Muscle Strains vs Muscle Tears: Understanding the Difference
Have you ever wondered why a sudden ache after exercise can mean anything from a mild pull to a serious rip?
I’m Dr. Lokesh Chowdary R (MBBS, MS – Orthopaedics), Managing Director and Senior Orthopedic Surgeon at Boss Multispeciality Hospital on Magadi Main Road, Bangalore, near Kamakshipalya and RR Nagar.
Soft tissue injuries are often mislabeled, and self-diagnosis is unreliable. I hear “muscle strain vs tear” as one of the most common questions from patients after a sudden ache at work, during sport, or after a slip.
Early symptoms can feel similar, so the safest path is to know the difference before pushing through pain. Here I focus on problems of muscle and tendon, while noting that sprains involve ligaments and joints and may need different care.
This article will explain how pulls and rips happen, how signs often differ, and what I look for in an orthopedic evaluation. I emphasize accurate diagnosis, non-surgical care first, physiotherapy-guided recovery, and surgery only when medically necessary.
Many soft tissue injuries improve with timely rest and guided rehab, but recovery varies. By the end, you should know which warning signs need urgent care and which early steps are reasonable at home.
How I Explain Soft Tissue Injuries in the Clinic
When someone walks into my clinic saying they “pulled” something, I start by untangling the words we use. Clear labels help me pick the right treatment and avoid repeated problems.
I explain that sprains are injuries to ligaments that support a joint. I then describe how tendons connect a contracting muscle to bone and how those tissues behave when overstretched.
During overstretching, tiny fibers may lengthen, partially split, or fully rupture. That changes how the area generates force. The body reacts with inflammation, causing swelling, tenderness, and sometimes bruising.
Often the same movement injures more than one structure. That is why I focus on function—how you walk, lift, and move—rather than only the label used casually.
| Structure | Role | Common Signs | Typical Concern |
|---|---|---|---|
| Ligament | Connects bone to bone | Joint pain, instability | Sprains; joint support loss |
| Tendon | Connects muscle to bone | Tenderness, reduced force | Overuse and partial tears |
| Muscle fibers | Produce movement | Cramp, weakness | Fiber splitting or rupture |
| Combined | Joint and movement | Swelling, bruising | Mixed tissue injuries |
I recommend early medical attention when pain or loss of function is significant. Most soft tissue problems respond to conservative care, but correct diagnosis matters for a safe recovery.
Muscle Strain: What It Is and Why It Happens
In clinic I often see people who wake with sudden pain after activity and ask what actually happened inside their soft tissues.
Definition and how it differs from a ligament injury
I define a muscle strain as an overstretching or partial tearing of a muscle or tendon. This affects the contracting tissue that produces movement, not the ligaments that stabilise joints.
Common causes I see
Typical triggers include a sudden sprint, lifting a heavy load at home, poor gym technique, or repetitive work tasks. Overuse and a single overload event both cause damage to muscle fibers and surrounding tissue.
Frequent locations and posture links
Hamstrings and the lower back are common because they absorb load during running, bending, and posture control. I also see shoulder and neck complaints tied to prolonged desk work and phone use that produce back and neck pain over time.
- Grades: mild (stretching), moderate (partial tear), severe (near complete rupture).
- What happens: micro-injury to muscle fibers triggers pain, stiffness, and weakness with movement.
- Early care: rest from the aggravating activity, controlled movement, and guided rehab usually help most recoveries.
| Grade | Typical signs | Recovery expectation |
|---|---|---|
| Mild | Local soreness, minimal weakness | Days to 2 weeks with rehab |
| Moderate | Pain with activity, reduced force | 2–6 weeks with physiotherapy |
| Severe | Marked weakness, difficulty using limb | Longer recovery; specialist review |
I reassure patients that soreness can feel alarming, but with early, individualised non-surgical care most recover well. I tailor rehab to the activity demands so return to work or sport is safe and effective.
Muscle Tear: What It Means When Tissue Actually Ruptures
A loud pop or sudden collapse during activity often signals more than routine soreness. In such moments, the problem may be a true rupture of the soft tissue rather than a simple overstretch.
Definition and seriousness
I use the term to mean a more significant rupture of tendon or contracting fibres. When fibres break, force transmission fails and strength drops quickly.
Typical triggers I see
Common events include an awkward landing, an explosive push-off, or gradual wear that reaches a breaking point. These mechanisms cause sharper pain, notable swelling, and often bruising.
Recognizable examples
- Achilles rupture — sudden calf pain and inability to push off.
- Rotator cuff tears — sharp shoulder pain with weakness overhead.
Some partial tears recover with physiotherapy and careful rehab. In other cases, especially complete ruptures or when function is lost, I may recommend surgery. Surgery is offered only when medically required, after clinical assessment and imaging.
Correct diagnosis is crucial; treating a true rupture like a mild pull can delay healing and cause poorer outcomes in some cases.
muscle strain vs tear: Key Differences You Can Feel
When activity suddenly stops because of a sharp jolt, the feel of the injury often gives a clue to its severity. I use simple patterns of symptoms to guide early decisions and to advise when an exam is needed.
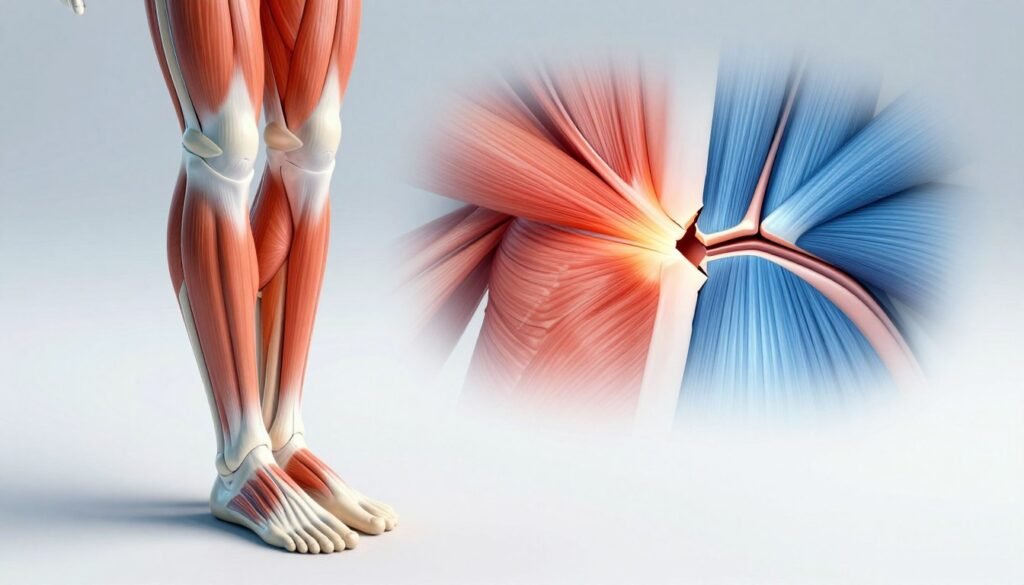
Pain pattern
Often a mild pull begins as soreness, tightness or cramping that grows with use. You may feel aching and some weakness but can usually keep moving.
A true rupture tends to cause sharp, intense pain that forces you to stop immediately. Pain may be severe and sudden.
Swelling and bruising
Mild to moderate swelling can occur with an overstretching injury and small bruises may follow.
Significant swelling and large, spreading bruising suggest more tissue disruption and need prompt assessment.
Function and movement
With less serious injuries you often have pain but retain most movement. Strength may be reduced.
When there is clear loss of normal use, or marked weakness, that points to a more serious problem.
The “pop” or “snap” moment
Hearing or feeling a pop can indicate a rupture. If that happens, stop activity and seek evaluation rather than self-treating.
- I list these patterns so you know what to watch for and when to get checked.
- If pain is worsening, swelling increases, or function drops quickly, see a clinician.
| Feature | Typical mild injury | Typical rupture |
|---|---|---|
| Pain | Soreness, cramp | Sharp, intense |
| Swelling | Mild to moderate | Significant |
| Movement | Limited but usable | Loss of normal use |
Signs and Symptoms I Take Seriously During Evaluation
A sudden change in how you walk or use a limb often gives the first clue about how serious the injury is.
I first watch movement: how you step in, which motions you avoid, and whether you can use the limb safely. That functional view guides what I test next.
Weakness, spasms, and tenderness with milder injuries
Common findings include localized tenderness, brief spasms, cramping, and reduced strength on resisted testing. These symptoms usually point to partial damage rather than full rupture.
Visible deformity or a gap with complete ruptures
When I see an abnormal contour or a visible gap, I worry about a complete rupture. A clear depression or loss of the normal line of the tissue is a strong sign for urgent review.
Red flags that need prompt attention
- Inability to bear weight or use the limb safely.
- Hearing a pop at the time of injury with immediate weakness.
- Rapidly increasing swelling or large bruising around the site.
- Pain that does not improve after a few days despite basic home care.
Early identification prevents further damage and helps me advise safe activity changes. Noting daily changes in symptoms makes my assessment more accurate and speeds recovery.
| Finding | What I look for | Likely concern |
|---|---|---|
| Tenderness & spasms | Local pain with tight bands on touch | Partial damage, rehabable |
| Weakness on testing | Reduced force with resisted movement | Partial or larger fibre involvement |
| Deformity / gap | Visible contour change or depression | Complete rupture; urgent review |
| Swelling / bruising | Rapid spread or large discoloration | Significant damage; imaging may be needed |
How I Confirm the Diagnosis at Boss Multispeciality Hospital
The first step is a clear timeline: what happened, when, and what you cannot do now. I follow a simple pathway at Boss Multispeciality Hospital on Magadi Main Road, Bangalore, near Kamakshipalya and RR Nagar.
History and focused exam
I ask whether you heard a pop, the exact movement that triggered the injury, and which activities cause the most loss of function. I check tenderness, swelling pattern, bruising, and compare strength side-to-side.
Assessing joint stability
I test nearby joints because a painful soft tissue complaint can hide a sprain or combined joint injury. Stability testing rules out related conditions that change treatment choices.
When imaging helps
I order scans when there is major loss of function, suspected Grade III damage, or when symptoms do not match a simple grade I or II case. Clinical exam stays central to planning care.
| Step | What I assess | Action |
|---|---|---|
| History | Onset, pop, trigger movement | Guide urgency and tests |
| Exam | Tenderness, bruising, strength | Grade injury; start conservative care |
| Imaging | Loss of function, deformity | Confirm severe cases; plan surgery if required |
Accurate diagnosis directs treatment. Many injuries improve with home care and physical therapy. Surgery is reserved only for cases that need it after assessment.
Non-Surgical Treatment First: Rest, Ice, Compression, Elevation, and Pain Control
I usually begin conservative care because protecting tissue early often changes the course of healing. Simple measures aim to reduce inflammation, limit further damage, and let function return safely.
R.I.C.E. basics and how to do it correctly at home
Rest from the painful activity; avoid loading the injured area while keeping gentle, pain‑free movement. Apply ice for 15–20 minutes every 2–3 hours on the first 48–72 hours. Use compression (an elastic bandage) to control swelling and elevation above heart level when possible.
Activity modification: how much rest is helpful and what to avoid
Rest does not mean complete immobility. Stop heavy lifting, sprinting, or forced stretches into sharp pain. Begin gentle range exercises as pain allows to prevent stiffness.
Medicines: when over-the-counter options may be used safely
Over-the-counter pain relievers can ease symptoms for a short period. People with chronic conditions or on other drugs should check with a doctor before taking medicines.
Expected recovery timelines
Mild problems often improve in days with proper care. More significant injuries commonly need weeks of guided rehab. Recovery varies by age, fitness, and injury grade.
- Seek review if swelling worsens, pain increases, or you cannot use the limb normally.
| Goal | Home action | Typical time |
|---|---|---|
| Reduce pain | Ice, rest, OTC medicines | Days |
| Control swelling | Compression, elevation | Days to weeks |
| Restore function | Gradual rehab | Weeks |
Physiotherapy-Guided Rehabilitation and Safe Return to Activity
Rebuilding safe movement after an injury takes a plan, patience, and guided therapy. Once acute pain and swelling settle, focused rehabilitation becomes the main tool I use to restore flexibility and strength without re-injury.
Restoring flexibility and strength
I begin with gentle range exercises to regain comfortable motion. Gradual loading follows to rebuild strength and control.
Progression milestones
My staged approach moves from controlled movement to light resistance, then to work- or sport-specific drills. I ask patients to meet simple milestones before advancing.
- Movement: pain-free range and normal walking patterns.
- Load: progressive resistance that restores strength and endurance.
- Activity: drills that mimic job or sport demands.
| Phase | Primary goal | Typical time | Key sign to progress |
|---|---|---|---|
| Early | Reduce pain, regain motion | Days–2 weeks | Pain controlled with movement |
| Strengthening | Restore strength and flexibility | 2–8 weeks | Improved resisted force |
| Return to activity | Work/sport readiness | 4–12+ weeks | Safe, reproducible task performance |
Posture, mechanics, and why recovery time varies
Correcting posture-related issues, workstation habits, and lifting technique reduces recurrence. Recovery time differs by grade of injury, tissue involved, sleep, nutrition, and how consistently you follow physical therapy.
I emphasise patient attention: listen to symptoms, follow milestones, and allow time to heal. My goal is safe, confident movement so you return to daily life and higher activity with lower risk of repeat problems.
Conclusion
Knowing which signs need urgent review helps avoid delays that worsen outcomes.
In short, a mild overstretch usually causes soreness and limited loss of function, while a frank rupture shows sharper pain, rapid weakness, larger swelling, bruising, or a pop at the time of injury.
Correct grading guides the right course: home care and physiotherapy often work well, and surgery is reserved for cases that truly need repair.
Come in if you cannot bear weight, have worsening pain or swelling, visible deformity, or persistent symptoms after a few days.
To book an appointment, see me — Dr. Lokesh Chowdary R, MBBS, MS (Orthopaedics) — at Boss Multispeciality Hospital, Magadi Main Road, Bangalore, near Kamakshipalya and RR Nagar, for diagnosis, treatment planning, and guided recovery.







