What Is Melasma? Causes, Symptoms & Who Gets It

Curious why dark, mask-like patches appear on the face and linger despite home care?
We see this common skin condition often at Boss Multispeciality Hospital, Bangalore. Under the care of Dr. Varsha D.V (MBBS, DDVL), patients gain clear, evidence-based guidance that feels personal and practical.
Melasma can follow hormonal shifts, sun exposure, or certain medications. Pregnant women often notice changes first, but anyone can develop these pigment patches.
Our team explains causes, reviews symptoms, and offers tailored plans that protect your skin while treating the spots. We keep language simple and options realistic, so you understand each step.
If you want calm, expert answers and a plan that fits your life, we invite you to read on and learn how we support patients here in Bangalore.
Understanding What Is Melasma
Many people notice dark, blotchy patches on the cheeks and forehead during hormonal changes. This common skin condition occurs when skin cells produce extra melanin, the pigment that gives skin its natural color.
- Melasma often appears during pregnancy, earning the nickname mask pregnancy in clinical use.
- Hormones can trigger this hyperpigmentation, especially in women during reproductive years.
- Though medically harmless, the appearance can affect confidence and daily life.
- Early evaluation at Boss Multispeciality Hospital, Bangalore, helps tailor safe care under Dr. Varsha D.V.
| Feature | Typical Cause | Initial Step |
|---|---|---|
| Pattern | Hormonal shifts, sun exposure | Consult dermatologist |
| Pigment | Excess melanin production | Sun protection |
| Who | Many women during pregnancy | Personalised management plan |
We recommend professional assessment to confirm diagnosis and guide safe treatment options tailored to your skin and lifestyle.
Common Symptoms and Visual Indicators
Some people notice matching patches on both sides of the face that slowly deepen over months.
These patches most often show on the forehead, cheeks, nose, and upper lip. They may appear as dark brown or light brown areas that mirror each other.
Symmetrical Pigmentation Patterns
We often see symmetrical patterns. The cheeks and upper lip commonly show the changes first.
- Symmetry across both sides of the face.
- Spots may also appear on the neck or near the nose.
- Women may notice more during pregnancy or with hormone shifts.
Gradual Onset of Dark Patches
Color builds slowly; many patients report a subtle change that worsens in summer with sun exposure.
At Boss Multispeciality Hospital, Bangalore, we use diagnostic tools to tell this skin condition apart from other hyperpigmentation. A dermatologist exam guides tailored treatment options so you get care matched to your type of pigmentation and health needs.
Primary Causes and Triggers
A blend of internal hormones and external UV exposure commonly triggers darker facial spots.
At our clinic, Dr. Varsha D.V notes that shifts in estrogen and progesterone in the body often play a central role. Many women report new patches during pregnancy or while on birth control, which shows how linked hormones and pigmentation are.
Sun exposure and UV light then amplify the issue. UV rays tell melanocytes to make more melanin, so existing hyperpigmentation can deepen quickly in bright months.

| Trigger | How it acts | Practical step |
|---|---|---|
| Hormonal change | Estrogen/progesterone increase pigment activity | Review medications; consult dermatologist |
| Sun / UV light | Stimulates melanin production and darkens spots | Daily broad-spectrum sun protection |
| Pregnancy & birth control | Hormone shifts trigger new or worse patches | Tailored care plan during pregnancy |
We educate you on environmental and internal causes so you can prevent worsening and protect skin long term.
Risk Factors and Who Is Most Affected
Some groups face higher odds for persistent facial spots; knowing this helps us offer timely care. Age, sex and hormones shape who develops darker patches on the face and neck.
The Connection to Pregnancy
At Boss Multispeciality Hospital, Bangalore, Dr. Varsha D.V notes that 15% to 50% of pregnant women develop this skin disorder during the second or third trimester. We see many cases linked to shifts in progesterone and other hormones.
Women are about 90% more likely than men to notice these changes. The condition is most common between ages 20 and 40. Clinicians often call it mask pregnancy when the face shows symmetrical brown areas.
- Hormone changes in pregnancy and after birth can trigger new spots.
- Sun exposure worsens pigment, so daily protection matters for everyone.
- When patches appear on the neck, we evaluate both skin type and triggers.
| Risk Factor | How it affects risk | Practical step |
|---|---|---|
| Pregnancy / birth | Hormonal surge (progesterone) increases pigment | Monitor changes; consult dermatologist in 2nd trimester |
| Sex and age | Women aged 20–40 show highest occurrence | Early evaluation and tailored care |
| Sun exposure | UV deepens existing patches and creates new ones | Daily broad-spectrum sunscreen and sun habits |
We personalise plans for you, especially if spots appear during pregnancy or after birth. Protecting skin from sun remains a key step to prevent worsening and support treatment success.
Diagnostic Procedures Used by Dermatologists
Special tools in the clinic let us see pigment depth that a mirror cannot reveal.
We use a Wood lamp, also called a black light, to examine your skin closely. This light makes pigment differences stand out so we can tell if the pigment sits in the top layer or deeper.
To make sure you receive the correct diagnosis, we review your medical history, including any recent birth or hormonal shifts. This helps us link changes in your body to the skin condition you notice.
- We may perform a biopsy when needed to rule out other conditions.
- We assess the depth and spread of patches on your face and body to plan the best control measures.
- Our dermatologist pairs test findings with safe treatment choices and product guidance for your skin type.
| Procedure | Purpose | Outcome |
|---|---|---|
| Wood lamp / black light | Locate pigment layer | Guides topical vs procedural care |
| Biopsy | Exclude other skin conditions | Confirms diagnosis |
| Medical history review | Identify triggers (birth, hormones) | Personalised plan |
With clear diagnostics, we tailor treatment so you get targeted care that protects long-term skin health.
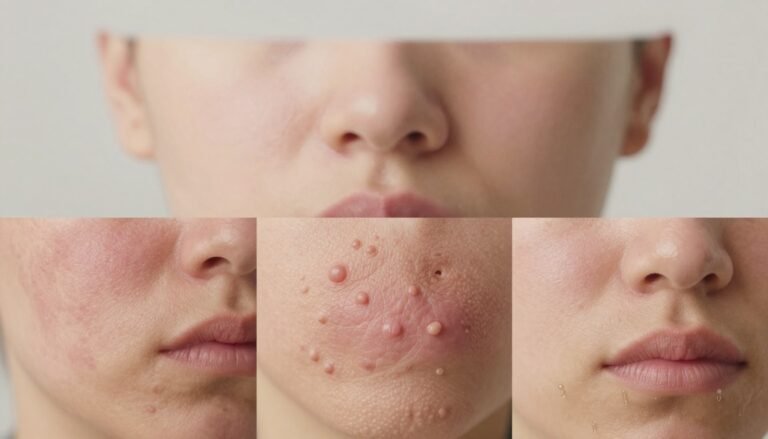
Categorizing the Types of Melasma
Identifying how deep pigment sits helps us select the right therapy for your skin.
Epidermal
Epidermal melasma affects the top layer of skin and usually shows as dark brown patches.
It often responds well to topical acid treatments and careful sun control.
We use a wood lamp to confirm pigment on the surface and plan simple therapy.
Dermal
Dermal melasma lies deeper and can appear bluish-gray.
This type needs different approaches because topical agents reach the surface less effectively.
A dermatologist may discuss combination therapies and longer timelines for control.
Mixed
Mixed melasma is the most common type and combines surface and deeper features.
We often pair chemical peels with other procedures to treat both layers.
Using a black light or wood lamp helps us map spots on the face and neck before treatment.
| Type | Appearance | Usual approach |
|---|---|---|
| Epidermal | Dark brown, surface | Topicals, sun care |
| Dermal | Bluish-gray, deep | Procedural therapy, longer control |
| Mixed | Light brown to dark brown blend | Combined treatments, tailored plan |
Effective Topical Treatment Options
Safe, doctor‑recommended topicals play a key role in controlling pigment caused by hormones and sun.
At Boss Multispeciality Hospital, Bangalore, we often prescribe azelaic acid for pregnant women because it is proven safe and gentle on skin.
Topical acids and other creams work by slowing melanin production. That helps fade brown patches and reduce contrast with surrounding skin.
- Azelaic acid — safe in pregnancy, reduces pigment and inflammation.
- Hydroquinone — commonly used at night under dermatologist supervision for short courses.
- Other acid blends — chosen by skin type and depth of pigment.
We select the right type of therapy for you and monitor progress closely. Our team explains how to apply products and how sun exposure affects results.
| Topical | Benefit | Notes |
|---|---|---|
| Azelaic acid | Reduces pigment | Safe in pregnancy; good for hormonal spots |
| Hydroquinone | Strong lightening | Use at night; under dermatologist care |
| Acid blends | Exfoliate and fade | Choose per skin type and pigment depth |
Advanced Clinical Procedures for Skin Restoration
When topical routines stall, targeted in-clinic therapies help renew skin tone. At Boss Multispeciality Hospital, Bangalore, we offer advanced options to tackle deeper pigment that creams cannot reach.
Laser Therapy and Microneedling
Our dermatologist, Dr. Varsha D.V, uses light-based therapy and microneedling to treat stubborn hyperpigmentation and persistent spots. These procedures stimulate controlled skin repair and reduce deep-seated patches.
Chemical peels and fractional lasers remove damaged layers while promoting new, healthy skin. Microneedling helps topical acid and serums penetrate more effectively after the procedure.
- Laser therapy targets pigment with focused light to fade dark areas safely over sessions.
- Microneedling creates microchannels that boost repair and improve texture.
- Chemical peels strip damaged layers and speed visible improvement when chosen carefully.
| Procedure | Main effect | Downtime | Best for |
|---|---|---|---|
| Fractional laser | Light targets pigment and stimulates collagen | Moderate (days) | Deep patches and uneven tone |
| Microneedling | Boosts healing and product absorption | Minimal (24–48 hrs) | Texture, mild hyperpigmentation |
| Chemical peels | Removes damaged top layers | Short (hours to days) | Surface pigment and mild spots |
We choose a blend of treatments and aftercare that protects long-term skin health. Please discuss these options with our team so we can design a safe, personalised therapy plan for your condition.
Lifestyle Adjustments and Sun Protection
Small daily choices help protect your skin and support clinical care. We recommend practical steps you can follow in Bangalore’s climate.

Make sure you use broad-spectrum SPF 50+ every morning, even on cloudy days. Reapply sunscreen after sweating or swimming to keep protection steady.
Avoid direct sun between 10 AM and 4 PM when UV light is strongest. Wear wide-brimmed hats and clothing that covers exposed areas to limit new spots and slow darkening of existing patches.
- We advise gentle skin care products that soothe and hydrate, not irritate, especially after chemical peels or other treatments.
- Use physical barriers (hats, umbrellas) alongside sunscreen for better control of hyperpigmentation.
- At Boss Multispeciality Hospital, Bangalore, Dr. Varsha D.V helps you choose products and routines that support long-term results.
| Measure | Why it helps | Quick tip |
|---|---|---|
| SPF 50+ daily | Blocks broad UV that deepens pigment | Apply 15 minutes before going out |
| Peak hour avoidance | Reduces strongest UV exposure | Plan outdoor tasks early or late |
| Protective wear | Physical shield for treated skin | Choose breathable fabric and wide brims |
Protecting your skin from the sun is the single most effective way to manage this condition and maintain results from treatments. We guide you on products and habits so your care plan fits daily life and delivers steady control.
Managing the Emotional Impact of Skin Conditions
When facial spots persist, many people feel less comfortable in social or work settings. We recognise how a visible skin condition can change daily confidence and mood.
Psychodermatology helps patients cope with the stress of long-term pigment issues. At Boss Multispeciality Hospital, Bangalore, Dr. Varsha D.V supports both medical care and emotional wellbeing.
We discuss practical steps to protect your mental health while treating the disorder. Managing stress, seeking counselling, or joining support groups often eases anxiety.
- We offer a caring environment that addresses the psychological side of this condition.
- Gentle products prevent irritation that can worsen both skin and mood.
- Simple light routines and realistic expectations help you track steady progress.
| Focus | How we help | Quick tip |
|---|---|---|
| Mental support | Psychodermatology referrals and counselling | Talk to a specialist early |
| Skin care | Recommend gentle, pregnancy-safe products | Patch test new items |
| Overall health | Stress management and lifestyle advice | Prioritise sleep and small daily routines |
Conclusion
Living with persistent dark patches can feel draining, but practical care brings steady improvement. This skin condition often involves excess melanin and gives dark brown or brownish spots that respond best to early control and consistent treatment.
We know many cases affect pregnant women and other women during hormone shifts. With diagnostic tools like a black light and tailored therapy — from topical acid products to chemical peels and light-based treatments — a dermatologist can guide safe treatment options and long-term control.
Make sure you prioritise sun protection and steady routines. If these spots affect your confidence, consult Dr. Varsha D.V at Boss Multispeciality Hospital, Bangalore — Call +91 9986607601 to Book an Appointment.