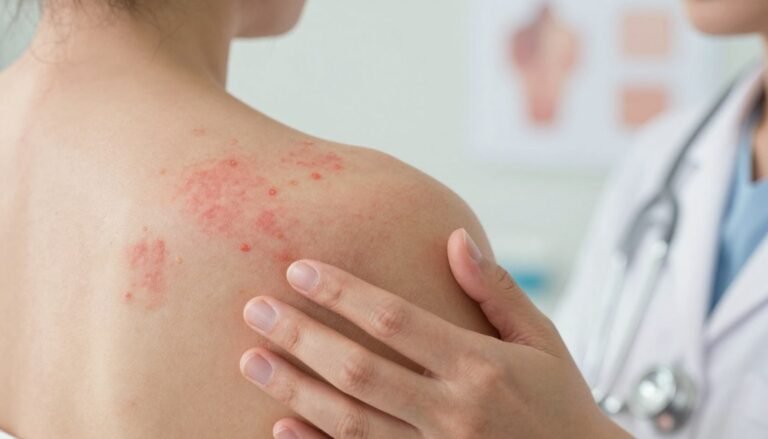
What Is Psoriasis? Causes, Types & Symptoms Explained
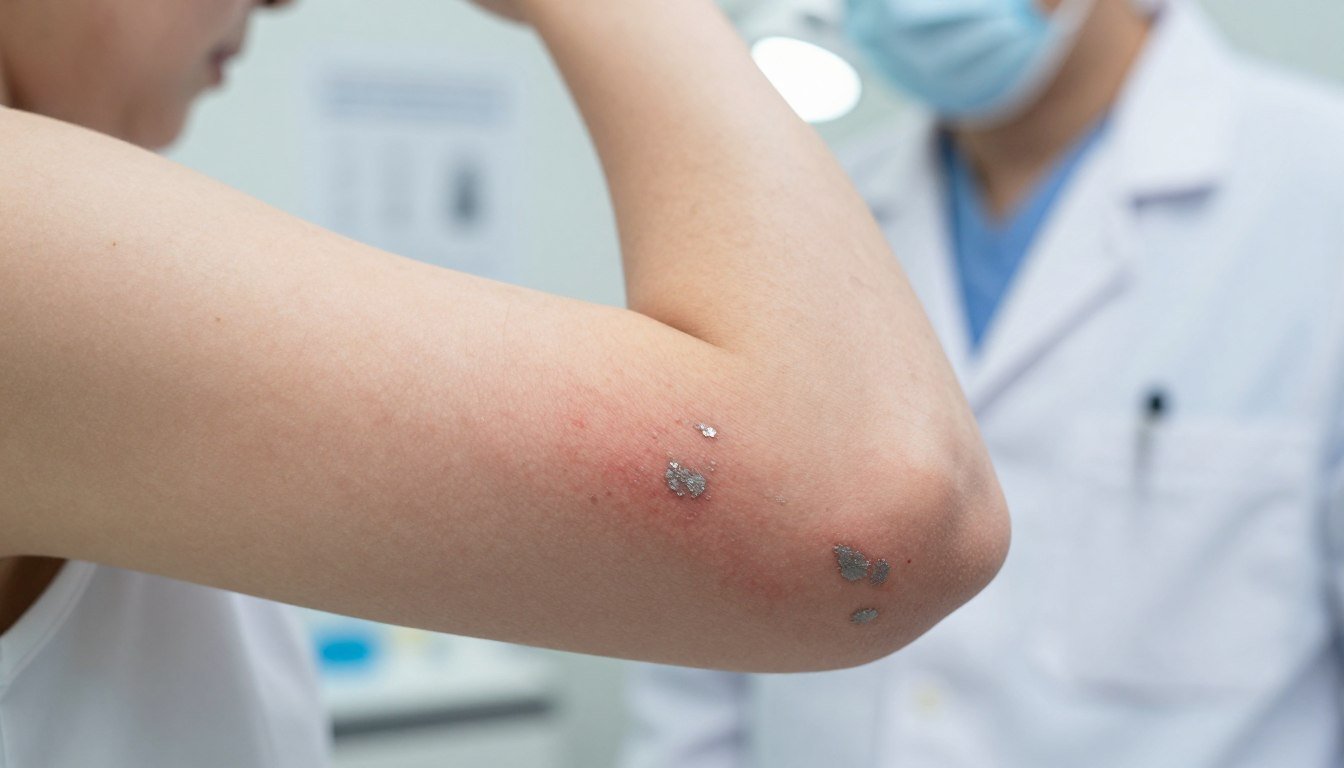
Can a single change in the immune system turn healthy skin into a persistent challenge that shapes daily life?
We know this condition affects millions of people and can feel overwhelming at first. Understanding what is psoriasis is the first step toward clearer skin and better well-being.
Psoriasis is a chronic disease where the immune system speeds up skin cell growth. That rapid turnover leads to patches, irritation, and varied symptoms that differ by types and by person.
Early diagnosis helps guide treatment and lifestyle choices. We urge you to seek professional care so a trained clinician can confirm diagnosis and tailor treatments to your needs.
Our aim is to give you clear, practical information so you can make informed decisions and find relief through modern care options.
Understanding What Is Psoriasis
Immune-driven overproduction of skin cells leads to patches that can itch, thicken, or flake.
This chronic disease most often shows as inflamed, scaly areas on the scalp, elbows, or knees. The pattern helps clinicians spot the condition early and guide care.
Many people notice cycles: active flare-ups alternate with clearer periods. Knowing this helps reduce fear and set realistic expectations for treatment.
Effective plans target your specific skin needs. We work with you to tailor treatment, manage symptoms, and improve daily comfort.
- Common sites: scalp, elbows, knees.
- Typical signs: red patches, scaling, occasional pain or itching.
- Care approach: personalised plans from dermatology teams.
| Site | Common Sign | Flare Pattern |
|---|---|---|
| Scalp | Thick scales | Intermittent |
| Elbows | Raised plaques | Photosensitive |
| Knees | Dry, red patches | Stress-linked |
The Role of the Immune System in Skin Health
An overactive immune response can speed skin renewal and reshape how your skin looks and feels. We want you to understand this process so you can follow treatment with confidence.
The Mechanism of Rapid Cell Growth
The immune system sometimes mistakes healthy tissue for a threat. It releases signals that drive cells to divide fast. These skin cells reach the surface in days rather than weeks.
This rapid turnover causes visible inflammation and thick, scaly patches. For people affected by psoriasis, daily care often focuses on calming that immune activity.
- Overactive immune signals trigger faster cell production in the body.
- These signals also fuel inflammation that leads to redness and scaling.
- Targeted therapies aim to slow cell turnover and reduce symptoms.
| Process | Effect on Skin | Clinical Impact |
|---|---|---|
| Immune activation | Increased cell division | Thick plaques; itching |
| Inflammatory signals | Redness and scaling | Visible flares; discomfort |
| Rapid skin renewal | Poor barrier function | Higher infection risk; treatment need |
Common Types of Psoriasis
Several distinct forms affect the skin differently, each requiring tailored care and attention.
Plaque Psoriasis
Plaque is the most common form. It shows as raised, red patches topped with silvery scales.
These plaques often form on the knees and elbows. They can itch and may thicken over time.
Guttate Psoriasis
Guttate often appears in children and young adults as many small red dots.
It commonly follows an upper respiratory infection or strep throat. Early treatment reduces spread.
Erythrodermic Psoriasis
Erythrodermic is rare but severe. Large areas of red, scaly skin can cover most of the body.
This form needs urgent medical care because it can affect temperature control and fluid balance.
- Inverse psoriasis appears in skin folds and worsens with rubbing or sweat.
- Triggers such as stress or certain medications can raise severity of symptoms.
- Identifying the type helps us choose targeted treatments that calm skin cells and reduce plaque buildup.
Recognizing the Symptoms
Many people first notice changes in texture or small patches on the scalp or knees.
Common signs include thick, red areas topped with silvery scales that may itch or bleed. Dry, cracked skin can sting during flare-ups.
You may see nail changes like pitting or thickening. Joint stiffness, swelling, or pain can point to psoriatic arthritis and needs prompt evaluation.
- Skin patches that grow into raised plaque or shed flaky scales.
- Severe flares that affect large areas of the body, including rare erythrodermic psoriasis.
- Small, drop-like spots in guttate patterns after infections for some people.
Tracking symptom changes helps us tailor care and assess severity. Note new pain, spreading plaques, or nail damage and tell your clinician.
| Sign | Common Site | When to Seek Help |
|---|---|---|
| Thick red plaques | Elbows, knees, scalp | Rapid spread or bleeding |
| Joint pain/stiffness | Fingers, knees, ankles | Morning stiffness or swelling |
| Nail changes | Fingernails, toenails | Pitting, lifting, or thickening |
Potential Triggers and Risk Factors
External influences and inherited traits often combine to trigger flare-ups in sensitive skin.
We know infections, smoking, and some medications can raise the risk of flares. Streptococcal throat infections often spark a sudden, guttate pattern, especially in children.
Environmental Factors
Stress, heavy smoking, and certain drugs may upset the immune system and prompt visible symptoms.
Identifying these environmental triggers helps you avoid avoidable flares and supports long-term control.
Genetic Predisposition
Many people with the disease have a family history. Genes influence how immune cells react and how skin renews itself.
Knowing family history lets us screen earlier and personalise care for better outcomes.
- Infections (strep) can trigger sudden outbreaks, particularly in younger patients.
- Medications for heart or mental health occasionally worsen skin inflammation.
- Lifestyle factors like stress and smoking increase flare frequency and severity.
| Trigger | How it Affects Skin | What We Do |
|---|---|---|
| Streptococcal infection | Can prompt rapid, droplet-like lesions | Treat infection; monitor for spread |
| Smoking & stress | Raise inflammation; worsen plaques | Offer cessation support; stress management |
| Certain medications | May alter immune response and flare risk | Review drugs with your clinician; consider alternatives |
| Family history | Higher lifelong susceptibility | Early evaluation and personalised plan |
Associated Health Conditions and Comorbidities
Many people living with this chronic condition face health issues that extend beyond the skin.
We monitor for linked conditions such as psoriatic arthritis, heart disease, obesity, diabetes, and depression. Early detection helps reduce long-term harm.

Psoriatic arthritis causes joint pain, swelling, and stiffness. It can also affect tendon attachments and lead to lasting joint damage if not treated early.
- Living with psoriasis raises the risk of other serious conditions, including inflammatory arthritis.
- Managing systemic inflammation can lower risk and improve everyday life.
- Care should look beyond visible symptoms to protect the whole body.
| Associated Condition | Typical Effect | Clinical Action |
|---|---|---|
| Psoriatic arthritis | Joint pain, swelling, tendon involvement | Early rheumatology referral; targeted treatment |
| Heart disease & diabetes | Increased cardiovascular risk; metabolic issues | Risk screening; lifestyle and medical management |
| Depression & obesity | Lower quality of life; higher inflammation | Mental health support; weight management plans |
The Diagnostic Process
A careful exam helps separate similar rashes so you get the right care quickly.
We start by reviewing your symptoms and medical history. Then we inspect the skin closely, noting plaque shape, size, and location. These clues often point toward a clear diagnosis.
The Role of Skin Biopsy
If visual exam leaves uncertainty, we may take a small skin sample. A skin biopsy removes a tiny piece so a lab can examine the cells under a microscope.
This test confirms the disease at a cellular level and helps rule out other skin conditions. With that result, we choose the most suitable treatment plan for you.
- Thorough skin exam to distinguish similar rashes.
- Biopsy when appearance alone cannot confirm diagnosis.
- Consideration of plaque location to guide care decisions.
- Review of symptoms and history to exclude other skin conditions.
- Clear diagnosis so people can begin timely treatment.
| Step | Purpose | Expected Outcome |
|---|---|---|
| Clinical exam | Identify plaque patterns and lesion sites | Probable diagnosis; plan next steps |
| Skin biopsy | Microscopic review of skin cells | Definitive diagnosis; guide therapy |
| History review | Assess triggers, symptoms, family risk | Personalised treatment recommendations |
Modern Treatment Options
Treatment choices have changed a lot in recent years, giving people more control over symptoms and daily comfort.
We offer a range of therapies for plaque psoriasis and other forms. Topical creams and medicated ointments help calm local inflammation and repair skin. Phototherapy uses targeted light to slow rapid skin cells turnover.
Systemic options include oral drugs and biologic or biosimilar medications that act on the immune system. For severe psoriasis or psoriatic arthritis, biologics can reduce inflammation across the body and protect joints.
- Topicals for mild to moderate plaques and symptom relief.
- Light therapy for widespread but non-severe disease.
- Oral and biologic systemics for moderate-to-severe cases and arthritis.
- Complementary care to support skin health and overall life quality.
| Approach | When Used | Benefits |
|---|---|---|
| Topical medications | Mild to moderate | Reduce scaling; soothe itching |
| Phototherapy (light) | Widespread skin involvement | Slows cell turnover; fewer flares |
| Systemic (oral/biologic) | Severe cases or arthritis | Lower systemic inflammation; protect joints |
Every person responds differently, so we tailor plans and monitor progress. Consistent care lowers the risk of heart disease and psoriatic arthritis and helps people enjoy better life quality.
Lifestyle Management and Prevention
Daily habits can shape how often flare-ups appear and how severe they feel.
We advise gentle care of your skin and scalp to manage scales and reduce irritation. Use mild cleansers and regular, fragrance-free moisturizers. Avoid scratching or picking at plaques to lower the chance of new lesions.
Stress and skin injury are common triggers. Stress-reduction techniques such as breathing exercises, gentle yoga, or short walks often help people stay more comfortable. Ask your clinician before adding new supplements or alternative therapies so they fit with your treatment plan.
- Keep skin hydrated and protect injured areas to prevent plaque formation.
- Review medications with your doctor to limit drugs that raise flare risk.
- Combine medical treatment and mindful lifestyle choices to improve life quality.
| Action | Benefit | When to Consult |
|---|---|---|
| Daily moisturising | Reduces scales and itching | If dryness persists |
| Stress management | Fewer flares; better sleep | If anxiety affects routine |
| Avoid skin trauma | Less new plaque formation | After cuts or procedures |
Expert Dermatological Care at Boss Multispeciality Hospital
At Boss Multispeciality Hospital we offer focused dermatology care for complex skin concerns. Our team evaluates each person with a clear plan that balances medical treatments and daily life needs.
We provide personalised diagnosis for plaque psoriasis, guttate and erythrodermic forms. We also screen for psoriatic arthritis and related risks so your whole body health is considered.
Consult Dr. Varsha at Boss Multispeciality Hospital, Bangalore — Call +91 9986607601 to Book an Appointment
Dr. Varsha D.V (MBBS, DDVL) leads our dermatology service. She offers expert, compassionate care and tailors treatments for severity, scalp involvement, and joint symptoms.
- Expert diagnosis and tailored treatment plans for all types.
- Options include topical care, light therapy, systemics and biologics when needed.
- Integrated support for joint pain from psoriatic arthritis and related conditions.
| Service | Conditions Treated | Typical Approach | Contact |
|---|---|---|---|
| Consultation & Diagnosis | Plaque psoriasis, guttate | Clinical exam, biopsy when needed | +91 9986607601 |
| Medical Treatments | Severe psoriasis, erythrodermic | Topicals, oral meds, biologics | Book with Dr. Varsha |
| Multidisciplinary Care | Scalp issues, psoriatic arthritis | Dermatology + rheumatology referrals | Boss Multispeciality Hospital |
Conclusion
A clear diagnosis and ongoing care help people regain confidence in their skin and routine. Consistent steps make daily life easier and reduce flare-ups.
This chronic disease can be managed. With personalised treatment and practical habits, you can keep skin calmer and more comfortable.
We are here to support every stage of your care. Take the first step by contacting our team at Boss Multispeciality Hospital to begin a plan tailored for you.
Call Dr. Varsha at +91 9986607601 to book an appointment and start your journey toward clearer, healthier skin and better long-term control of psoriasis.