When Should You See a Dermatologist for Eczema or Psoriasis?
Are mild flares just an annoyance, or do they signal a deeper problem that needs expert care?
We know living with chronic skin conditions can feel exhausting. If over-the-counter creams no longer help, you may face worsening symptoms, sleep loss, or infection risk.
Our goal is practical. We explain how to tell if home remedies are enough or if a doctor’s evaluation is needed. You will learn which triggers and factors commonly drive persistent inflammation and which signs suggest a more serious condition.
This short guide helps patients in Bangalore and beyond make informed choices about skin health. You will find clear cues about timing, treatments, and realistic care steps. We aim to ease worry and point you toward effective, evidence-based options that protect long-term skin health.
Understanding the Differences Between Eczema and Psoriasis
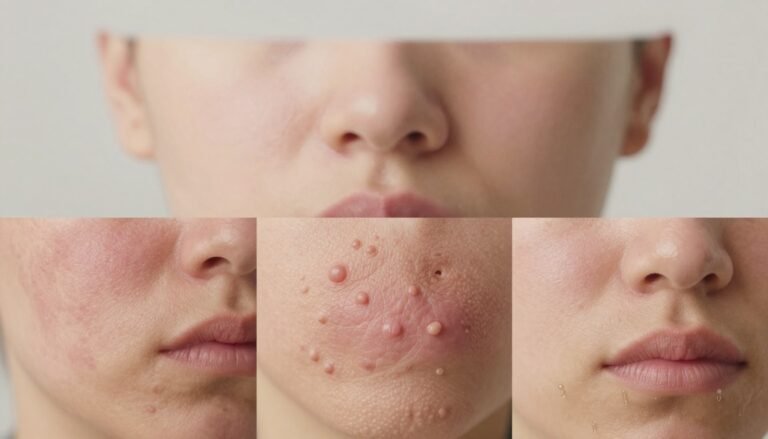
Many people confuse red, itchy skin patches and miss key clues that point to two different conditions. We’ll outline clear, simple signs so you can recognise likely causes and discuss options with your care team.
Key Symptoms of Eczema
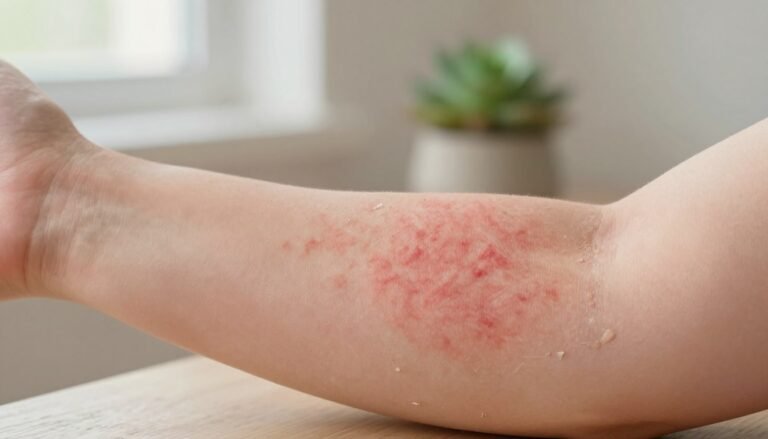
Eczema is a common skin condition that affects far more people than some other disorders. It often appears on the inner elbows or behind the knees and causes dry, itchy patches.
Atopic dermatitis is the most frequent form, marked by intense inflammation and a tendency to flare with lack of moisture. Stress and environmental triggers often make symptoms worse.
Identifying Psoriasis Plaques
Psoriasis is a distinct disease in which skin cells grow too quickly. This leads to thick, well-defined plaques that can be silvery and scaly.
Psoriasis often starts between ages 15 and 35 and commonly affects the scalp, elbows, knees, or lower back. Both conditions involve the immune system, but their underlying skin cell behaviour differs.
- Eczema: dry, itchy patches; common in folds like behind knees and elbows.
- Psoriasis: rapid skin cell buildup; firm plaques on scalp and extensor areas.
- Shared traits: red patches, stress as a trigger, need for tailored care.
| Feature | Typical Location | Appearance |
|---|---|---|
| Atopic dermatitis | Inner elbows, behind knees | Red, dry, inflamed |
| Psoriatic plaques | Scalp, elbows, knees, lower back | Thick, silvery scales |
| Common trigger | Whole body | Stress, moisture loss, immune shifts |
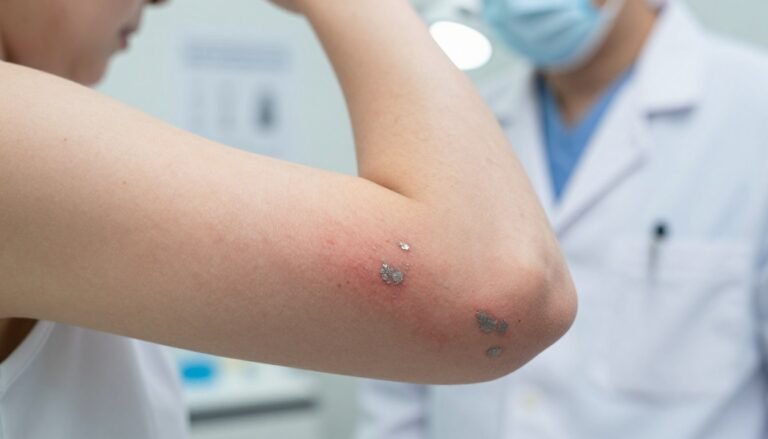
Recognizing When to See a Dermatologist for Eczema or Psoriasis
Persistent red patches or sudden bouts of swelling can mean your skin needs professional attention.
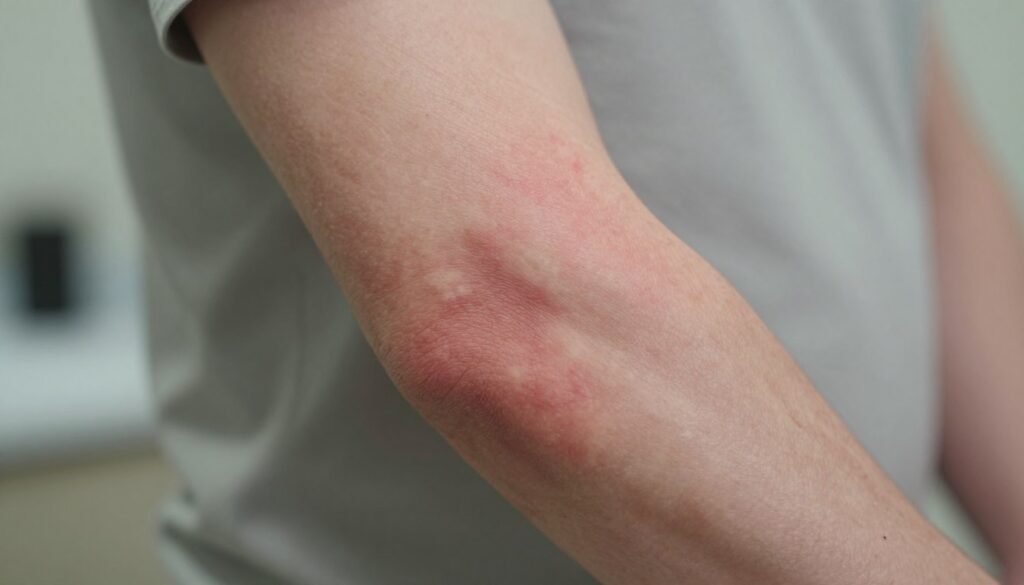
If your skin condition causes intense redness, swelling, or sleepless nights despite counter creams, reach out for an evaluation. Severe itching that interrupts sleep harms recovery and quality of life.
- Cracking, oozing, or signs of infection in patches require prompt medical care.
- Chronic atopic dermatitis or long-standing plaques often need prescription medication beyond over-the-counter treatment.
- Lesions on sensitive areas like the scalp, elbows, or knees that do not improve should be assessed by a doctor.
- Family history of skin conditions raises the chance a simple rash is a chronic issue rather than routine dryness.
Professional assessment clarifies the difference between simple dryness and an immune-driven skin condition. Targeted treatments can reduce inflammation and protect your body from complications.
| Sign | Why it matters | Next step |
|---|---|---|
| Cracking or oozing | Risk of infection | Seek prescription care |
| Sleep disruption | Poor healing and fatigue | Schedule an appointment |
| Resistant plaques | May need systemic medication | Specialist evaluation |
Common Triggers and Lifestyle Factors Affecting Skin Health
Lifestyle choices often shape how active your skin inflammation becomes. Small changes in daily habits can cut down flares and improve comfort.
Managing Daily Triggers
Stress is a major trigger that worsens both eczema and psoriasis flares. Good sleep and simple stress-relief practices help your immune system and skin cells stay balanced.
Avoid harsh soaps and synthetic fragrances. Keep moisture levels steady with bland emollients. These steps protect skin cells and reduce redness and cracking.
- Track patterns: note weather, foods, or medications that cause patches on the scalp, elbows, or knees.
- Maintain routine: gentle cleansers, regular moisturising, and timely rest aid long-term control.
- Discuss persistent symptoms and over-the-counter limits with your care team if issues persist.
| Trigger | Effect on Skin | Practical Action |
|---|---|---|
| Stress and poor sleep | Increased inflammation, flare risk | Sleep hygiene, relaxation exercises |
| Harsh soaps or dry air | Moisture loss, redness, cracking | Use mild cleansers, humidify rooms |
| Medications or cold weather | Sudden patches or worsened plaques | Monitor triggers, adjust routines with a clinician |
Advanced Treatment Options at Boss Multispeciality Hospital
Complex skin issues often need more than creams; targeted, hospital-grade treatment can make a clear difference. At Boss Multispeciality Hospital in Bangalore we offer structured plans for stubborn patches and long-standing inflammation.

Personalized Care with Dr. Varsha D.V.
Dr. Varsha D.V (MBBS, DDVL, Consultant Dermatologist & Dermatosurgeon) leads personalised programmes for patients with eczema and psoriasis. We assess your history, examine skin cells and tailor prescription plans that match your needs.
Modern Therapeutic Approaches
Our clinic provides prescription creams and advanced medications beyond over-the-counter options. Treatments include topical agents, systemic medication when needed, and targeted therapies that calm the immune system.
- Focused care for scalp and body plaques, including difficult cases.
- Evidence-based plans aimed at long-term control and comfort.
- Support for medication management and follow-up in Bangalore.
| Treatment | Use | Next step |
|---|---|---|
| Topical creams | Reduce redness and dry patches | Prescription and routine review |
| Systemic medications | Control widespread inflammation | Specialist monitoring |
| Targeted biologics | Modulate immune response | Eligibility assessment |
Why Professional Diagnosis Matters for Chronic Skin Conditions
A formal diagnosis separates simple dry skin from immune-driven conditions that need targeted therapy. Accurate identification affects long-term treatment and reduces trial-and-error with creams and over-the-counter options.
We can uncover underlying factors such as stress or harsh soaps that make a skin condition worse over time. A doctor can review your history, test if needed, and explain how the immune system is involved.
Mislabeling atopic dermatitis as routine dryness often delays proper medication and prolongs inflammation. Chronic inflammation in the body may point toward systemic disease and needs careful evaluation by a specialist.
- Targets correct medications and avoids ineffective remedies.
- Identifies triggers and builds a root-cause plan.
- Monitors for wider disease that affects the whole body.
| Issue | Likely result | Benefit of professional care |
|---|---|---|
| Misdiagnosis | Poor response to treatment | Timely correction and proper medication |
| Unchecked triggers | Repeated flares | Trigger management and lifestyle advice |
| Systemic signs | Hidden disease risk | Comprehensive assessment and follow-up |
Conclusion
An organised approach brings predictability and better outcomes for persistent skin issues.
– Managing chronic skin conditions like eczema and psoriasis needs steady attention and healthy lifestyle choices.
– Recognising early symptoms and seeking professional care can limit long-term discomfort and help you keep clear, healthy skin.
– We encourage you to prioritise skin health by working with a specialist who understands these complex conditions and your daily routine.
– Taking proactive steps now often leads to better results and a higher quality of life for you and your family.
Consult Dr. Varsha at Boss Multispeciality Hospital, Bangalore — Call +91 9986607601 to Book an Appointment.