Achilles Tendonitis in Runners: Prevention and Recovery Tips

Have you ever wondered why a small ache at the back of the heel can stop your running so quickly?
I’m Dr. Lokesh Chowdary R (MBBS, MS – Orthopaedics), Managing Director and Senior Orthopedic Surgeon at Boss Multispeciality Hospital on Magadi Main Road, Bangalore, near Kamakshipalya and RR Nagar.
I see this pattern often: sudden training changes overload the tendon and bring pain. Most cases improve when we diagnose correctly and manage load carefully.
I prefer non-surgical care first, guided physiotherapy, and step-by-step return to running. Surgery is reserved only for cases that do not respond to structured rehab.
I will explain why many call it “achilles tendonitis” but why some of these problems behave more like tendinopathy. You’ll get practical advice on reducing overload, keeping fitness safely, and rebuilding strength over time.
If you feel worse, have sudden swelling, or cannot weight-bear, stop self-care and seek an appointment so we can confirm the diagnosis and tailor a plan for you.
Understanding the Achilles tendon and why runners overload it
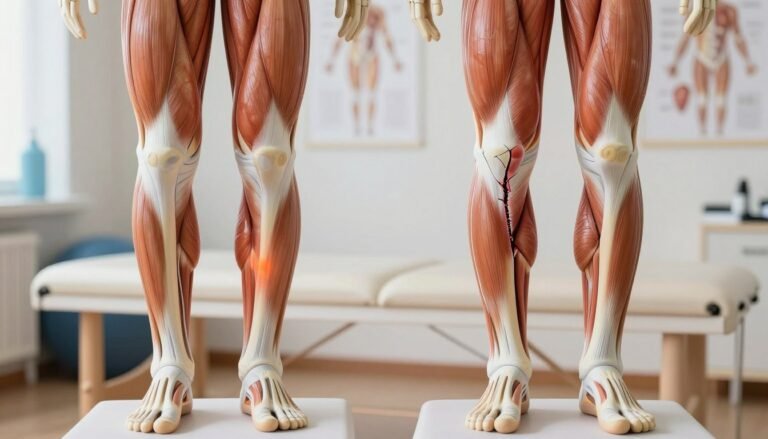
A powerful connector between calf and heel stores energy and releases it every time you run. I use plain clinic language to explain what I look for and why load matters.
What the structure does at the foot and ankle during push-off
The achilles tendon links calf muscles to the heel bone and acts like a strong cable during push-off. It helps the foot and ankle store elastic energy and then return it as you leave the ground.
Why running loads matter
During running the tendon can face about five to eight times your body weight. That means small training increases, extra body weight, or poor recovery can quickly raise tendon stress.
Tendonitis versus tendinopathy — my clinical view
Many painful cases are not classic inflammation. I often call these tendinopathy because the tissue has failed to adapt, not because it is mainly inflamed.
This matters for treatment. If the problem is failed adaptation, the plan focuses on graded loading, calf capacity building (including the gastrocnemius), and sensible rehab rather than only rest or pills.
Common causes of Achilles pain in running
Most painful flare-ups begin slowly, after several days or weeks of extra load, not a single misstep. Identifying the real cause helps prevent repeat problems and speeds recovery.
Training errors that trigger overload
I see this most often: a rapid rise in weekly mileage, adding speed sessions too soon, or stacking hard workouts without rest. These changes increase tendon load and raise the risk of injury.
Footwear, surfaces and sudden changes
Switching shoes abruptly—say from cushioned trainers to minimal footwear or spikes—can increase stress at the heel quickly. Hills, slanted roads, track work, and uneven paths also raise demand even if distance stays the same.
From hip to foot: biomechanics that matter
Poor control at the hip or knee — such as hip drop or inward knee rotation — changes how each stride loads the tendon. Weak or unstable foot control can focus stress on one area and increase recurrence risk.
Calf muscle tightness
Tightness in the gastrocnemius or soleus alters ankle motion and raises tendon stress. I often assess calf flexibility and leg strength because simple stretches and progressive loading reduce long-term risk.
- If pain persists, get an assessment rather than guessing — a targeted plan prevents recurrence.
Symptoms to watch for and when it’s more than “normal soreness”
Not all heel discomfort means a simple muscle ache—some patterns point to a more serious problem. I look for specific signs that suggest overload rather than routine training fatigue.
Morning stiffness, stair pain, and the “warms up then returns” pattern
Classic symptoms include stiffness on waking and soreness when climbing stairs. Many people report pain that eases with a short warm-up but returns later or the next morning.
Where you feel it: mid-portion vs insertional near the bone
Location matters. Mid-portion pain often occurs 2–6 cm above the heel and responds to different exercises than insertional pain at the heel bone. I ask you to point to the exact area during assessment.
Thickening, swelling, and tender nodules along the tissue
You may notice swelling, a thicker feel, or small tender nodules. These changes do not always mean a tear; they often reflect the tissue adapting or failing to adapt.
Reactive, dysrepair, and degenerative patterns — what they mean for recovery
I explain the continuum: reactive → dysrepair → degenerative. Early reactive cases usually improve faster. Degenerative changes can take longer and need structured load management.
- If pain sharpens, function drops, or swelling increases, stop self-testing and get an assessment.
- Many cases improve with graded care, but the exact recovery time varies by person and tissue state.
How I diagnose Achilles problems and rule out other injuries
When heel pain brings your training to a halt, the right questions reveal the real problem fast. I rely on a clear history and a focused exam to separate tendon overload from other causes.
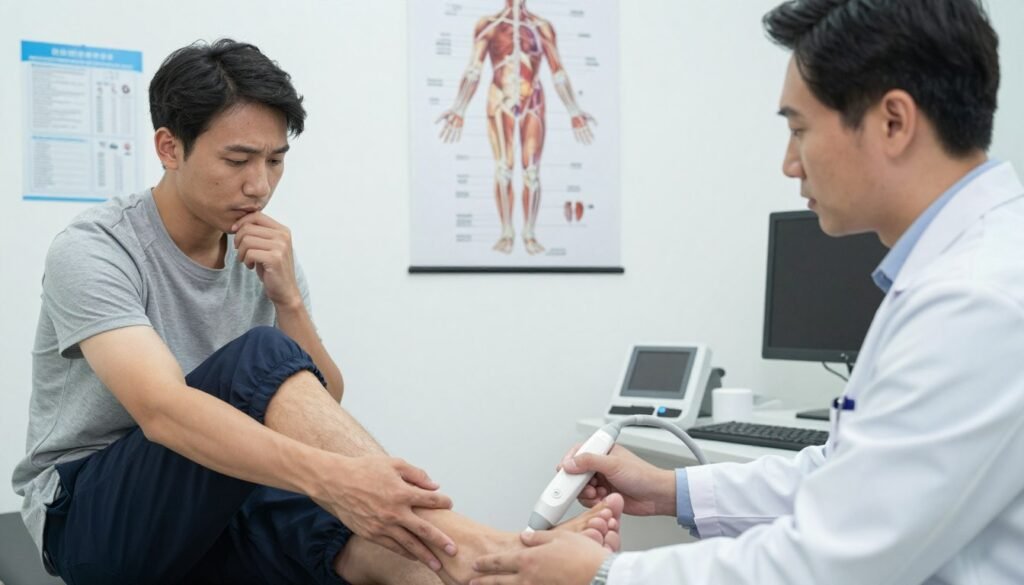
Key history questions about training and daily activity
I ask about weekly running amount, recent intensity changes, and any new hill or track work. I also check for shifts in day-to-day activity that raise load on the legs or feet.
Hands-on exam: what I check
I palpate the tendon for focal tenderness, thickening, and to determine mid-portion versus insertional position. I test calf strength and endurance because weak calf muscles let the tendon face too much load.
- Foot posture and how your feet load the ground.
- Ankle range of motion that can move stress onto the tendon.
- Leg alignment and knee control, which alter strain during each step.
- Simple functional exercises to observe pain response and capacity for strengthening work.
Conditions that mimic tendon problems
Some injuries look like tendon pain but need different care. Retrocalcaneal bursitis, tenosynovitis, and insertional problems at the bone can change the plan. Haglund’s deformity, a bony prominence, is one clear example where treatment differs.
Accurate diagnosis guides non-surgical care and speeds recovery. If symptoms persist, come in for an orthopedic review and a physiotherapy plan tailored to your exam and activity.
Immediate steps to reduce pain and protect the tendon
Immediate steps can lower pain quickly and stop further damage while you plan rehab. I focus on short-term measures that protect the tendon but keep you active where safe.
Smart rest and safe cross-training
Smart rest means cutting high-impact load, not total inactivity. Reduce running and replace it with low-impact options that suit your foot ankle comfort.
- Cycling, swimming, and elliptical work well while you keep fitness.
- Adjust the amount and weight-bearing tasks at work to reduce daily load.
Ice, medications, and short-term supports
Apply ice to the most painful area for up to 20 minutes at a time, several times a day, and stop sooner if the skin goes numb. NSAIDs can ease pain and reduce inflammation-like swelling for short periods, but they do not fix tendon thickening and should not be used long-term without review.
| Intervention | When I use it | Notes |
|---|---|---|
| Heel lift / shoes | Early pain from heel irritation | Small lift and supportive shoes reduce strain |
| Walking boot | Severe pain limiting walking | Short-term only to avoid calf weakness |
| Night splint | Prominent morning stiffness | Holds ankle to ease morning heel pain |
I tailor these choices to each person. If symptoms don’t improve, seek a focused exam so we can plan the next rehab steps.
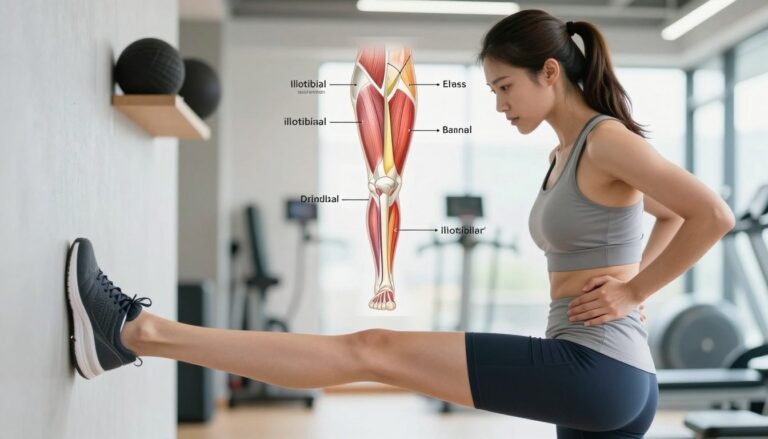
Physiotherapy-guided recovery: exercises that rebuild calf and tendon strength
Rebuilding calf and tendon strength needs a plan that balances challenge with safety. I use stepwise loading so the tissue adapts instead of staying irritated.
Why load management is the real treatment, not complete inactivity
The tendon needs controlled stress to remodel. Complete rest removes that stimulus and delays recovery.
I dose activity based on pain, function, and how you respond the next day. That next-day response guides the next step.
Isometric heel raises for pain control and early strengthening
Start supported heel raises holding 10–15 seconds. Build time to 30–45 seconds as pain allows.
Perform short sets with good alignment and test tolerance before adding load or reps.
Eccentric heel drops and how to do them slowly and safely
For mid-portion problems I add slow eccentric drops. Lower the heel over 3–5 seconds, controlled and pain-monitored.
Avoid rapid drops and stop if sharp warning pain appears. I change knee position—straight to target gastrocnemius, bent to target deeper calf muscles—based on your exam.
When stretching helps and when it aggravates
Some overloaded tendons dislike long tensile stretches. I decide case-by-case using location and irritability.
If stretching increases next-day pain, we reduce or stop it and use strengthening instead.
Progressing to plyometrics and return-to-run drills
Once symptoms settle, I add short plyometric drills like active plant walk and A-skip. Keep sets brief and focus on position and timing.
Gradual progression teaches the tendon to store and release energy safely before a full return to running.
| Stage | Main goal | Example | Key note |
|---|---|---|---|
| Early | Pain control | Isometric heel holds 10–15 seconds | Build to 30–45 seconds |
| Strength | Load tolerance | Slow eccentric drops 3–5 seconds | Mid-portion cases only |
| Return | Power and timing | Active plant walk, A-skip drills | Short sets, monitor next-day response |
achilles tendonitis runners: how to know if you should run and how to return safely
Deciding whether to try a short run after heel pain needs clear, simple checks. I use a stepwise approach that protects the tissue while keeping fitness where safe.
Simple functional checks I use before allowing a trial run
I require a pain-free walk first. If walking is comfortable, I ask for 20 double-leg heel raises without sharp pain.
Next, try 10–15 controlled single-leg hops. These tests show if the tendon tolerates load and quick changes in force.
How to restart with short minutes, monitor the next-day response, and progress
If the checks pass, begin with a short trial run—about 5 minutes or short run-walk intervals. Keep effort easy and time brief.
Record a simple diary and check the next day for increased stiffness or more pain. The 24-hour response is the best guide to safe progression.
Prevention habits, ESWT, and when surgery is discussed
Progress the amount of running slowly. Avoid sudden mileage increase, keep consistent shoes, and maintain regular calf strength work to reduce relapse risk.
In chronic cases that fail months of rehab, ESWT can help when paired with a structured loading program. Surgery is considered only after well-followed non-surgical care for around six months or when bone or major tendon damage is suspected.
| Check | Pass criteria | Next step |
|---|---|---|
| Pain-free walk | No sharp heel pain | 20 heel raises test |
| Heel raises | 20 reps without sharp pain | Single-leg hops test |
| Single-leg hops | 10–15 controlled hops | 5 minutes easy run / run-walk |
| 24-hour response | No worse stiffness or increased pain | Gradual increase in minutes and load |
Conclusion
I recommend a non-surgical-first plan that protects the tissue, reduces overload, and builds strength in a stepwise way.
The achilles tendon links the calf to the foot and works with the whole leg and back. Lasting recovery needs attention to body control, not just one sore area.
Respect warning symptoms such as morning stiffness, focal pain, or a thickened area. Adjust training, use the right exercises, and judge progress by next-day response rather than pushing through pain.
Healing times vary by injury stage and daily stress. If symptoms persist or you need a tailored plan, book an appointment with me, Dr. Lokesh Chowdary R, at Boss Multispeciality Hospital on Magadi Main Road, Bangalore (near Kamakshipalya and RR Nagar).