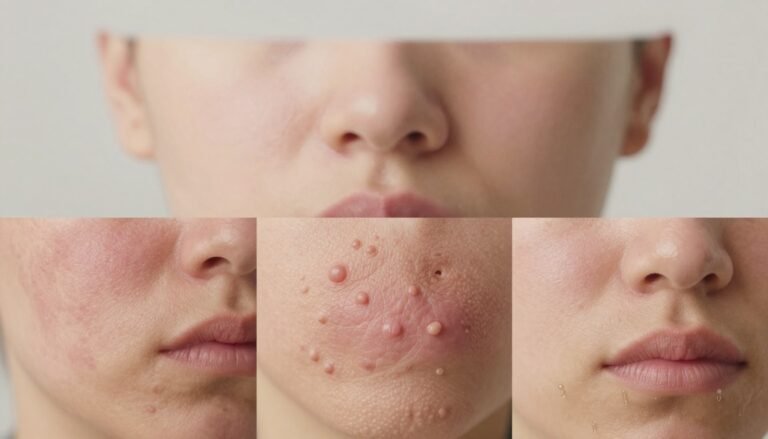
Hormonal Acne in Women: Triggers, Symptoms & Treatment

Have you ever wondered why breakouts return despite good habits and home care?
Persistent spots can feel overwhelming. We know this and we want to help you find clear, practical steps to manage your skin.
At Boss Multispeciality Hospital in Bangalore, Dr. Varsha D.V (MBBS, DDVL) offers evidence-based care. We listen, assess root causes, and design a plan that fits your health profile.
Seeking a qualified dermatologist is often the first step toward lasting improvement. Our approach balances medical treatment with gentle, personalized support so you get safe results without harsh promises.
Read on to learn common triggers, signs to watch for, and medically guided options that many patients in India find effective.
Understanding Hormonal Acne in Women
Acne can start or return well into adulthood, catching many people off guard.
Dr. Susan Massick reports that about half of females in their 20s and one in four women in their 40s experience adult acne. These numbers show that breakouts are not just a teen issue.
Shifts in hormones during different life stages can make oil glands more active. Pregnancy, for example, often brings noticeable skin flare-ups as hormone levels change.
- Many assume blemishes are only a teenage problem; adults also get persistent breakouts.
- Fluctuations in estrogen and progesterone often play a role.
- Effective care starts with recognizing that the skin reflects internal changes.
We recommend a dermatologist evaluation when breakouts recur. A clinical assessment helps distinguish surface irritation from deeper biological triggers and guides safe, evidence-based treatment.
Biological Triggers and Hormone Fluctuations
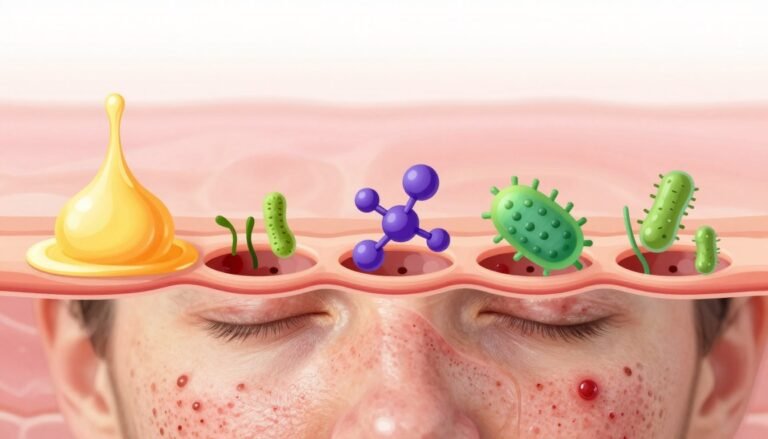
When hormone levels shift, the skin can react quickly. Small rises in certain chemicals set off a chain that increases oil and inflammation. We focus on explaining these changes so you know what to watch for.
The Role of Androgens
Androgens, such as testosterone, are not just male hormones. People assigned female at birth also produce them, and even modest rises can stimulate oil glands.
That extra oil clogs pores and can lead to persistent acne. A dermatologist can check hormone levels and suggest targeted care when needed.
Impact of Stress and Sleep
Stress triggers cortisol, which often ramps up oil production and inflames the skin.
Poor sleep worsens this cycle and reduces resilience. Managing stress and improving sleep are simple steps that support overall health and clearer skin.
- Androgens play a direct role in oil production and breakouts.
- Stress increases cortisol and can worsen skin flare-ups.
- Good sleep and lifestyle habits help reduce these triggers.
Identifying Symptoms and Affected Areas
You may find recurring, tender nodules along your jawline that resist ordinary spot care. These lesions are often deep and painful rather than surface blackheads or whiteheads.
Dr. Susan Massick notes that hormonal acne often forms on the lower face—jawline, chin and neck. These bumps feel firm and can leave marks if handled roughly.
We advise seeing a dermatologist to confirm whether your breakouts match this pattern. A clinical exam focuses on where the skin shows inflammation and how the lesions behave over time.
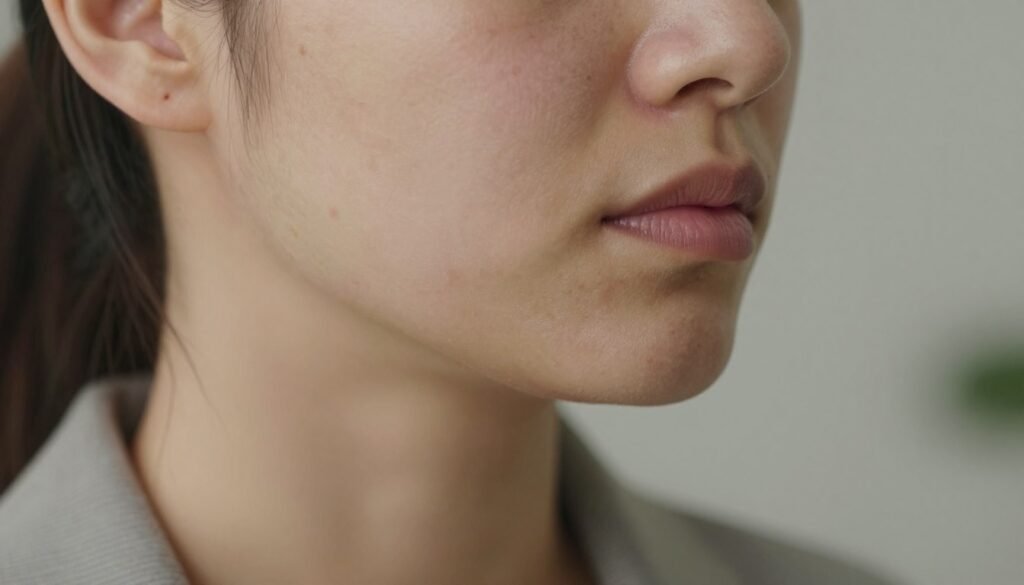
- Clusters commonly appear around the jawline, chin, and neck and cause discomfort.
- Deep, painful nodules distinguish these spots from typical teenage blemishes.
- A dermatologist can identify causes and suggest targeted care to reduce scarring.
Avoid popping these nodules. Squeezing increases the risk of permanent scarring or discolouration and can delay healing.
Distinguishing Hormonal Acne from Other Skin Conditions
Different skin conditions can look similar, yet they need very different treatments. A clear diagnosis saves time and prevents ineffective remedies.
Fungal acne versus deeper gland-driven breakouts
Fungal acne occurs when yeast enters hair follicles. It often shows as small, uniform bumps on the forehead rather than the lower face.
Men who take testosterone supplements can also develop breakouts, showing how hormone levels affect both sexes. Detecting the cause matters because treatment for fungal acne differs from that for deeper, gland-related lesions.
- Fungal acne is often itchy and forms small, even bumps; the other type is deeper and painful.
- We help people tell these conditions apart so you get the right care quickly.
- Even men may see changes linked to therapy, so hormone levels are a shared factor.
- A dermatologist will inspect hair follicles and skin texture to confirm the diagnosis.
Accurate identification prevents wasted treatments and helps adults find effective, targeted care.
Lifestyle Adjustments for Clearer Skin
Practical changes at home help reduce flare-ups and support clearer skin. We advise simple, steady habits rather than quick fixes.
Choose gentle, non-comedogenic and hypoallergenic cleansers for daily face care. Avoid essential oils that can clog pores and irritate sensitive skin.
Exercise and a balanced diet help lower stress and boost overall health. Limiting excess sugar and dairy may reduce certain breakouts for some people.
- Use gentle, non-comedogenic products to prevent further irritation.
- Manage stress with yoga or meditation to lower cortisol and calm skin.
- Adopt a healthy diet and regular activity to support long-term skin health.
- See a dermatologist for product guidance and to avoid abrasive exfoliants.
- Keep routines consistent—steady care is the foundation for managing hormonal acne.
We focus on small, sustainable steps that help you achieve clear skin over time. If flare-ups persist, a clinical review can tailor treatment to your needs.
Over-the-Counter and Topical Treatment Approaches
Smart topical options help control oil and calm inflamed skin without complex procedures.
We recommend starting with gentle, evidence-based products that target the root causes of breakouts. Topicals can reduce blocked follicles, limit bacteria, and speed cell turnover when used correctly.

Retinoids and Adapalene
Retinoids such as adapalene and tretinoin regulate oil production and boost skin cell renewal. This helps clear clogged pores and lowers the chance of new bumps forming.
We often recommend retinoids as an effective treatment for people with persistent adult acne. A dermatologist will show you how to introduce them slowly to avoid irritation.
Benzoyl Peroxide Benefits
Benzoyl peroxide reduces inflammation and kills surface bacteria that worsen breakouts. It pairs well with retinoids when timed correctly to balance effectiveness and comfort.
Using the right topical products can help you treat hormonal acne by reducing oil and calming the face. A clinician will tailor a routine so you see results without excess dryness.
- Retinoids: promote turnover and prevent clogged pores.
- Benzoyl peroxide: anti-bacterial and anti-inflammatory support.
- Professional guidance ensures safe combination use and steady progress.
| Product | Main Benefit | Best Use |
|---|---|---|
| Adapalene/Tretinoin | Regulates oil, speeds cell turnover | Night routine, gradual build-up |
| Benzoyl Peroxide | Kills surface bacteria, reduces inflammation | Spot treatment or alternating with retinoid |
| Combined Care | Balanced control of clogged pores and bacteria | Follow dermatologist plan to limit irritation |
Medical Interventions and Prescription Therapies
Medical options can target the root causes of recurring breakouts rather than only treating surface signs.
We often start with therapies that adjust hormone levels and reduce oil driven by androgens. Birth control pills with balanced estrogen and progesterone can help regulate cycles and lower flare-ups during reproductive years.
Spironolactone is another common choice. It blocks androgen effects on hair and oil glands and can reduce deep, painful bumps over months.
- We may prescribe birth control pills to help regulate hormone levels and achieve clearer skin.
- Spironolactone addresses androgen-related causes that often drive persistent breakouts.
- For severe, treatment-resistant cases, isotretinoin can offer lasting remission when monitored carefully.
- Short courses of antibiotics plus benzoyl peroxide may control inflammation while limiting resistance.
| Treatment | Main Action | Typical Use |
|---|---|---|
| Birth control pills | Stabilize hormone levels | For people with menstrual-linked breakouts |
| Spironolactone | Blocks androgen effects on oil and hair | Off-label for adults with persistent lower-face lesions |
| Isotretinoin | Reduces oil, shrinks glands, clears clogged pores | Severe, nodular disease under close supervision |
We tailor prescriptions to your health, stress factors, and goals. Working with a dermatologist helps you know how long hormonal acne will last and when to adjust therapies for safe, steady improvement.
Expert Dermatological Care at Boss Multispeciality Hospital
When breakouts persist despite careful routines, professional care can make the difference.
At Boss Multispeciality Hospital in Bangalore we offer evidence-based skin care led by Dr. Varsha D.V (MBBS, DDVL). Our clinic focuses on identifying triggers that drive adult breakouts and on building a clear, practical plan.
Consult Dr. Varsha D.V for Personalized Treatment
Dr. Varsha is a Consultant Dermatologist & Dermatosurgeon who tailors acne treatment to your needs. She evaluates hair and oil patterns, review stress and health factors, and recommends a balanced plan to treat hormonal acne when appropriate.
- We provide effective treatment plans for specific skin concerns.
- Dr. Varsha identifies unique triggers and designs gentle, long-term care.
- Trust our team to help you achieve clear skin and lasting confidence.
- To see a dermatologist, consult Dr. Varsha at Boss Multispeciality Hospital — Call +91 9986607601 to Book an Appointment.
| Service | Main Focus | Best For |
|---|---|---|
| Clinical Assessment | Identify triggers and skin type | Adult, recurring breakouts |
| Personalized Plan | Topical and systemic treatment | Targeted, effective treatment |
| Follow-up Care | Monitor progress and adjust therapy | Long-term clear skin |
Conclusion
Finding steady improvement often means combining smart home care with professional support. We aim to help you adopt gentle habits and consistent care that protect your skin and build confidence.
Understand the causes that drive breakouts. Address clogged pores and monitor hormones and levels that affect oil production. For many people, tailored treatment works best for lasting change.
Worried about how long hormonal acne last or about adult acne? We guide you through realistic timelines and options so you know what to expect.
If flare-ups persist, please see dermatologist at a trusted clinic. Together we can plan safe treatment and help you achieve clearer skin over time.