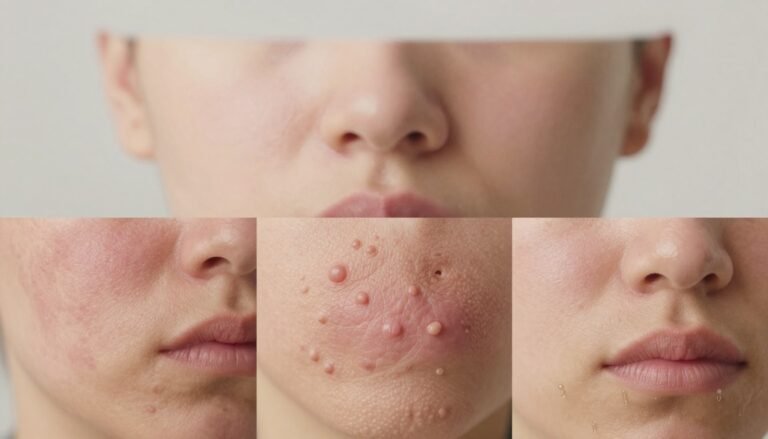
Eczema vs Psoriasis: How to Tell the Difference (With Symptom Checklist)
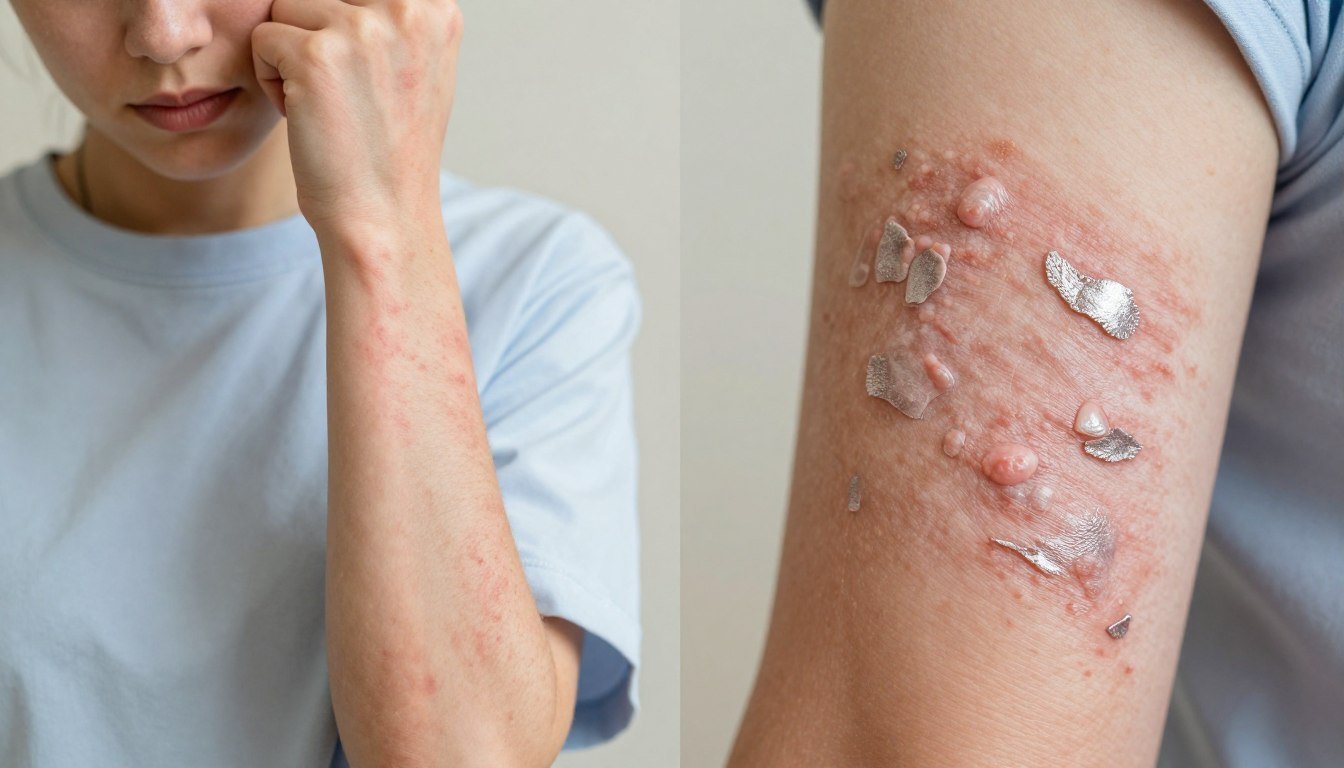
Have you ever wondered why one red, itchy patch won’t respond to the same creams as another?
We know it can be confusing. Both conditions can make skin feel raw and uncomfortable, but they are not the same. Eczema affects about four times more people worldwide than psoriasis, so the odds may surprise you.
In this short guide we explain key differences in plain language. You’ll get a simple symptom checklist to spot common signs like dry patches, thick scaly areas, and the kind of itching you feel.
Accurate diagnosis matters because treatments and medications differ — what helps atopic dermatitis may not work for plaque disease. We want to help you identify likely triggers and prepare for a focused discussion with your dermatologist or pediatrician if children are affected.
Understanding the Basics of Eczema vs Psoriasis
Not all itchy red skin comes from the same underlying process. We’ll explain how the immune system and heredity shape each condition so you can spot key differences and talk with your doctor more confidently.
The Role of the Immune System
Both conditions involve the immune system and cause visible inflammation. In one, immune signals speed up skin-cell turnover, leading to thick, scaly patches.
In the other, immune pathways make skin more sensitive and prone to dryness and intense itching. Neither is always a classic autoimmune disease, yet immune activity drives symptoms and flare-ups.
Genetic Factors
Atopic dermatitis is the most common type of eczema and often runs in families. Children with a family history of allergic conditions are more likely to develop this dermatitis.
Genetic risk also exists for psoriasis, though the inheritance patterns differ. Stress, environment, and infections act as triggers for people of any age.
- Both are chronic and affect children and adults.
- Identifying the type helps guide treatment choices.
| Feature | Immune Role | Typical Onset |
|---|---|---|
| Atopic dermatitis | Immune-driven sensitivity and inflammation | Often begins in childhood |
| Psoriasis | Immune-mediated rapid skin-cell growth | Can start at any age, common in adults |
| Common traits | Chronic inflammation, stress triggers | Affects people across ages |
Key Clinical Differences in Skin Appearance
Examining the shape, texture, and location of a rash gives clear clues about its cause. We look for how thick a patch is, whether the edge is sharp, and if scales are present.
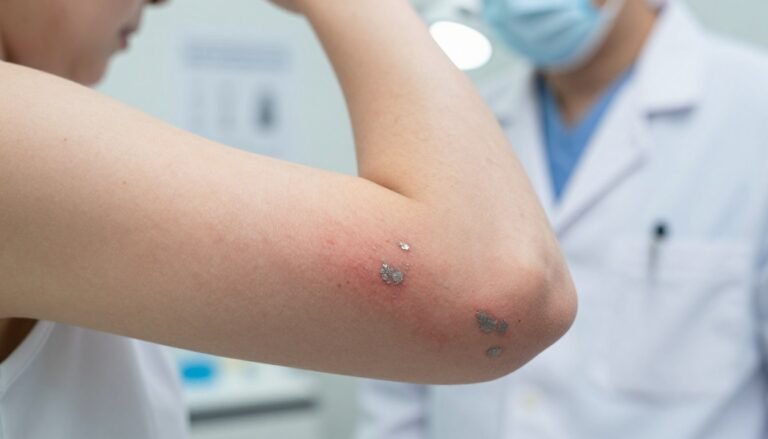
Psoriasis often forms raised, well-defined plaques with silvery scales. These patches result from rapid skin cells building up. Many people notice them on the elbows, knees, and scalp. About 8 million American adults have this condition.
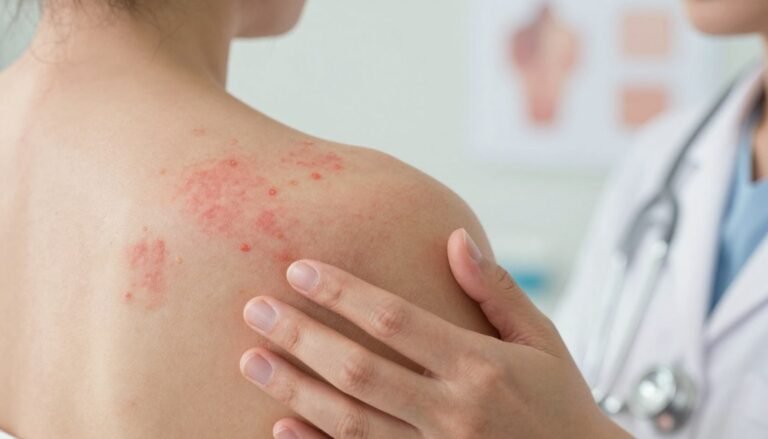
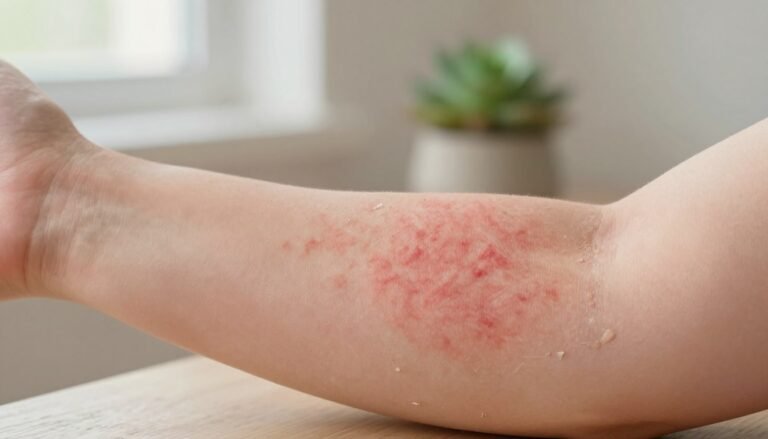
In contrast, eczema usually appears as red, inflamed, itchy skin that favors body folds. It can ooze or crust when the skin barrier breaks. Children commonly get dry rashes behind the knees and in elbow creases.
- Psoriasis: thick plaques, silvery scales, well-defined edges.
- Eczema: less distinct patches, intense itching, more common in folds and on hands or face.
- Location and texture help dermatologists decide the next steps for testing and treatment.
| Feature | Psoriasis | Eczema / Atopic dermatitis |
|---|---|---|
| Typical texture | Thick, scaly | Dry, inflamed |
| Common areas | Elbows, knees, scalp | Body folds, face, hands |
| Edges | Well-defined plaques | Less distinct patches |
Identifying Common Triggers for Flare-ups
Small changes in your day-to-day life often spark a sudden skin flare-up. Knowing common causes helps you act early and reduce discomfort.
Environmental Irritants
Harsh soaps, detergents, and fragranced products are frequent irritants that worsen eczema symptoms. Cold weather and dry indoor air strip moisture and can spark inflammation.
Protect your hands and avoid abrupt product switches to limit reactions on sensitive areas like the elbows and knees.
Stress and Lifestyle Factors
Stress affects the immune system and can trigger flares in both psoriasis and eczema. Poor sleep, smoking, and heavy alcohol use also raise the chance of symptom recurrence.
Keeping a simple diary of stress, diet, and sleep often reveals patterns you can change to prevent future episodes.
Medication Triggers
Certain medications, including some blood-pressure drugs, have been linked to worsening plaques in psoriasis. Always tell your dermatologist about new prescriptions or supplements.
Avoiding triggers is a key part of long-term management and helps make any medical treatment more effective.
- Avoid harsh irritants and opt for gentle, fragrance-free products.
- Track stress and daily exposures in a journal to spot causes fast.
- Protect skin from injury and sunburn to prevent new patches.
| Trigger type | Typical effect | Practical step |
|---|---|---|
| Environmental irritants | Dryness, itching, flare-ups | Use mild cleansers and moisturize |
| Stress and lifestyle | Immune-driven flares | Improve sleep, manage stress |
| Medications | May worsen plaques or redness | Review meds with your doctor |
Age of Onset and Long-term Health Risks
The age when symptoms first appear gives useful diagnostic clues. Psoriasis most commonly starts in early adulthood, often between 15 and 35, and tends to be lifelong.
Childhood skin inflammation often begins in infancy. Many children improve as their skin barrier matures, though some people carry symptoms into adult years.
Long-term risks differ between these conditions. Psoriasis can raise the chance of cardiovascular disease, metabolic syndrome, and psoriatic arthritis in some patients.
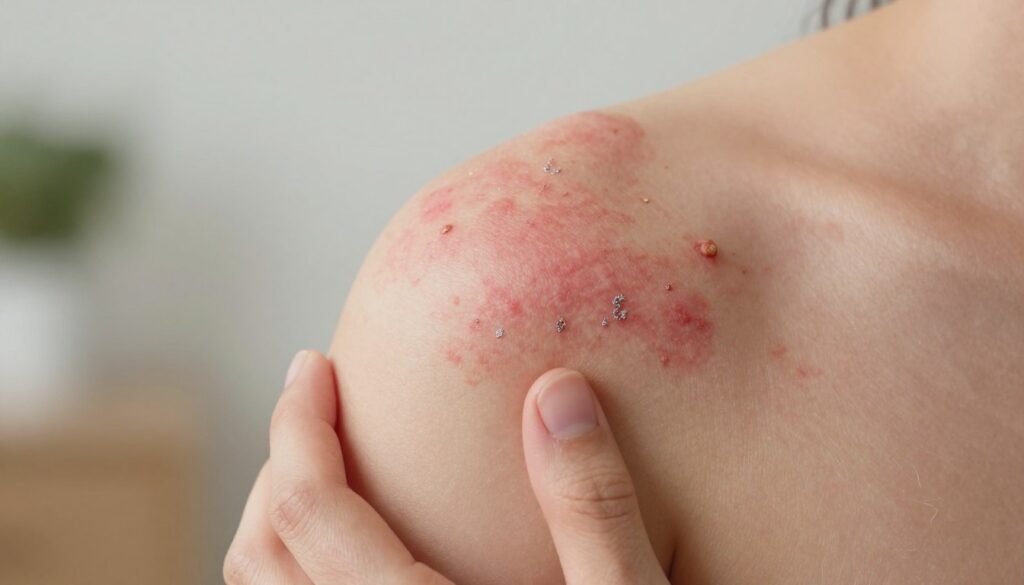
- Both conditions may cause thick, leathery patches if not managed well.
- Psoriasis plaques often appear on the elbows, knees, scalp, or hands as scaly patches.
- Childhood dermatitis commonly affects folds and areas prone to itching.
| Onset | Long-term risks | Common areas |
|---|---|---|
| Early adulthood (15–35) | Cardiovascular disease, metabolic issues, arthritis | Elbows, knees, scalp, hands |
| Infancy or childhood | Allergic conditions; may improve with age | Skin folds, face, hands |
Early intervention helps protect overall health and comfort. We recommend discussing persistent patches or new symptoms with a dermatologist to plan long-term care.
Diagnostic Approaches for Skin Conditions
A firm answer about a stubborn skin patch usually requires medical examination and sometimes lab work. We recommend seeing a dermatologist when patches persist, spread, or do not respond to basic care.
The Importance of Professional Diagnosis
A professional diagnosis from a dermatologist is the only way to accurately distinguish between eczema and psoriasis for your specific case. Treatment protocols differ, and using the wrong approach can delay relief.
At your visit, the doctor will examine affected areas and ask about family history of the immune system or dermatitis. They may review your medications and recent exposures to find likely causes of inflammation.
- Clinical evaluation clarifies symptoms and guides therapy.
- When appearance is unclear, a small biopsy or lab analysis may confirm the diagnosis.
- Understanding root causes helps us tailor long-term treatment and avoid trial-and-error.
| Procedure | Purpose | What to expect |
|---|---|---|
| Physical exam | Visual assessment of lesions | Quick, in-office review and discussion |
| Skin biopsy | Confirm diagnosis when unclear | Minor outpatient procedure with local numbing |
| Medication review | Identify drugs that may worsen skin | Adjust prescriptions under medical guidance |
If you have concerns about your rash, seeking timely diagnosis starts you on the path to clearer, healthier skin. We are here to help you navigate tests, results, and effective treatment options.
Effective Management and Treatment Strategies
Good skin control blends targeted treatments with simple daily steps you can keep up.
Topical corticosteroids reduce inflammation quickly. Emollients protect the barrier and cut itching by keeping skin hydrated.
For moderate to severe cases, doctors may offer systemic medications or light therapy (phototherapy) to slow skin cells and calm an overactive immune system.
- Use fragrance-free moisturizers and avoid known irritants to reduce flare-ups.
- Follow prescribed topical treatments like corticosteroids or calcineurin inhibitors for short, safe courses.
- Consider phototherapy for widespread or stubborn patches on the scalp and body under specialist supervision.
- Manage stress through sleep, meditation, or gentle exercise to lower trigger risk.
| Approach | When to use | Expected benefit |
|---|---|---|
| Topical corticosteroids | Mild to moderate flares | Reduces inflammation and itching |
| Emollients / barrier care | Daily maintenance | Improves hydration and prevents irritation |
| Phototherapy (light therapy) | Moderate to severe or widespread disease | Slows excess skin cell growth and eases scales |
| Systemic medications | Severe or treatment-resistant cases | Controls immune-driven inflammation systemically |
Expert Care at Boss Multispeciality Hospital
Getting specialised care helps turn uncertainty about a rash into a clear plan. At Boss Multispeciality Hospital in Bangalore we deliver focused dermatology services for persistent skin problems.
Our team is led by Dr. Varsha D.V (MBBS, DDVL), Consultant Dermatologist & Dermatosurgeon. She manages complex psoriasis and eczema cases, using proven protocols and modern medications.
We combine clinical exam, targeted tests, and personalised treatment plans. You can expect clear explanations, stepwise therapy, and follow-up to track progress.
- Evidence-based medications and up-to-date treatment options.
- Compassionate consultations where your questions matter.
- Tailored plans for adults and children with chronic skin conditions.
If you are struggling with persistent skin issues, consult Dr. Varsha at Boss Multispeciality Hospital, Bangalore — Call +91 9986607601 to Book an Appointment.
| Service | Lead clinician | Contact |
|---|---|---|
| Dermatology consultations | Dr. Varsha D.V (MBBS, DDVL) | +91 9986607601 |
| Medications & topical care | MD-led prescriptions | In-clinic review |
| Procedures & dermatosurgery | Consultant dermatosurgeon | Appointment required |
Conclusion
.
Clear steps help you move from confusion to a confident plan for managing persistent skin patches. A quick checklist and awareness of psoriasis eczema signs can guide when to seek care.
Both eczema and psoriasis need a reliable diagnosis and a tailored treatment plan. We recommend discussing your history, current creams, and any family pattern so your clinician can recommend the right approach.
Identify your triggers, keep a simple routine, and ask about options such as light therapy or medication when needed. Early action on symptoms and triggers often cuts flare-ups and eases daily discomfort.
You do not have to manage these skin conditions alone. Call for a consultation to get a clear diagnosis and a personalized plan that helps protect your skin and comfort.