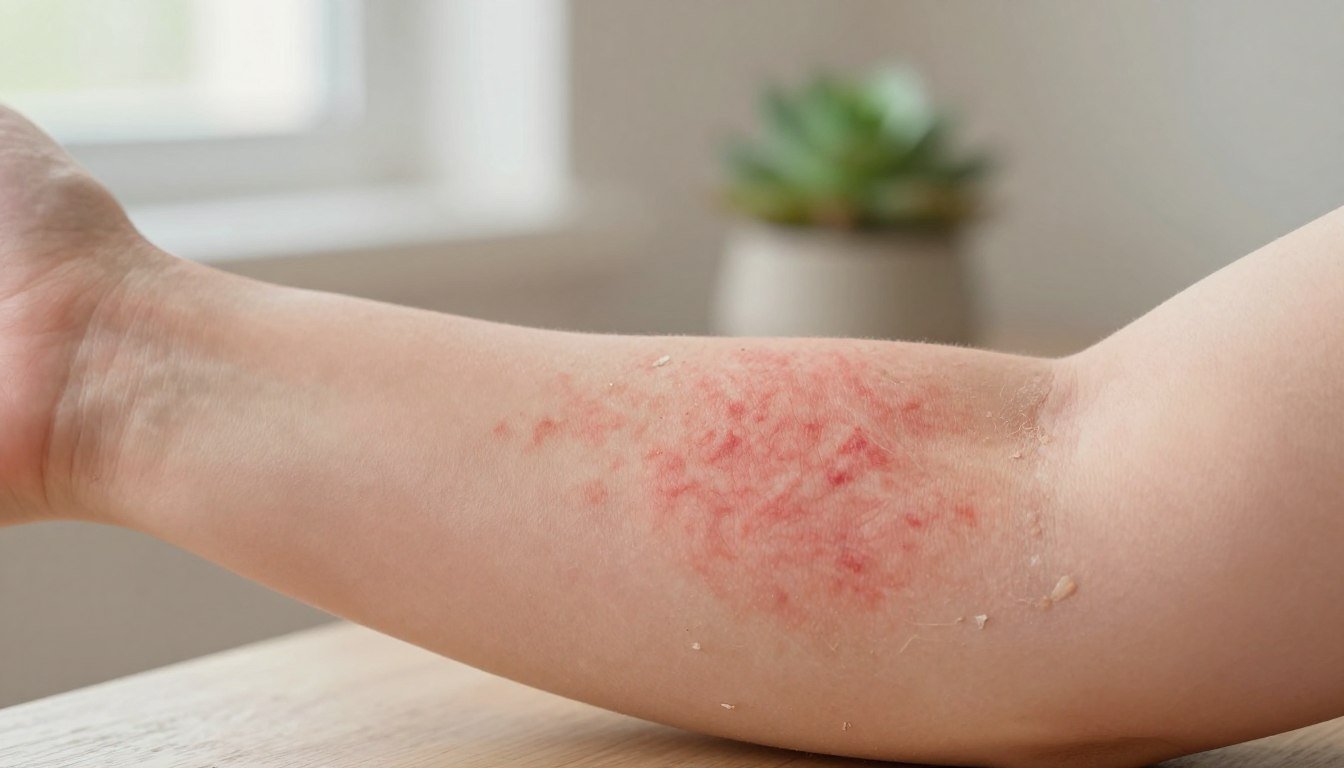
Have you ever wondered why a small change in routine can set off long nights of itching and discomfort?
We know that living with eczema feels unpredictable. Understanding the complex nature of eczema flare-ups is the first step toward reclaiming comfort for your sensitive skin.
In this article, we offer clear, evidence-based insights into what causes episode events and how to protect your skin barrier. We focus on practical steps you can try at home and decisions to discuss with your dermatologist in Bangalore.
Managing this chronic condition needs a proactive approach. By spotting early warning signs, you can shorten an eczema flare-up and reduce its intensity.
We aim to guide you with simple, trustworthy advice so you feel more confident caring for your skin day to day.
Understanding Eczema and Its Impact
Understanding early signs helps you act quickly when your skin begins to change. We explain how the cycle of itching works and what to watch for so you can protect your skin barrier.
The Scratch-Itch Cycle
The scratch-itch cycle starts when irritants or allergens set off skin chemicals that make you itch. Scratching gives short relief but releases more inflammation, which increases the urge to scratch again.
Recognizing Early Symptoms
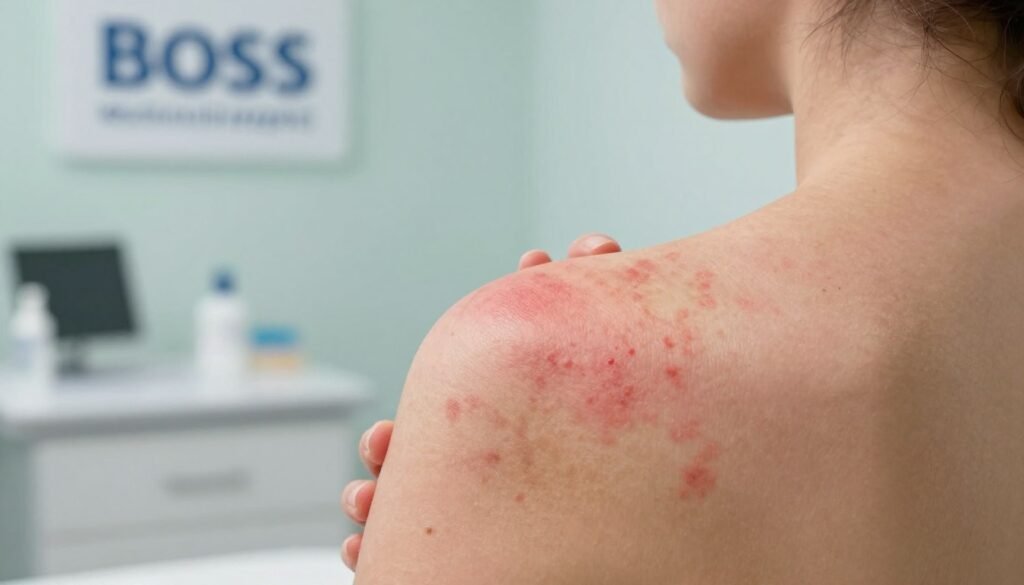
Atopic dermatitis, often called dermatitis in medical notes, usually begins with dry skin or small patches of redness. These early symptoms can appear over time and vary by age and location on the body.
- Chronic dry skin that flakes or feels tight.
- Patches of discolored or inflamed skin that grow in a few days.
- Different types of irritation—itching, burning, or stinging—help point to the right care.
Knowing the common causes eczema and spotting symptoms early gives you a better chance to reduce an eczema flare and choose the right treatment with your dermatologist.
Common Eczema Flare Up Triggers
Common everyday factors often start a chain reaction that worsens sensitive skin. Researchers link environmental, dietary, immune, and emotional causes to worsening symptoms.
Identifying your unique eczema flare up triggers is vital for long-term control. Many people find external factors make their condition worse, and a single episode often has multiple causes.
- Environmental allergens such as dust, pollen, and pet dander.
- Diet and food sensitivities that vary from person to person.
- Immune responses and skin barrier changes that cause inflammation.
- Stress and sleep loss that amplify symptoms and scratching cycles.
By tracking daily habits and symptom patterns, you learn which factors most often lead to an eczema flare-up. That makes it easier to build a practical care plan with your dermatologist and reduce episodes over time.
The Role of Environmental Allergens
Invisible allergens in the room may slowly damage the skin’s barrier and raise irritation. Common airborne allergens include pollen, pet dander, dust, mold, smoke, and pollution, all of which can worsen sensitive skin over time.
Common Airborne Irritants
Contact with irritating chemicals in everyday items may include detergents, fragranced soaps, dyes, and certain metals. These chemicals can strip oils and increase water loss through the skin.
- Environmental allergens are significant triggers for many people because they weaken the skin barrier and raise transepidermal water loss.
- Cleaning your home regularly and limiting carpets or heavy upholstery can help reduce airborne irritants.
- Choosing skincare products free from fragrances and dyes avoids common chemicals that irritate skin.
- Some people react to metals such as nickel or gold when they touch the skin directly.
- Keeping your home properly humidified can help reduce the impact of allergens and protect sensitive skin.
How Emotional Stress Affects Skin Health
Stress does more than affect mood — it can alter immune signals and weaken the skin barrier. A 2023 study found that stress may trigger or worsen eczema symptoms by changing immune responses and barrier function.
Chronic stress may also influence your immune system and spark inflammation in the skin. When cortisol rises during long periods of tension, you may notice worse itching and redness.
We recommend simple, proven steps to help you take control. Regular exercise, yoga, or short meditation sessions reduce stress and can lower the chance of an eczema flare-up.
- Prioritize quality sleep and set a calm bedtime routine.
- Talk with friends, family, or a therapist to ease emotional burden.
- Try gentle breathing exercises during high-stress moments.
| Stress Action | Effect on Skin | Quick Tip |
|---|---|---|
| Short-term tension | Temporary redness or itch | Deep breaths for 2 minutes |
| Chronic stress | Weakened barrier, more inflammation | Daily walk, 30 minutes |
| Poor sleep | Higher cortisol, worse symptoms | Fix sleep schedule, avoid screens |
By keeping stress in check, you can often reduce the frequency of eczema flare-ups and improve your overall skin health. If stress feels unmanageable, we encourage you to seek professional help so you get both emotional and dermatologic care.
Managing Dietary Factors and Food Sensitivities
Many people notice that certain meals make their symptoms worse within hours or days. Diet can affect skin health, so it pays to watch how you and your children respond after eating.
Identifying Trigger Foods
A large 2023 study of 225,568 people found nearly half reported a food sensitivity and over a third had a food allergy. The common list includes peanuts, tree nuts, sesame, cow’s milk, eggs, soy, wheat, seafood, and shellfish.
While food allergies are more common in children, adults can also notice that certain foods worsen eczema symptoms. Keeping a simple food diary helps you spot patterns without guesswork.
When to See an Allergist
If you suspect a food link, consult a doctor or an allergist for formal testing. Tests and guided elimination diets protect nutrition and avoid unnecessary restrictions.
Identifying personal trigger foods can help manage the condition, but diet alone rarely cures it. Work with your care team so you get safe, effective advice tailored to you or your child.
Impact of Weather and Temperature Changes
Weather that swings between hot and cold can make managing sensitive skin more difficult. Cold, dry air often steals moisture and leaves the surface brittle. Hot, humid days can make you sweat more and invite irritants to bother your skin.

Extreme weather changes are common causes that can trigger an eczema flare-up. Many people notice symptoms shift with the seasons, so routine tweaks matter.
- In winter time, run a humidifier at home to add moisture and protect the barrier.
- If you sweat easily, choose loose, breathable clothes and pause during hard exercise.
- Take a cool shower after activity to rinse sweat and calm inflammation.
- Adjust your moisturiser and clothing choices as the weather changes to reduce irritation.
We recommend tracking how different weather patterns affect you. Small adjustments at home often reduce symptoms and help you stay comfortable year-round.
Hormonal Fluctuations and Skin Sensitivity
Hormone shifts across the month can change how your skin feels and reacts.
Changes in estrogen, progesterone, testosterone, insulin, and cortisol can affect eczema and the way your body shows symptoms. These shifts may also make the barrier more fragile and raise itch or redness.
Many people notice worse discomfort during menstruation or menopause. We know these times are a natural part of life, yet they can make caring for sensitive skin harder.
Keeping a simple symptom diary helps you and your provider spot patterns tied to your cycle. Gentle, consistent skin care during these windows helps protect the barrier and reduce irritation.
| Hormone | Common effect on skin | Quick care tip |
|---|---|---|
| Estrogen | Can affect moisture and elasticity | Use fragrance-free moisturiser daily |
| Cortisol | Linked to more inflammation and itch | Manage stress; try short breathing breaks |
| Insulin/Testosterone | May alter oiliness and irritation | Maintain balanced diet; see clinician if severe |
Preventing Infections in Compromised Skin
When broken skin meets common bacteria, a simple scratch can become a serious infection. Staphylococcus aureus is the most common culprit in people with eczema and often worsens symptoms fast.
Signs of Bacterial or Viral Infection
If the affected area grows more red, discoloured, or starts to ooze fluid, these are warning signs. You may also see crusting, increased pain, or spreading warmth around the sore.
- When your skin barrier is compromised, it can become a site for bacterial or viral infection; signs may include oozing or crusting.
- If you notice infection signs, see a doctor promptly to get the right treatment and prevent complications.
- At home, help reduce risk by keeping the area clean and avoiding scratching open sores.
- Common treatments often involve prescribed antibiotics or medicated soaks to restore the surface and reduce bacteria.
- Monitor changes closely — early care is the best way to protect your overall health and manage worsening symptoms.
| Sign | What it may mean | Immediate action |
|---|---|---|
| Increased redness or warmth | Possible bacterial infection (eg. Staphylococcus) | Contact your doctor; avoid self-applied steroids on raw skin |
| Oozing or yellow crusting | Active infection that may spread | Keep clean; seek prescription antibiotics or soaks |
| Sudden pain or fever | Systemic response; needs urgent review | See a clinician promptly for assessment and treatments |
We encourage people to watch for signs and act early. Prompt attention helps reduce complications and keeps the skin healthier long term.
Professional Care at Boss Multispeciality Hospital
When skin concerns persist despite home care, expert medical support can make a meaningful difference. At Boss Multispeciality Hospital, Bangalore, we offer a calm, evidence-based approach to help you find lasting relief.
Expert Guidance from Dr. Varsha D.V
- We provide comprehensive care for patients facing persistent eczema flare-ups and other chronic conditions.
- Dr. Varsha D.V, MBBS, DDVL, is a Consultant Dermatologist & Dermatosurgeon who listens closely and guides treatment decisions.
- Our team designs personalised plans that combine medical treatments and practical daily care to help manage symptoms.
- We believe every patient deserves a doctor who explains options clearly and supports a steady path to healthier, more comfortable skin.
- You can rely on Boss Multispeciality Hospital, Bangalore, for professional follow-up and coordinated care when needed.
If you would like a consultation with Dr. Varsha or want to learn about available treatments, we are here to help. Contact our clinic to schedule an appointment and discuss a plan that fits your life and needs.
Conclusion
Small, consistent changes often make a big difference for sensitive skin. We know managing a chronic skin condition takes patience and time.
Identify what affects you as a person and work with a clinician to build a steady routine. Simple steps protect the barrier, reduce discomfort, and help prevent a flare.
If you seek medical support, a doctor can offer targeted treatment and personalised advice. We are here to help you understand what can cause eczema and which treatments suit your needs.
Ready to take the next step? Consult Dr. Varsha at Boss Multispeciality Hospital, Bangalore — Call +91 9986607601 to Book an Appointment.