Melasma vs Hyperpigmentation: What’s the Difference?

Have you ever wondered why some dark patches on your face fade while others linger despite sunscreen and creams?
We see many patients in Bangalore who use the words interchangeably. Understanding the difference helps you pick the right treatment and avoid wasted time.
At our clinic, we explain that one term names a specific condition tied to hormones and pregnancy, while the other covers many types of pigment changes caused by sun exposure, acne, or inflammation.
Both involve melanin production, but triggers and areas affected often differ. That matters when choosing topical creams like hydroquinone, sunscreen habits, or laser options.
We aim to help you identify whether your dark spots are post-inflammatory changes, a hormonal mask, or another cause. Knowing the cause guides safe, evidence-based care and restores confidence in your skin tone.
Understanding Skin Discoloration
When your skin shows new patches of color, the cause may be simple or require targeted care. Melanin is the pigment that gives your skin its natural tone, and increased production can create darker spots on the face or body.
Many patients notice darker areas after acne or injury. Post-inflammatory hyperpigmentation happens when inflammation heals and leaves a darker mark behind.
It is important to tell general hyperpigmentation apart from melasma. Some types link to hormones or pregnancy and need tailored treatments. Other patches follow sun exposure, acne, or irritation and respond to different approaches.
We identify triggers to guide care. By addressing melanin production and the root cause, we can recommend safe, effective options that fit your lifestyle and skin type.
| Feature | Common Causes | Typical Areas |
|---|---|---|
| Post-inflammatory pigmentation | Acne, cuts, irritation, inflammation | Face, body areas with injury |
| Hormonal pigmentation | Pregnancy, hormonal changes | Cheeks, forehead, upper lip |
| Sun-related pigmentation | Sun exposure, UV damage | Face, hands, shoulders |
Defining Melasma vs Hyperpigmentation
Not all darker areas on your skin are the same. We first look at signs and triggers to plan care that fits your skin tone and lifestyle.
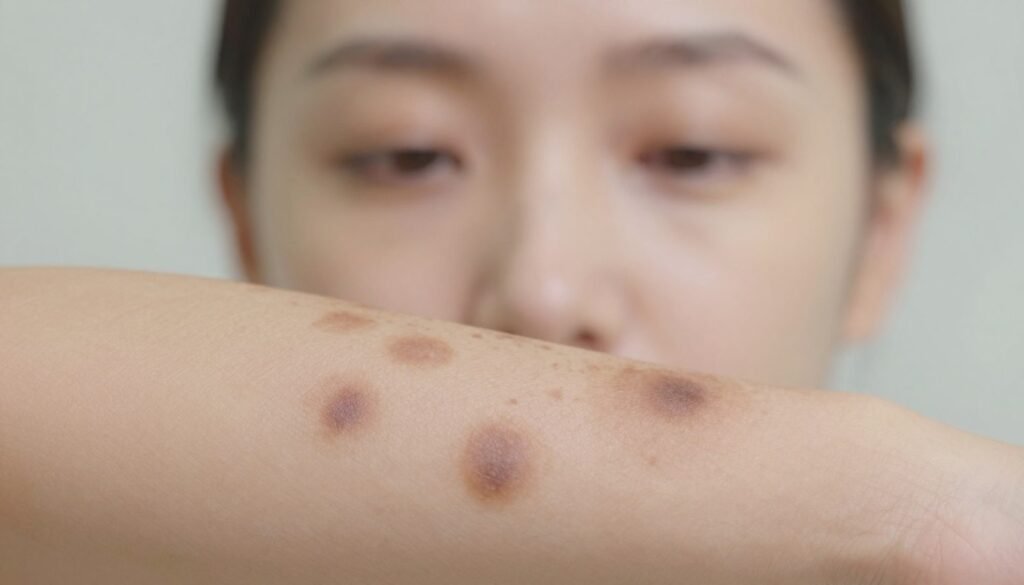
What is Hyperpigmentation
Hyperpigmentation is a broad skin condition where dark spots appear from increased melanin production.
It can follow acne, injury, inflammation, or sun exposure. It may show up on any body area and affects many skin tones.
Understanding Melasma
Melasma is a specific type of pigmentation tied to hormonal changes and often called the “mask of pregnancy”.
It commonly appears as symmetric patches on the cheeks, forehead, and upper lip. Women aged 20 to 40 are at higher risk.
- Sun exposure and genetics influence how pigment shows across skin tones.
- Post-inflammatory hyperpigmentation often follows acne or skin injury.
- Accurate diagnosis guides the right treatments and safe follow-up care.
| Type | Common Triggers | Typical Areas |
|---|---|---|
| General hyperpigmentation | Acne, inflammation, UV exposure | Face, hands, body |
| Melasma | Hormonal changes, pregnancy, sun | Cheeks, forehead, upper lip |
| Post-inflammatory | Injury, acne, procedures | Sites of prior inflammation |
Key Differences in Appearance and Patterns
How pigment arranges across your face—symmetrical or scattered—tells us a lot about the cause.
Melasma often forms broad, symmetrical patches across both cheeks, the forehead, or the nose. These even areas of darker skin usually reflect hormonal influence and concentrate on the face.
Other types of hyperpigmentation tend to appear as isolated dark spots. These spots can result from acne, injury, or sun exposure and may show up anywhere on the body.
- Symmetry: melasma shows even patches across the cheeks and forehead.
- Distribution: hyperpigmentation appears as scattered spots or localized marks.
- Triggers: hormonal shifts for melasma; acne and sun for other pigmentation.
- Diagnosis: visual pattern guides our choice of treatments and follow-up.
| Feature | Melasma | Other pigmentation |
|---|---|---|
| Pattern | Symmetrical broad patches | Isolated or uneven spots |
| Common triggers | Hormonal changes, pregnancy | Acne, inflammation, sun exposure |
| Typical areas | Cheeks, forehead, upper lip | Face, hands, body sites of injury |
Common Triggers and Underlying Causes
Many factors trigger uneven pigment, and knowing them helps us prevent new patches. We assess each cause to design care that fits your skin and daily life.

Hormonal Fluctuations
Hormone shifts are a major trigger, especially during pregnancy or when using birth control. Increased estrogen and progesterone boost pigment production in some women.
We note family history, since about 33–50% of people with this condition have relatives affected. That background helps us predict risk and plan safe treatments.
Sun Exposure and UV Damage
UV rays prompt the skin to make more melanin as a defense. Regular sun exposure worsens both long-standing and new dark areas.
Daily sun protection reduces flare-ups and supports any medical treatment you choose.
Genetic and Environmental Factors
Genetics, medications, heat, and inflammation from acne all shape how pigment shows on the body. Certain antibiotics or antidepressants can also trigger unwanted dark spots.
We review your medical history and lifestyle to control these factors and reduce recurrence.
| Trigger | How it acts | What to watch for |
|---|---|---|
| Hormonal fluctuations | Increases pigment production | Symmetric facial patches; recent pregnancy or contraceptive use |
| Sun exposure | Stimulates melanin, darkens existing spots | Worsening on face, hands, or other exposed areas |
| Inflammation & medications | Post-inflammatory pigmentation; drug-induced pigment | Dark marks after acne or new medicines |
By managing these triggers together, we help you protect your skin, reduce new pigment, and choose the right treatment plan for lasting results.
Professional Treatment Options for Pigmentation
Expert evaluation helps match your pigment pattern with evidence-based therapies for lasting improvement. We review medical history, sun habits, and prior treatments before recommending a plan.
Clinical Procedures and Topical Therapies
We offer a range of professional options to reduce persistent dark spots and even your skin tone. Topical creams such as hydroquinone are used when appropriate to slow melanin production and lighten marks over weeks.
- Laser therapy targets deeper pigment and can also stimulate collagen for smoother skin.
- Chemical peels remove the top damaged layer to reveal fresher skin and reduce visible spots.
- We counsel on medications and skincare to avoid interactions and protect results.
- Daily sun protection is essential to prevent recurrence after any treatment.
| Option | Best for | Recovery |
|---|---|---|
| Topical creams (hydroquinone) | Superficial pigment, maintenance | Minimal; weeks of use |
| Chemical peels | Surface discoloration, texture | Days to a week |
| Laser therapy | Deep or stubborn pigmentation | Variable; clinic follow-up |
We tailor treatments to the causes we identify. Our goal is safe, steady improvement and a plan that fits your lifestyle in India’s climate and sun exposure.
Preventive Measures for Clearer Skin
A few steady steps each day help keep your skin even and reduce the need for future treatments.
Use a broad-spectrum sunscreen with SPF 30 or higher every morning. Reapply during long outdoor hours to lower the risk of sun-induced pigmentation and new dark spots.
Avoid prolonged sun exposure during peak hours. Wear a wide-brim hat and seek shade when UV levels are highest to protect fragile areas prone to patches.
Include gentle, dermatologist-recommended creams in your daily routine. For those prone to melasma, tinted sunscreens add protection against visible light from screens as well as UV rays.
Regular skin check-ups let us track progress and adjust preventive measures early. In some cases, periodic laser sessions can help maintain an even tone and address early signs of hyperpigmentation.
- Daily SPF and reapplication
- Avoid peak sun hours and use physical barriers
- Consistent creams and follow-up with your dermatologist
| Measure | Why it helps | Ideal frequency |
|---|---|---|
| Sunscreen (SPF ≥30) | Prevents UV-triggered pigment darkening | Daily, reapply every 2–3 hours outdoors |
| Gentle topical creams | Maintains skin barrier and evens tone | Daily, as advised by dermatologist |
| Clinic follow-up / Laser | Monitors progress and treats early patches | Every 3–6 months or as recommended |
Expert Care at Boss Multispeciality Hospital
Targeted medical care helps address persistent facial patches that resist over-the-counter creams. At Boss Multispeciality Hospital, Bangalore, we combine clinical experience with patient-centered plans to treat stubborn dark spots and uneven skin tone.
Consultation with Dr. Varsha D.V.
Dr. Varsha D.V (MBBS, DDVL) is a Consultant Dermatologist & Dermatosurgeon who evaluates complex cases of melasma and hyperpigmentation. She focuses on clear diagnosis, explaining how hormones, sun, and inflammation shape your skin.
We offer personalized treatment options, from medical-grade creams like hydroquinone to procedural choices such as laser therapy. Every plan includes sunscreen guidance and follow-up to protect results.
| Service | Best for | Note |
|---|---|---|
| Topical therapy | Superficial spots | Medical supervision advised |
| Chemical peels | Surface unevenness | Short recovery |
| Laser | Stubborn patches | Requires clinic follow-up |
We invite you to book a professional evaluation to explore the best treatment options for your specific concerns. Consult Dr. Varsha at Boss Multispeciality Hospital, Bangalore — Call +91 9986607601 to Book an Appointment.
Conclusion
Knowing the exact cause of dark spots makes choosing the right treatment options much simpler.
Distinguishing this skin condition lets us tailor treatments to your skin and lifestyle. Both melasma and the broader pigmentation that follows acne or sun can improve with medical care.
Protecting your skin daily and using a personalised routine helps keep results steady. Seek expert advice so you avoid harmful self-treatment and get safe, effective options.
We are here to guide you through causes, treatment choices, and follow-up to restore an even skin tone. Contact our clinic for a careful assessment and a plan that fits you.