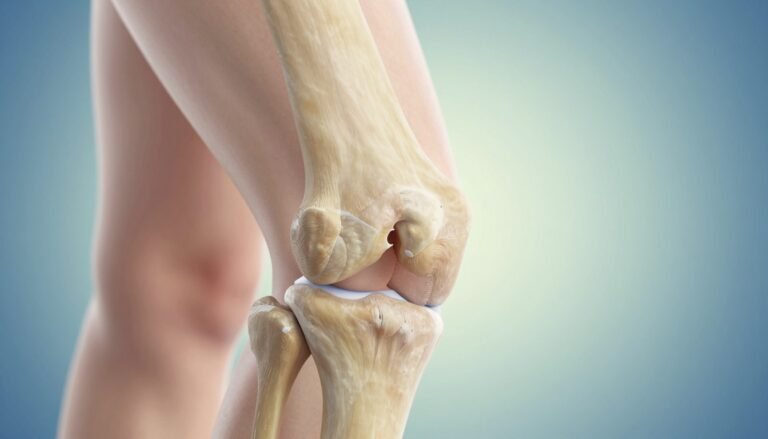
Early Signs of Knee Arthritis You Shouldn’t Ignore
Have you noticed your knee acting up after a walk or when climbing stairs and wondered if it will get worse?
I am Dr. Lokesh Chowdary R, MBBS, MS – Orthopaedics, Managing Director and Senior Orthopedic Surgeon at Boss Multispeciality Hospital on Magadi Main Road, Bangalore. I keep explanations simple and reassuring.
Small, on-and-off pain or mild swelling can be the first clue that cartilage is wearing down. That process leads to irritation and gradual inflammation, which can change how the joint feels and moves.
This guide will help you spot warning signals, understand what happens inside the joint, and learn practical next steps. My aim is timely evaluation, accurate diagnosis, and starting with non-surgical care whenever possible.
Not all knee pain equals arthritis, so do not self-diagnose. If your knee bothers you during walking, using stairs, or after rest, read on — those patterns matter and a doctor can help plan the right care.
Why catching knee arthritis early matters for your knee joint
In practice I find the first complaints are subtle—short-lived stiffness or a twinge that fades with rest. These small changes often come and go before swelling or limited motion appears.
As an orthopedic surgeon in Bangalore, I tell people that this quiet phase is the best window to slow joint wear. When symptoms are mild, we can reduce load on the knee joint and build muscle support to protect cartilage.
What I see most often in clinic when symptoms start “quietly”
- Mild pain after a long day or discomfort on stairs that improves with rest.
- Brief stiffness after sitting, then normal motion once you move.
- Repeated micro-irritation that, over months, can add damage even if the knee looks normal.
I explain that this disease often progresses at different rates for different people. If mild patterns recur weekly or begin to limit walking, stairs, squatting, or rising from a chair, it is time for evaluation.
Early assessment helps us identify risks, order imaging only when needed, and start focused physiotherapy. Many knees respond well to conservative care when we treat the whole person—not just the X-ray.
Early signs of knee arthritis: what to look for before it gets worse
You may feel a repeatable pattern of discomfort that tells us more than a single bad day. Watch how your symptoms change with activity and rest. Small clues at home help me decide when to examine, image, or start treatment.
Pain that worsens with activity but eases with rest
Most people notice pain after long walks, standing, or climbing stairs. The discomfort usually eases when you sit or rest. If pain returns with routine tasks, tell your doctor.
Stiffness after sitting or in the morning
Stiffness can feel like a “rusty” knee after a car ride, prayer sitting, or on waking. It often clears after a few minutes of movement. Persistent stiffness that limits routines needs evaluation.
Swelling and a full feeling in the joint
Swelling may be visible puffiness or a subtle fullness. Inflammation inside the joint can cause this even without a clear injury. Note how long swelling lasts and what eases it.
Grinding, reduced motion, and wobbliness
Grinding or crackling sounds suggest surface changes, especially with pain and stiffness. You may also find stairs, squatting, or rising from a chair harder than before. A feeling that the joint may give way can come from muscle weakness or joint change and deserves a check.
Simple self-check: track when pain begins, what worsens it, what relieves it, and whether swelling or stiffness lasts beyond a day. Bring these notes to your visit — they guide diagnosis and care.
What’s happening inside the knee when arthritis begins
I’ll describe how the knee’s parts work together and what goes wrong at the start.
The knee is a smooth-moving hinge. Cartilage acts like a cushion and a slick surface so bone glides without friction. That cushion keeps each step quiet and low-impact.
Cartilage wear and why bones may rub
Cartilage can thin with time or after repeated stress. As it roughens, the space between bone ends narrows and movement feels less smooth.
When cartilage loss continues, the closer bone contact raises friction and creates a deep ache during activity.
How inflammation fuels pain and swelling
Inflammation is the lining’s response inside the joint. It can cause swelling, warmth, and stiffness, especially after rest.
Bone spurs and limited movement
Extra bone growth at the edge, called bone spurs, may form where tissues try to adapt. Over time these osteophytes can add a tight feeling and reduce range of motion.
- I reassure patients that early change often means we can protect cartilage and reduce further damage.
- Next I review risk factors so treatment targets the true cause.
Common risk factors that speed up osteoarthritis knee changes
Certain lifestyle and medical factors make joint wear progress faster. I use this list to identify whether a case looks like gradual wear (primary) or follows a clear trigger (secondary).
Age, genetics, and family history
Getting older raises risk, and family history can matter too. I tell patients that age increases chance but does not guarantee severe damage. Genetics explain why some people develop osteoarthritis knee sooner than others.
Weight-related load on the joint
Extra weight raises mechanical load. A simple rule: each pound gained can add roughly four pounds of pressure through the joint while walking. Small weight loss often reduces pain and slows wear.
Repetitive stress from work and habits
Frequent kneeling, squatting, or heavy lifting adds repeated compressive forces. Over years, these tasks can speed surface damage and make symptoms appear earlier.
Sports injuries, meniscus tears, and old fractures
Past injuries—meniscus tear, ligament damage, or a fracture—can change alignment and stability. Even after healing, altered mechanics raise the chance of later osteoarthritis knee changes.
| Risk factor | How it speeds wear | Practical step I recommend |
|---|---|---|
| Age & genetics | Gradual cartilage thinning over years | Regular check-ups and early physiotherapy |
| Weight | Increases joint load; higher pain | Modest weight loss and low-impact activity |
| Repetitive stress | Repeated compression and micro-damage | Modify tasks, use knee pads, strengthen muscles |
| Prior injuries (tear/fracture) | Altered mechanics and uneven load | Assess alignment, targeted rehab, consider imaging |
Takeaway: if you have several risk factors plus persistent discomfort, seek evaluation. I focus on prevention and practical steps first, not blame, so we can protect your joint and slow damage.
How knee arthritis pain feels and how it differs from a strain or sports injury
Some people feel a dull, creeping ache that appears without any single incident to blame. That timeline clue helps me tell apart joint wear and a direct soft-tissue injury.

Gradual onset versus a clear injury event
Arthritis pain tends to build slowly and return with repeated bending or weight-bearing. A strain or sports injuries usually follow a twist, fall, or heavy workout and cause sharp pain right away.
Why weather may make joint pain feel worse
Some people report more pain on cold or rainy days. The exact link is unclear, but joints can feel stiffer when humidity or barometric pressure changes.
- Grinding or creaking suggests joint surface change rather than simple muscle strain.
- A strain often hurts with one specific move; wear hurts across many daily tasks.
- Do not rely on pain drugs for weeks. See a doctor if pain persists.
| Feature | Joint wear | Strain / sports injuries |
|---|---|---|
| Onset | Gradual | Sudden |
| Sensation | Creaking, ache | Sharp, focal |
| Response | Needs structured plan | May improve with rest |
Red flags I watch for include persistent swelling, repeated giving-way, or pain that limits walking. If you notice these, seek assessment so we treat cause, not just symptoms.
Types of arthritis that affect the knee and why the diagnosis matters
Different diseases can damage the knee joint, so identifying which one matters for treatment.
Osteoarthritis versus rheumatoid arthritis
Osteoarthritis is a degenerative disease where cartilage wears down over time. It causes pain with use and changes in joint mechanics.
Rheumatoid arthritis is an autoimmune condition. It causes more inflammation, often affects many joints, and needs medical therapy that controls the immune system.
Post-traumatic arthritis after ligament or cartilage injuries
Injuries to ligaments, meniscus, or bone can change how the joint moves. Even years later, altered load can cause gradual cartilage loss and pain.
Other important causes I rule out: gout and joint infection
Gout gives sudden, very painful flares from crystal deposits. It needs different medicines to control crystals and inflammation.
Septic arthritis is an infection inside the joint. It causes severe pain, warmth, redness, fever, and often limits weight bearing. This is time-sensitive and requires urgent evaluation, joint fluid testing, and antibiotics.
- I rule out these causes because each one needs a unique plan—exercise and braces suit wear, immune therapy suits inflammatory disease, crystals need metabolic care, and infection needs urgent treatment.
| Type | Key feature | Typical treatment focus |
|---|---|---|
| Osteoarthritis | Degenerative cartilage loss, activity-related pain | Load reduction, physiotherapy, weight management |
| Rheumatoid arthritis | Autoimmune inflammation, multiple joints | DMARDs and specialist medical care |
| Post-traumatic | After ligament/meniscus injury or fracture | Rehab, alignment assessment, targeted surgery if needed |
| Gout / Infection | Crystal flares or septic joint with fever | Crystal control or urgent antibiotics/drainage |
I reassure patients that many cases are manageable once we identify the correct type and start the right plan early. If you notice severe swelling, fever, or inability to bear weight, seek prompt care.
How I diagnose knee arthritis accurately at Boss Multispeciality Hospital
At Boss Multispeciality Hospital I start every assessment by listening carefully to your story and current limits. I ask when pain began, what makes it worse, what helps, any past injuries, and family history. This helps me decide which tests truly matter.
My physical exam checks swelling, local tenderness, range of motion, stability, gait, and crepitus. I watch how you walk and perform simple stability moves. These findings guide whether imaging or lab work is needed.
- X-ray: shows joint space narrowing and bone spurs and helps confirm osteoarthritis patterns.
- MRI: reserved when X-rays are unclear or when we suspect cartilage, meniscus, or ligament damage.
- Blood tests: used when I suspect rheumatoid arthritis or elevated inflammation (ESR/CRP).
- Joint aspiration: performed when gout or infection is possible; fluid analysis finds crystals or bacteria.
| Test | What it shows | When I order it |
|---|---|---|
| X-ray | Joint space, bone spurs | Initial evaluation to confirm osteoarthritis |
| MRI | Cartilage, meniscus, ligaments | If pain or instability is unexplained on X-ray |
| Blood tests | Inflammation markers, rheumatoid factors | Suspected inflammatory disease |
| Joint fluid test | Crystals, infection | Acute swelling, fever, or sudden severe pain |
I practise in Bangalore (Magadi Main Road, near Kamakshipalya and RR Nagar) and focus on accurate diagnosis while avoiding unnecessary tests. A correct diagnosis lets me tailor the right treatment for your joint, bone, and cartilage health and prevent overtreatment.
How to start treatment without surgery and protect your cartilage
Begin with simple steps that reduce stress on the joint and build strength. My goal is to ease pain while keeping you active and independent.
Activity changes that keep you moving
Limit deep squats, high-impact jumping, and repeated stairs for a while. Avoid complete rest—muscles need use to support the joint.
Physiotherapy and strengthening
I use guided therapy to strengthen muscles around the hip and thigh. Stronger muscles reduce load on cartilage and improve walking confidence.
Low-impact exercise choices
Choose cycling, swimming, or graded walking plans. These exercises preserve fitness without heavy joint pounding.
Weight, medications and support
Modest weight loss lowers mechanical stress and often cuts pain. Use OTC pain relievers or prescribed medications for short periods under my guidance.
Supportive braces and proper footwear can shift load and ease discomfort during daily tasks.
| Approach | Main benefit | Typical use |
|---|---|---|
| Physiotherapy | Strengthen muscles, improve mobility | Core therapy for most patients |
| Low-impact exercise | Maintain fitness, reduce pain | Cycling, swimming, walking plans |
| Weight management & support | Lower joint stress and pain | Diet, braces, footwear advice |
Practical home steps—ice after activity, pacing tasks, and tracking triggers—help you stay in control. Conservative treatments often improve function, but progress varies for each person.
When injections make sense and what to expect
When non-surgical care still leaves you with limiting pain, I may suggest an injection as part of a wider treatment plan. Injections can help you reduce inflammation or improve joint comfort so physiotherapy and activity changes work better.
Corticosteroid injections for inflammation flares
Corticosteroid injections calm joint inflammation and often ease swelling quickly. I use them for short-term relief during a flare so you can do rehab and regain movement.
Expect benefit for weeks to a few months. Repeat injections are possible but limited to avoid harm to tissues and cartilage.
Hyaluronic acid “gel” injections for lubrication
Hyaluronic acid injections act like extra joint lubrication for selected osteoarthritis patients. They may reduce friction and help some people walk or climb stairs more comfortably.
Patient selection matters: younger, active people with mild-to-moderate wear tend to get the most consistent benefit.
Platelet-rich plasma: where the evidence stands
Platelet-rich plasma (PRP) injections are promising in some studies, but results vary by preparation and technique. I discuss PRP honestly: it may help some patients, yet outcomes are not guaranteed.
- When to consider injections: persistent pain despite therapy, or a flare limiting daily tasks.
- Realistic expectations: relief ranges from weeks to months and differs per person.
- Safety basics: sterile technique, brief post-injection rest, and call me for redness, fever, or worsening pain.
| Type | Main goal | Typical duration |
|---|---|---|
| Corticosteroid | Reduce inflammation | Weeks–months |
| Hyaluronic acid | Improve lubrication | Months in selected cases |
| Platelet-rich plasma | Support healing response | Variable; evidence mixed |
I use injections as one component of care, not a replacement for strengthening, weight management, and lifestyle measures. Together, these treatments aim to control pain and preserve function so you can stay active.
When surgery becomes necessary, including total knee replacement
When daily tasks become hard despite dedicated therapy, I discuss surgical options with patients. Surgery is a considered step, not a first-line choice. I recommend it when structured treatment, weight loss, medicines, and physiotherapy no longer control pain or restore function.
How I decide you may need surgery
Key reasons include persistent pain that limits walking, visible deformity (bowing), repeated giving-way, or major loss of daily function. I require exam findings and imaging to match symptoms before advising an operation.
Procedures I may consider
- Arthroscopy only for mechanical issues like loose bodies or recent trauma.
- Osteotomy to realign the bone when damage is focused to one side.
- Partial or total knee replacement when wear is advanced and broad relief is needed.
Partial versus total replacement and outcomes
Partial replacement swaps one compartment and preserves more bone. Total knee replacement replaces the surfaces across the joint. Both aim to reduce pain and improve mobility. Expect meaningful improvement, not a “young” joint, and remember results vary.
| Procedure | Main goal | Who may benefit |
|---|---|---|
| Arthroscopy | Remove loose fragments, relieve locking | Selected patients with mechanical blockage |
| Osteotomy | Shift load away from damaged side | Younger patients with single‑side wear |
| Total/Partial replacement | Stop bone‑on‑bone rubbing; restore alignment | Advanced osteoarthritis with lost function |
Recovery and why outcomes vary
Rehab guides the result: early movement, swelling control, progressive strengthening, and gait training. Recovery timelines differ with age, weight, pre‑op stiffness, muscle strength, and other health issues. When surgery is truly needed, proper timing and consistent physiotherapy often restore independence for many patients.
Conclusion
Simple, repeatable changes in how your joint feels can guide an effective plan for care.
Recurring knee pain with activity, stiffness after sitting or on waking, visible swelling, or reduced confidence on stairs are patterns worth noting. These features often reflect gradual wear and local inflammation that produce discomfort and reduced motion.
Not every ache is arthritis, so a correct diagnosis matters. Start by easing unnecessary stress on the joint, keep gentle movement, begin a targeted exercise plan, and work on sustainable weight loss if needed.
Many people improve with lifestyle changes, physiotherapy, and focused non-surgical treatment. Outcomes depend on your body, activity, and exam findings. If you’d like a proper orthopedic evaluation, book an appointment with me — Dr. Lokesh Chowdary R at Boss Multispeciality Hospital, Magadi Main Road (near Kamakshipalya and RR Nagar), Bangalore.