What Is Osteoarthritis? Symptoms, Causes, and Stages Explained
I often hear a question that makes patients pause: could simple daily tasks be a sign of progressive joint damage? I ask this because early recognition changes the path forward.
I am Dr. Lokesh Chowdary R, MBBS, MS (Orthopaedics), Managing Director and Senior Orthopedic Surgeon at Boss Multispeciality Hospital on Magadi Main Road, Bangalore, near Kamakshipalya and RR Nagar. Proper evaluation matters, since many causes of joint pain look alike.
Osteoarthritis is a common degenerative joint disease caused by wear of cartilage and underlying bone. It affects hundreds of millions of people—about 237 million were reported in 2015—and usually progresses slowly over years.
In this Ultimate Guide I explain simply why it happens, what it feels like, and how we treat it step-by-step. I cover symptoms, causes, risk factors, stages, diagnosis, and treatments from home care to surgery when needed.
Typical joints involved include the knee, hip, hands, spine, and big toe. My aim is to reduce pain, protect joints, and keep daily life moving. If symptoms affect sleep, walking, or work, seek accurate assessment rather than months of self-treatment.
What is osteoarthritis and why it happens in the joints
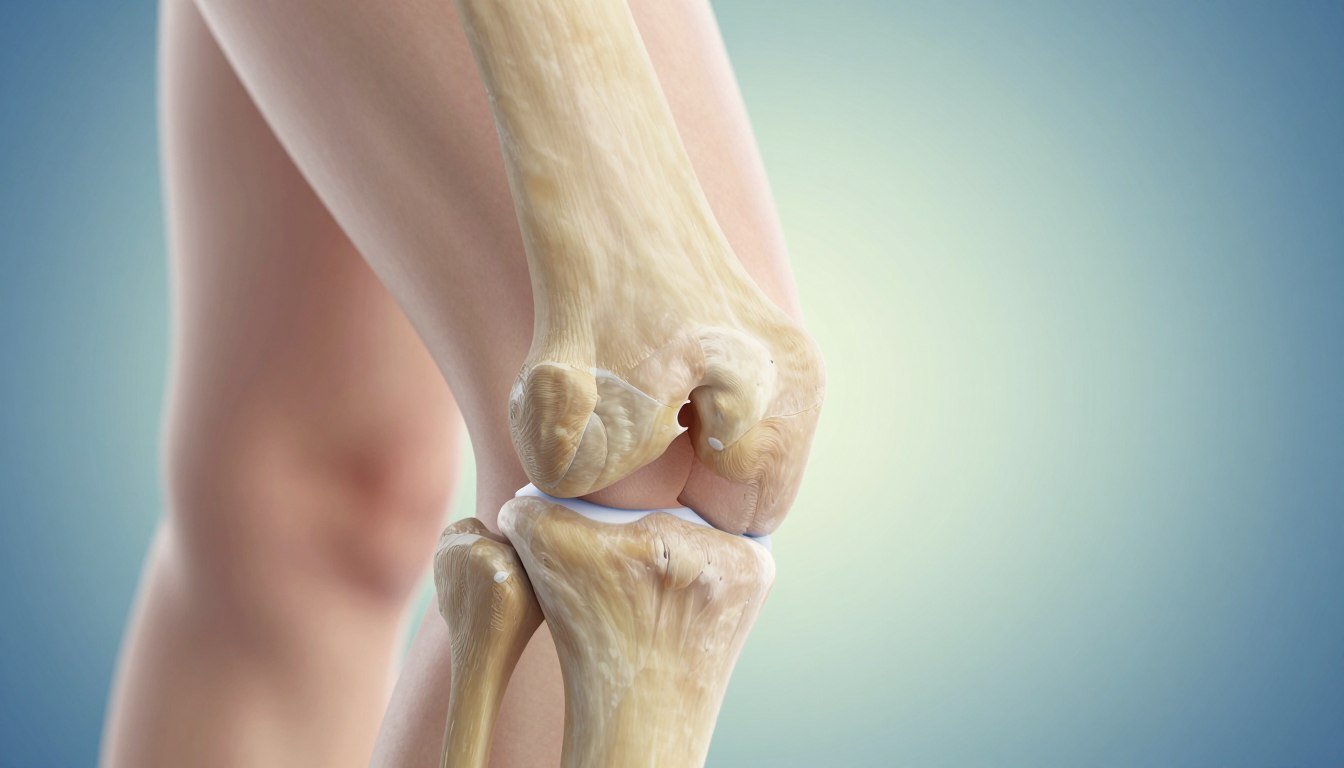
In clinic I explain joint damage simply, using examples people see every day. A healthy joint has smooth cartilage and a thin film of fluid that lets bones glide without pain.
With time the cartilage thins and becomes rough. The bone under the surface also adapts and may form small spurs that change movement. These changes cause stiffness, grinding, and reduced motion.
Not just plain wear and tear
It is tempting to blame everything on wear and tear, but the body’s repair response and low-grade inflammation also matter. Alignment, muscle strength, past injury, and genetics change how the condition progresses.
How this differs from inflammatory disease
Rheumatoid arthritis causes widespread inflammation, warmth, and longer morning stiffness. That needs different tests and early specialist treatment. The common joint problem I see usually affects function more than the whole body.
- Healthy: smooth cartilage, clear fluid, easy motion.
- Early change: cartilage thins, mild pain with activity.
- Progression: rough surfaces, bone spurs, reduced range.
| Feature | Common joint disease | Rheumatoid arthritis |
|---|---|---|
| Main cause | Mechanical stress and low-grade inflammation | Autoimmune inflammation |
| Pattern | Often single or weight-bearing joints | Symmetric, many joints |
| Stiffness | Brief after rest | Prolonged morning stiffness |
How osteoarthritis can affect daily life over time
Daily tasks often shift slowly; patients notice limits only when a routine becomes hard. Over months and years, small changes add up and begin to affect life at home and work.
Why symptoms often progress slowly over years
I see the condition build in stages. At first, people adapt—avoiding squats, skipping stairs, or shortening walks. These choices hide early loss of function.
Progress may pause or even improve for a period. Good days and flare-ups are common and do not always mean rapid decline.
Why joint damage on scans doesn’t always match pain
X-rays and scans show structure, not the full story. Pain depends on inflammation, muscle support, sleep, stress, and how the nervous system senses the joint.
Some patients have mild imaging changes but severe pain. Others have clear structural change yet manage daily life well.
- Common limits: kneeling for prayer, squatting for chores, climbing stairs, long standing at work.
- Pain can fluctuate—plan activity, rest, and simple strengthening to improve function.
- Early evaluation helps protect life routines and avoids needless rest or fear.
| Daily problem | Scan finding | Practical response |
|---|---|---|
| Stairs hurt after long climb | Minor joint-space change | Strengthen quads, pace steps, use rail for support |
| Severe pain with normal X-ray | Little visible damage | Assess inflammation, sleep, and muscle strength; treat symptoms |
| Limited bend but tolerable pain | Advanced cartilage loss | Focus on safe movement, assistive aids, and tailored rehab |
Osteoarthritis symptoms I look for in the clinic
When a patient walks into my clinic, I listen for descriptions that reveal how daily movement feels. Short, concrete details often tell me which symptoms matter most.
Joint pain with use, better with rest
Pain usually worsens after walking, stairs, or long standing and eases with rest. Early on, pain follows activity rather than lasting all day.
Brief stiffness after rest
Morning or “after sitting” stiffness tends to ease within about thirty minutes. That brief stiffness helps distinguish this condition from inflammatory types.
Swelling, warmth, and when to worry
Swelling may feel hard and knobbly from bone changes or soft from extra fluid. Mild warmth can occur; a hot, very red, intensely swollen joint needs urgent review.
Grinding, locking, instability, and muscle change
Crepitus or “crackling” often means rough surfaces; sound alone rarely demands surgery. Locking or catching suggests a mechanical fragment, especially in the knee.
Joints may “give way” from pain and weak muscles. I watch for muscle wasting because strength work gives the best non-surgical benefit.
- Classic pattern: activity-linked pain, short morning stiffness.
- Red flag: sudden severe swelling, fever, or inability to bear weight.
| Sign | Typical finding | Action |
|---|---|---|
| Crepitus | Grinding sound, no fever | Assess range and reassure |
| Locking | Intermittent catching | Consider imaging, refer if persistent |
| Muscle wasting | Thigh or around joint smaller | Start strength program |
Which joints are most commonly affected by osteoarthritis
Different joints tend to show telltale patterns, so I look for clues in how pain starts and where it travels.
Knee pain and stairs
The knee is my most common site. It bears weight and handles twisting forces, so small damage becomes noticeable on stairs, squats, and rising from a chair.
When the patellofemoral area is stressed, pain shows with deep bend. That helps me separate knee surface pain from hip referral.
Hip pain that travels to the groin or thigh
Hip discomfort often presents as groin or front-of-thigh pain. Patients may struggle to get in and out of a car or to cross their legs.
Hands, spine, feet, shoulder, and jaw
Finger joints can grow bony nodes and reduce grip. Heberden’s and Bouchard’s nodes are common exam findings.
Neck and low back changes (spondylosis) can cause local stiffness and nerve symptoms, yet not every back ache is due to these changes.
Foot problems, especially the big toe (hallux rigidus), change gait and can add stress to knees and hips. Shoulders may click; jaw pain can affect chewing and sometimes starts earlier than other joints.
- I use pattern recognition—activity triggers, location, and simple maneuvers—to narrow diagnosis.
- Any joint can be affected, but these common patterns guide targeted treatment in clinic.
| Joint | Typical pain pattern | Exam clue | Practical tip |
|---|---|---|---|
| Knee | Stairs, squatting, bending pain | Crepitus, tenderness around patella | Quad strengthening, pace stair use |
| Hip | Groin or front-thigh pain, car transfer difficulty | Reduced internal rotation, gait limp | Use chair-height aids, targeted hip exercises |
| Hands / Fingers | Grip weakness, nodal bumps at joints | Bony swellings at DIP/PIP | Adaptive tools, hand strengthening |
| Feet / Spine / Jaw | Toe stiffness, back stiffness, chewing pain | Limited toe dorsiflexion; neck tenderness; jaw crepitus | Supportive footwear, posture work, dental/ENT review if needed |
What causes osteoarthritis
I like to show patients that joint stress plus limited repair over time creates a pattern, not a single blameworthy cause. This helps avoid guilt about weight or work while keeping focus on practical steps to protect function.
Mechanical stress, alignment, and low-grade inflammation
Repeated load on a joint concentrates forces on small areas. Bow legs, knock knees, hip shape, or foot mechanics can make this worse.
Low-grade inflammation sits in the background. It is milder than autoimmune disease but enough to cause pain and occasional swelling.
Cartilage thinning, rough surfaces, and osteophytes
Cartilage thins and roughens. That creates the grinding you might feel when moving after a rest.
As cartilage wears, bone adapts and may grow osteophytes (bony spurs). These can limit motion or irritate nearby tissues.
Synovium thickening and extra joint fluid
The lining (synovium) may thicken and make more fluid. That causes soft swelling and a sense of fullness around the joint.
Together, these changes explain pain after activity, stiffness after sitting, and occasional instability. Understanding this lets us target care: reduce load, build muscle support, and control symptoms beyond pills.
- Process: stress + reduced repair → structural change.
- Alignment alters load; correctable in many cases.
- Inflammation is low-grade but actionable.
| Structural change | Patient sensation | Why it happens | Practical response |
|---|---|---|---|
| Cartilage thinning | Grinding, pain with use | Repeated load, poor repair | Strengthen muscles, reduce peak loads |
| Osteophytes | Stiffness, limited motion | Bone adaptation to uneven stress | Mobilization, targeted exercises, injections if inflamed |
| Synovial thickening | Soft swelling, fullness | Low-grade inflammation | Rest, anti-inflammatory measures, assessment |
| Malalignment | Faster localized damage | Bony shape or limb axis differences | Bracing, footwear, surgical options if severe |
Risk factors that increase your chances of developing osteoarthritis
Risk factors quietly shape who develops joint wear and when symptoms appear. I review them to guide prevention and early care.
Age and healing changes
After the late 40s many people show slower tissue repair, small muscle loss, and gradual cartilage change. Early strength work delays decline and helps function.
Weight and joint load
Extra weight raises load on the knee and hip with every step. Even modest weight loss reduces pressure and lowers the chance of faster joint wear.
Prior injury, tears, and surgeries
Past ligament tears, fractures, or joint surgery often speed local joint damage. I ask about sports, falls, and operations to spot high risk early.
Work and repetitive stress
Jobs with long standing, heavy lifting, or routine squatting and kneeling raise risk. Smart technique, timed breaks, and aids cut the impact without stopping work.
Genetics and anatomy
Family traits, limb-length differences, and childhood joint problems change load patterns. These factors may cause earlier symptoms despite careful activity.
Secondary joint disease
Conditions such as gout or rheumatoid arthritis can set the stage for later joint wear. Controlling inflammation reduces secondary damage.
- I stress prevention: strengthen muscles, manage weight, and protect injured joints.
- Normal exercise helps; avoid unmanaged overload and untreated tears.
| Risk factor | Typical effect | Why it matters | Practical step |
|---|---|---|---|
| Age (late 40s+) | Gradual cartilage change | Reduced healing and muscle mass | Begin strength and balance training |
| High weight | Increased knee and hip load | More wear per step | Weight loss, low-impact exercise |
| Prior injury / tear | Early joint degeneration | Altered mechanics and instability | Targeted rehab, consider brace if needed |
| Repetitive work | Focal cartilage stress | Accumulated microdamage | Ergonomic changes, rest breaks, technique |
Stages of osteoarthritis and what “progression” really means
Progress in joint disease often follows a personal path; I describe stages so patients can plan, not panic.
Early changes that may not show on X-ray
Early stage often brings occasional pain after activity, short stiffness, and mild swelling.
Symptoms may appear even when X-rays look near normal.
I focus on history and simple tests for diagnosis rather than relying only on imaging at this stage.
Moderate patterns: more frequent pain and limits
In moderate disease symptoms occur more often and daily tasks feel harder.
Stairs, long walks, or rising from the floor may need pacing or pain control.
Imaging may show smaller joint space and early osteophytes, but treatment still aims to preserve function.
Advanced stage: narrowing, spurs, and higher disability risk
Advanced stage usually shows clear joint space narrowing, larger osteophytes, and possible deformity.
Disability risk rises if muscle support and weight management are not used.
Why many people plateau or feel better for periods
Progression rarely runs in a straight line. Improved strength, lower inflammation, better sleep, and smarter pacing can stabilise symptoms for years.
Staging guides care but does not define your outcome; I treat pain and function first, not just the film on the X-ray.
| Stage | Typical symptoms | Common imaging | Key approach |
|---|---|---|---|
| Early | Occasional pain, brief stiffness | Normal or subtle changes | Exercise, weight control, monitor |
| Moderate | Frequent pain, reduced activity | Joint space narrowing, small osteophytes | Rehab, pain strategies, bracing |
| Advanced | Persistent pain, deformity, limits | Marked narrowing, large osteophytes | Surgical referral if conservative care fails |
When joint pain might not be osteoarthritis
I warn patients that not every new joint problem is the common degenerative condition. Sudden severe change often signals an alternate diagnosis and needs prompt review.
Red flags I treat urgently include sudden intense swelling, a hot or very red joint, fever, an inability to bear weight, severe night pain, or a recent injury with obvious deformity. These signs can mean infection, a fracture, crystal arthritis such as gout, or another inflammatory disorder.
Inflammatory arthritis usually presents differently. Expect prolonged morning stiffness, warmth across many small joints, and systemic symptoms such as fatigue or fever. That pattern contrasts with activity-linked stiffness and short morning stiffness seen in typical wear-related disease.
Gout often arrives with sudden, very painful attacks, commonly at the big toe, and needs a different treatment plan than degenerative joint problems. Treating the wrong condition delays relief and risks harm.
I reassure most patients that the usual degenerative condition is manageable. Still, new severe signs should prompt evaluation rather than assuming it’s normal. I use careful history, exam, and targeted tests to reach an accurate diagnosis and rule out urgent mimics.
| Feature | Urgent concern | Typical degenerative pattern |
|---|---|---|
| Onset | Sudden, severe | Gradual, activity-related |
| Appearance | Hot, red, swollen | Occasional mild swelling, not hot |
| Stiffness | Prolonged morning stiffness or all-day stiffness | Brief stiffness after rest (minutes) |
| Systemic signs | Fever, malaise | None or mild tiredness from pain |
How I diagnose osteoarthritis accurately
Accurate diagnosis begins when I listen closely to how your pain started and what changes it through the day. From that history I shape a focused exam and order only the tests that answer specific questions.
History: patterns that guide investigation
I ask when symptoms began, which activities worsen pain, what relieves it, and how sleep, walking, or work are affected. This helps me separate likely degenerative change from inflammatory or crystal types.
Physical exam: signs I look for
I check tenderness along joint lines, crepitus with movement, bony swelling, soft effusion, range of motion, stability, and nearby muscle strength. Weak muscles often worsen knee function and need early rehab.
Imaging and tests: when they help
X-rays confirm later-stage changes such as joint space narrowing, osteophytes, and alignment issues. Early films may look normal and should not override clinical findings.
There is no blood test for the degenerative type, but bloods rule out rheumatoid disease, gout, or infection when the pattern suggests another cause.
MRI is useful mainly for the knee when locking, suspected meniscal or ligament injury, or if symptoms and X-ray do not match.
- I choose tests to answer one clinical question at a time.
- The goal is a clear diagnosis and a safe, effective treatment plan.
| Step | Key finding | When useful |
|---|---|---|
| History | Activity-linked pain | Always |
| Exam | Tenderness, crepitus, instability | Directs treatment |
| Imaging / labs | X-ray changes; bloods to exclude other types | Targeted, not routine |
My non-surgical treatment approach for osteoarthritis
I start by defining realistic aims: reduce pain, protect the joint, and preserve activity. I explain that care focuses on function and quality of life rather than a quick cure.
Setting realistic goals
I set clear targets with patients: reduce pain episodes, lower flare-ups, protect joint surfaces, and keep independence in daily activities. We measure progress by activity tolerance and sleep quality.
Activity modification without over‑resting
I advise less high-impact load, more breaks, and safer techniques for lifting and squatting. Complete rest often worsens stiffness and muscle loss, so I favour paced movement guided by physiotherapy.
Heat versus ice and joint stress reduction
Use heat for morning stiffness and muscle tightness. Use ice after overuse or to ease swelling during a flare-up.
- Pacing, supportive footwear, and a cane when needed to unload painful joints.
- Long-term treatment plans work best; small gains add up over months.
- I tailor each plan to pain levels, safety, and daily roles at home or work.
| Problem | Practical tip | When to use |
|---|---|---|
| Stiffness | Warm packs, gentle range work | Before activity |
| Swelling | Ice, rest, elevation | After flare or heavy use |
| Joint load | Cane, footwear, pacing | Daily tasks, walking |
Physiotherapy and exercise that support joints safely
I guide patients toward simple movement routines that protect joints and rebuild confidence. Physiotherapy is central: stronger muscles unload painful areas and often reduce reliance on rest alone.
I teach range-of-motion work as joint “lubrication.” Gentle bend-and-straighten sets restore flexibility after sitting or waking and lower stiffness.
Strengthening for protection
Targeted strengthening around the knee and hip improves stability and cuts episodes of the joint “giving way.” Focus on quadriceps, gluteal, and core muscles with supervised progressions.
Aerobic and low-impact options
Regular aerobic exercise helps fitness, sleep, and pain control. I recommend low-impact activities such as walking on level ground, cycling, swimming, and aquatic therapy when land work hurts.
Gait, balance, and fall-risk training
Balance drills and gait training reduce falls, especially in older adults with knee or hip problems. I include simple steps and functional practice tailored to daily activities.
- Start gentle, increase gradually, and use pain as your guide—mild ache is okay; sharp pain is not.
- Individualise plans to prior injuries, surgery, and the joints involved.
- Physiotherapist-led programs ensure safe technique and steady progress.
| Exercise type | Primary benefit | Suggested use |
|---|---|---|
| Range-of-motion | Flexibility, less stiffness | Daily, short sets |
| Strengthening | Joint support, reduced pain | 3× weekly, progressive load |
| Aerobic (low-impact) | Fitness, mood, sleep | 30 min most days, adapt to pain |
Weight, diet, and lifestyle changes that can reduce joint pain
Modest, steady changes in weight and routine can cut joint pain significantly. I tell patients that even small drops in weight ease pressure on the knee, hip, back, and feet with every step.
Balanced eating supports muscle and overall health rather than promising a cure. Aim for adequate protein, whole grains, vegetables, legumes, and healthy fats. Avoid crash plans and extreme cleanses that are hard to sustain.
Supplements deserve a cautious view. Fish oils show clearer benefit for inflammatory joint disease; their role in osteoarthritis is mixed but generally safe. Glucosamine and chondroitin may help some people—often the knee—after several weeks. Try a time-limited trial and reassess benefit.
Lifestyle factors matter: improve sleep, break up long sitting, and keep daily walks short and steady. Combine diet with gentle strengthening to protect joints and reduce pain over months.
- Mechanical advantage: less weight = less joint load per step.
- Modest loss (5–10%) often yields meaningful symptom relief.
- Sustainable diet + exercise beats any “miracle” plan.
| Change | Effect on joints | Practical tip | Timeline |
|---|---|---|---|
| 5–10% weight loss | Reduced load on knee and hip | Small calorie cut, more walking | 8–12 weeks |
| Balanced diet | Better muscle mass, metabolic health | Protein at each meal, fibre-rich foods | Immediate and long-term |
| Fish oils | Possible symptom help; stronger for inflammatory arthritis | Discuss dose with clinician; 8–12 week trial | 4–12 weeks |
| Glucosamine / chondroitin | Mixed results; some knee benefit | Trial for 6–12 weeks, stop if no change | 6–12 weeks |
Medications and injections used for osteoarthritis pain relief
I explain medicines as tools to control pain so patients can stay active and do strengthening work. Medicines do not rebuild cartilage, so I always pair drug choices with exercise, weight control, and joint protection.
Topical NSAID gels for knees and hands
Topical NSAID gels often help local pain in the knees and hands more than deep joints like the hip. They give good symptom relief with fewer whole‑body side effects than oral tablets.
Paracetamol and what to expect from it
Paracetamol can ease mild to moderate pain when used within recommended doses. It may be enough for some daily tasks, but many need stronger options during flare-ups. I check liver risk and total daily dose, especially if other medicines are taken.
Oral NSAIDs and safety considerations
Oral NSAIDs (for example ibuprofen or naproxen) are stronger for activity‑linked pain. They can upset the stomach, affect kidneys, and raise cardiovascular risk. I screen for ulcers, high blood pressure, kidney disease, and heart problems before prescribing. When needed, I consider the lowest effective dose and stomach protection.
Steroid injections for severe pain in selected joints
Targeted steroid injections can calm severe pain in a single joint, commonly the knee or thumb. Relief may last weeks to months and can allow physiotherapy to resume. I use injections selectively and avoid repeated courses without review.
TENS and other supportive pain‑management options
TENS and similar devices help some patients, though evidence is mixed. Physiotherapists can advise correct use. Other supportive measures include splints, heat, ice, and topical rubs as part of a broader plan.
Why long‑term opioids are generally avoided
Long‑term strong opioids offer limited sustained benefit and carry risks of dependence and side effects. I reserve them only for carefully selected cases, short courses, and after specialist review.
- Medicines manage symptoms; combine them with exercise and load management for best outcomes.
- Choices depend on age, other health conditions, and current medicines—so personalised review matters.
| Option | Main benefit | Key safety note |
|---|---|---|
| Topical NSAID gel | Local relief for knees and hands | Low systemic side effects |
| Paracetamol | Mild–moderate pain control | Check total daily dose; liver safety |
| Oral NSAIDs | Stronger short‑term pain relief | GI, kidney, and heart screening needed |
Braces, supports, and everyday ergonomics for joint protection
Practical supports and better posture often give immediate relief and help long-term strength work. I recommend simple changes you can use at home, work, or while travelling in India.
Knee supports, canes, and footwear choices
Braces reduce joint stress and improve confidence during activity. They help while you build muscle strength and should fit correctly rather than being the priciest option.
- Choose a knee support sized by the manufacturer and try it during light walking before heavy use.
- Use a cane in the opposite hand to unload a painful hip or knee and steady your gait on uneven roads.
- Pick shoes with cushioning and stable soles; replace worn footwear that alters alignment.
Protecting neck, back, hips, and knees with posture
Posture-related issues often add load to the back and hips. Sitting too low, hunching over phones, or lifting incorrectly raises risk of evening joint pain.
Simple ergonomics help: chair height with feet flat, lumbar support, screen at eye level, micro-breaks every 30–45 minutes, and lift with knees, not the back.
| Problem | Practical fix | Benefit |
|---|---|---|
| Weak gait / falls | Cane, physiotherapy gait training | Safer walking, less overload to other joints |
| Desk-related back/neck strain | Adjust chair and screen, hourly stretch | Less morning stiffness, fewer flare-ups |
| Worn shoes | Stable cushioning, replace regularly | Better alignment, reduced knee pain |
I encourage physiotherapy to match supports to your needs and to teach safe daily movements. These modest steps often mean less pain by evening and more confidence on stairs and uneven surfaces.
When surgery is medically required, including joint replacement
When repeated, structured non-surgical care no longer controls symptoms, we begin to discuss surgery as a medically required step. I consider surgery only if persistent pain, sleep loss, or marked limits to walking and daily tasks remain despite rehab, weight control, medicines, and supports.
Signs conservative treatment is no longer enough
Red flags include severe ongoing pain, repeated falls, inability to walk needed distances, or loss of independence with basic activities. These outcomes raise disability risk and justify surgical review.
Joint replacement for hip and knee: benefits and limits
Replacement can greatly reduce pain and restore walking and function for many patients. More than 90% of hip and knee replacements are performed for degenerative change.
It does not recreate a young joint. High-impact sports remain discouraged to protect the implant.
Implant longevity and why results vary
Modern hip and knee implants commonly last 20 years or more, but durability depends on activity, weight, bone quality, and overall health.
- Success factors: good muscle strength, posture, controlled diabetes, and adherence to physiotherapy.
- Risks increase with very high activity, poor bone, or uncontrolled medical issues.
| Decision point | Typical reason | Practical note |
|---|---|---|
| Surgery considered | Persistent severe pain, limited function | Stepwise review after failed conservative treatment |
| Replacement goal | Reduce pain, improve walking | Realistic expectations; avoid high-impact strain |
| Longevity | Often 20+ years | Varies by patient and rehab quality |
Recovery and long-term care after orthopedic surgery
Surgery begins a pathway, not the end of treatment. I emphasise physiotherapy-guided recovery because it converts an operation into better walking, less pain, and safer daily life in Bangalore—stairs, buses, and uneven pavements included.
Physiotherapy-guided rehabilitation timelines and milestones
Early mobilisation starts within 24 hours for most replacements. You will work on standing, short walks, and simple range-of-motion tasks.
Over weeks we add progressive strengthening, balance work, and gait training. By 6–12 weeks many patients return to routine activities as strength and pain allow.
Managing swelling, stiffness, and safe return to daily activities
Swelling and stiffness are common early. I recommend elevation, suitable ice, gentle motion, and graded walking to ease both.
Return to stairs, bathing, and car travel depends on your strength and balance—not a fixed date. I check progress at follow-ups and clear activities when safe.
Preventing falls and protecting the operated joint
- Use proper footwear and bathroom grips at home.
- Use a cane or walker until balance training shows improvement.
- Maintain healthy weight and continue muscle work to protect the joint long-term.
Why recovery differs for each patient
Age, fitness, other health issues, and how closely you follow physiotherapy change timelines. I review wound healing, gait, and pain at visits and adjust the plan accordingly.

| Stage | Goal | Typical time |
|---|---|---|
| Early mobilisation | Safe walking, ROM | 0–2 weeks |
| Strength & balance | Independence on stairs | 3–12 weeks |
| Return to routine | Work, commute, walking outdoors | 6–12+ weeks |
Conclusion
I close with a simple summary: osteoarthritis is a common joint condition where cartilage and nearby structures change over time, causing pain, stiffness, and reduced function.
The usual pattern I see is activity-linked pain with brief stiffness after rest. Early, accurate diagnosis matters because not all joint pain has the same cause and some require urgent care.
My stepwise approach favours education, activity modification, physiotherapy and exercise, weight and lifestyle changes, targeted medicines or injections when needed, and surgery only when conservative measures fail.
Outcomes vary by person and joint, so I tailor each plan to your goals and overall health. For a detailed assessment and personalised treatment plan, book an appointment or visit me at Boss Multispeciality Hospital, Magadi Main Road, Bangalore (near Kamakshipalya and RR Nagar). I will review your diagnosis and guide safe, effective next steps for better joint health.