IT Band Syndrome: Causes, Symptoms, and Stretching Solutions
Have you ever wondered why the outside of your knee hurts more after a run or a long ride, even when you feel strong otherwise?
I’m Dr. Lokesh Chowdary R (MBBS, MS – Orthopaedics), Managing Director and Senior Orthopedic Surgeon at Boss Multispeciality Hospital, Magadi Main Road, Bangalore. In my clinic near Kamakshipalya and RR Nagar I first seek a clear diagnosis so we avoid wasted time on random advice.
iliotibial band syndrome is a common overuse issue where fascia rubs on bone, causing irritation and swelling. Athletes face higher risk, but most people recover without giving up sport.
My aim here is simple: help you spot early signs, explain likely causes, and share a safe step-by-step IT band syndrome treatment plan that favors non-surgical care and physiotherapy-guided recovery. Surgery is reserved only when truly needed.
Recovery varies by severity, training load, and body mechanics. Read on to learn home stretches, strengthening tips, and how to return to running or cycling without flare-ups.
What I mean by IT band syndrome and why it causes outside knee pain
You may feel a rubbing or catching sensation at the outside of your knee when you jog or climb stairs. I explain this calmly in clinic so you know what to expect and where pain comes from.
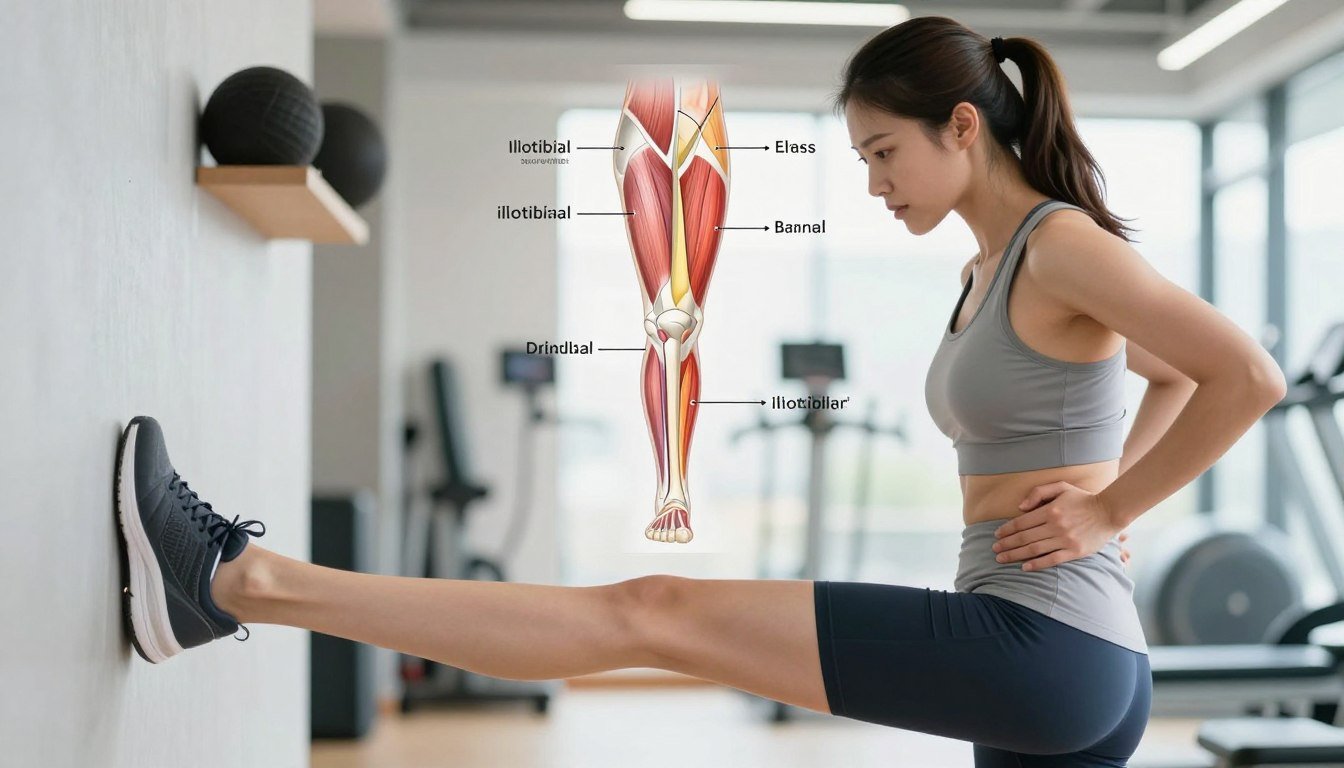
The iliotibial band and its role in hip and knee stability
The iliotibial band is a strong strip of fascia down the outer thigh. It helps stabilise the hip and the knee when you walk, run, or climb.
How friction and bursa irritation create pain and swelling
When the band repeatedly glides over the lateral knee, friction can irritate the nearby bursa. That irritation causes local swelling, tenderness, and a sharp or burning pain with activity.
Outside hip pain and trochanteric bursitis connections
- Rubbing can also happen near the greater trochanter, producing outside hip pain that mimics trochanteric bursitis.
- Weak hip control or poor alignment at the hip knee junction often makes symptoms worse at the knee hip side.
- Many patients improve with rest, but persistent or unusual pain needs careful evaluation.
Common causes I see in runners, cyclists, and active people in India today
Repeated knee flexing during long sessions can slowly overload the outer knee and cause gradual irritation.
Overuse from repetitive knee bending
Activities like running, cycling, and hiking mean many knee bends. Each bend adds friction at the lateral knee and can inflame the bursa over weeks.
Training mistakes that overload the leg
Sudden jumps in distance or intensity, back-to-back hard sessions, and trying to run through early pain are common errors. Proper pacing of training steps and rest prevents setbacks.
Running surfaces, hills, and banked roads
Uneven pavements, steep flyovers, and sloped roads change lateral loading. In many Indian parks and streets, these surfaces increase strain and spark outside knee symptoms.
Shoe support issues and worn footwear
Flat soles, poor arch support, or old shoes alter foot alignment. Misalignment travels up the leg and raises risk of overuse injury.
| Cause | Why it matters | Common sign | Quick fix |
|---|---|---|---|
| Repetitive bending | Builds friction at lateral knee | Aching after runs | Reduce volume; pace steps |
| Sudden training jump | Overloads muscle control | Sharp flare on activity | Cut intensity; add rest day |
| Banked or uneven surfaces | Shifts lateral stress | Worse on hills | Change route; avoid slopes |
| Worn shoes | Alters foot and hip alignment | Uneven wear patterns | Replace shoes; check foot support |
Symptoms and early warning signs you shouldn’t ignore
Notice a burning ache along the outer thigh or the side of your knee during longer runs or rides? That early discomfort is often the clearest symptom to watch for.
I look for a typical pattern: a sharp or burning pain on the outside of the knee that may radiate up the thigh or to the side of the hip.
Typical pain pattern along the outside knee, thigh, or hip
Pain usually appears later in a session and eases with rest at first. Over time it can start earlier and last after exercise. Tenderness to touch and occasional warmth or mild redness may be present.
Clicking or popping sensations during movement
Some patients report clicking or popping at the outside knee or hip. When this comes with local pain and a repeatable position, it often reflects friction from the band and merits assessment.
How symptoms change as the condition progresses
Left unchecked, mild late-activity soreness can become earlier pain, lingering soreness, and reduced tolerance for stairs or long walks. Severe swelling, locking, or true instability points to a different condition and needs prompt evaluation.
- I advise early evaluation so recovery is achievable with the right steps.
- Use these signs as an early warning system rather than a reason to panic.
Risk factors and body mechanics that make IT band syndrome more likely
Certain patterns of movement and weakness raise the risk of outside knee pain. I explain these in plain language so you can see why a clinical check is helpful before assuming a simple fix.
Hip abductor and glute weakness
When the hip abductors and glute muscles are weak, the pelvis and thigh drift inward as you run or climb. That shift increases tension across the lateral thigh and the knee with each step.
Tight muscles and reduced flexibility
Tight outer-thigh and hip muscles limit glide and make friction more likely. Stretching and soft-tissue work often form part of my plan to restore smooth movement.
Foot pronation, ankle control, and gait
A foot that rolls inward or poor ankle control alters knee tracking. Small gait faults repeated thousands of steps can cause overload higher up the leg.
Structural factors and arthritis
Leg-length differences, bowed legs, or knee arthritis may mimic or worsen symptoms. I recommend assessment so we separate true degenerative knee pain from a mechanically driven band issue.
| Factor | Why it matters | What I check |
|---|---|---|
| Weak hip muscles | Alters thigh alignment | Single-leg squat |
| Tight outer muscles | Reduces glide | Flexibility tests |
| Foot/ankle control | Changes load at knee | Gait and shoe review |
| Structural issues | Mimic or worsen pain | Leg-length and X-ray if needed |
How I diagnose IT band syndrome in the clinic
I begin by asking when the pain started and which activity brings it on. I want to know recent changes in training and how long symptoms settle after you stop.
History questions I ask about pain, training load and recovery time
I ask about the type of activity (running or cycling), how much you do, any sudden increases, and rest days. I also check how quickly swelling or soreness eases with rest and time away from activity.
Physical exam focus: tenderness, swelling, alignment and range of motion
I palpate the exact spot of tenderness at the outer knee and note any swelling or bruising. I assess hip and knee alignment, leg-length differences, and range of motion while you stand and walk.
Ober test and what it tells me
The Ober test is a simple test I use to check iliotibial band tightness. A positive result suggests tightness that may be adding to your pain and reduced glide.
When I order X-ray or MRI
I rely on history and exam first. I request an X-ray if I suspect arthritis or bony alignment issues. I choose MRI when soft-tissue detail will change management or if the condition is unclear.
| Step | What I look for | Why it matters |
|---|---|---|
| History | Onset, activity, training changes | Guides diagnosis and time to recovery |
| Exam | Tenderness, swelling, alignment, ROM | Pinpoints source of pain and dysfunction |
| Ober test | Band tightness | Shows lateral tightness that may need therapy |
| Imaging | X-ray or MRI if needed | Rules out other knee or hip conditions |
IT band syndrome treatment: step-by-step non-surgical plan I usually start with
Managing lateral knee pain starts with simple, staged steps that calm irritation while keeping you active. I prioritise conservative care and tailor each plan to the person’s goals and exam findings.
Relative rest and activity change
I advise relative rest: stop the specific activity that triggers pain and replace it with low-load exercises like swimming or walking. This reduces friction and swelling without losing fitness.
Pain control: ice and short-term medicines
Apply ice for 10–15 minutes after activity and consider short courses of NSAIDs if safe. I caution people with stomach or kidney issues to check with their doctor first.
Physiotherapy goals and progression
Therapy focuses on reducing tension, improving hip control, and guided stretch and strengthening exercises. Gradual loading and gait retraining reduce recurrence.
When injections are considered
If inflammation persists after a well-followed conservative plan, a corticosteroid injection may be used selectively to speed calming before continued rehab.
| Step | Action | Purpose | Typical weeks |
|---|---|---|---|
| Initial | Relative rest, ice, NSAIDs | Calm irritation and swelling | 1–2 weeks |
| Rehab | Physiotherapy: stretch & strengthen | Improve control, reduce friction | 4–8 weeks |
| Escalation | Consider injection if needed | Control persistent inflammation | After 2–6 weeks of rehab |
Stretching solutions and home exercises that support healing
I offer simple, safe moves you can do at home to ease lateral tightness and build control. Stretching works best when paired with strengthening and careful load management, not as a stand-alone fix.
How to do a glute stretch safely
Lie on your back. Cross the affected leg over the other so the ankle rests on the opposite knee. Gently draw the uncrossed knee toward your chest until you feel a calm stretch in the glute.
Hold 20–30 seconds. Repeat 2–3 times. Stop if the move causes sharp pain.
Standing outer-thigh stretch for lateral tightness
Stand tall and cross one foot behind the other. Lean the hip of the back leg toward the same side until you feel a mild pull along the outer thigh. Keep your torso upright so the stretch is in the correct position.
Foam roller technique: what to do and what to avoid
Place the roller under the outside of the thigh and use slow, short rolls. Spend 30–60 seconds along tender spots. Avoid pressing hard over sharp pain or bruised areas. Do not roll directly over the knee joint.
Hip abduction strengthening to protect the knee and hips
Try side-lying leg lifts or standing band walks with light resistance. Do controlled 10–15 reps, 2–3 sets. Strong hip muscles reduce load on the iliotibial band and protect the knee during runs or rides.
Gym option: hip abductor machine basics
Use low weight and slow movement. Sit with the pads over the outer thighs, keep a neutral spine, and squeeze gently on the outward phase. Quality reps matter more than heavy load.
| Exercise | Duration/Reps | Purpose | Caution |
|---|---|---|---|
| Glute stretch | 20–30s ×3 | Release hip muscles | Stop if sharp pain |
| Standing outer-thigh | 20–30s ×2 | Target lateral tightness | Keep upright position |
| Foam roller | 30–60s | Soften tight part | Avoid rolling over knee |
| Side-lying lifts | 10–15 reps ×3 | Strengthen hip abductors | Controlled motion only |
How to return to running, cycling, and sport without flare-ups
Before you lace up again, a short plan can help you return to sport without repeating the same pain. I focus on slow progress, listening to your body, and practical changes that lower risk.
Gradual return principles and pacing your steps week by week
Only restart when daily walking and stairs are comfortable with no lingering knee pain. Begin with 2 short sessions in the first week and increase by one session or 10% distance per week.
Use pain as your guide: mild ache that settles within a few hours is acceptable; sharp or increasing outside knee pain means step back and add more rest.
Cross-training choices that reduce knee friction while keeping fitness
Choose low-load options such as swimming, pool running, and cycling on flat routes. These activities maintain aerobic fitness while lowering repeated lateral stress on the knee.
Practical shoe and surface changes to lower risk
Check shoe wear and replace running shoes every 300–500 miles. Worn soles change foot and ankle mechanics and raise risk to the knees.
| Change | Why it helps | Practical tip |
|---|---|---|
| Shoes | Restore support and alignment | Replace shoes at 300–500 miles |
| Surfaces | Reduce uneven lateral load | Prefer flat tracks and even pavements |
| Training pace | Allow tissue adaptation | Increase distance slowly over weeks |
If pain returns quickly, swelling increases, or your symptoms change, please come back for reassessment. I prefer to prevent recurrence rather than rush a full return.
When surgery is considered and what recovery may involve
If months of rehab and sensible load changes leave you with ongoing pain, surgery may enter the discussion. I view surgery as a last resort and explain options without creating undue alarm.
Failed conservative care means persistent symptoms despite a well-followed plan, clear correction of training errors, and at least six months of guided rehab and biomechanical work. When imaging and exam point to a discrete source that keeps causing friction, then I consider operative options.
Possible procedures and what each does
- Arthroscopic excision of the inflamed bursa to remove the painful tissue and reduce irritation.
- Lengthening of the iliotibial band to lower tension and lessen rubbing over the lateral knee.
- Partial excision of a degenerative portion when a localized, damaged part contributes to the condition.
Recovery timeline and rehabilitation
After surgery, recovery often takes longer than non-surgical care. Early healing is measured in weeks, but full return to sport commonly requires up to three months with staged rehab.
Rehab focuses on restoring mobility, strengthening hip and thigh control, and a graded return to running or cycling. Rushing back can reintroduce friction or new problems, so I emphasise slow progression and close follow-up.
| Procedure | Main goal | Typical recovery time |
|---|---|---|
| Bursa excision | Remove inflamed tissue | 6–8 weeks initial, full activity ~10–12 weeks |
| Lengthening | Reduce lateral tension | 8–12 weeks progressive rehab |
| Partial excision | Remove damaged part | 8–12 weeks; sport-specific progression |
Decisions are individual. I consider your goals, exam findings, and response to therapy before recommending any operation. Proper rehab and realistic time frames give the best chance of lasting recovery.
Conclusion
Simple changes can make a big difference. Iliotibial band syndrome is a common, treatable condition that often causes outside knee and hip pain. Most people improve with rest, ice, guided therapy, and a gradual return to activity.
Focus first on reducing irritation, then rebuild strength and flexibility for the leg and hip. Respect early symptoms and avoid training errors that repeat overload. If pain or swelling persists, seek a timely review rather than self-managing for months.
If you need a clear plan, book an appointment with me, Dr. Lokesh Chowdary R (MBBS, MS – Orthopaedics), at Boss Multispeciality Hospital on Magadi Main Road, Bangalore (near Kamakshipalya and RR Nagar). I will confirm the diagnosis and help you return to sport safely.







