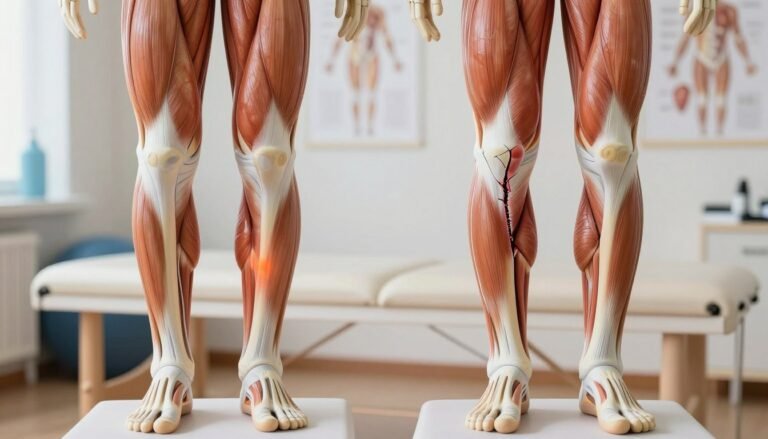
Rheumatoid Arthritis vs Osteoarthritis: Key Differences
Have you ever wondered why two people with the same joint pain can need very different treatments?
I am Dr. Lokesh Chowdary R (MBBS, MS – Orthopaedics), Managing Director and Senior Orthopedic Surgeon at Boss Multispeciality Hospital on Magadi Main Road, Bangalore.
Many patients arrive describing “arthritis” symptoms, but these two conditions are not the same even if the pain feels similar at first.
Osteoarthritis is a wear-and-tear problem where cartilage gradually breaks down. The other is an autoimmune problem where the immune system attacks the synovial lining of the joint.
Getting the right diagnosis guides the right plan. I focus on accurate assessment, start with non-surgical care, and use physiotherapy-guided recovery whenever possible.
Some people may have overlapping problems, so tests such as X-rays and blood work help us decide between home care, medicines, injections, or surgery.
I aim to reduce pain and protect joint function, but recovery varies from person to person and there are no one-size-fits-all timelines.
Why I’m Often Asked About Rheumatoid Arthritis vs Osteoarthritis in My Clinic
In my Bangalore clinic I often hear the same worry: “My joints ache — what exactly is causing it?” I say this is a very normal question.
Why joint pain can feel similar even when the cause differs
Pain is how the body signals trouble, but the same aching can come from different problems.
Which joints hurt, when they hurt, and what helps or worsens them give important clues. Morning stiffness, activity-related discomfort, and other symptoms point us toward the right type of condition.
Why the right diagnosis matters before treatment
Starting random medicines or injections can be risky if we do not know the diagnosis. I prefer a stepwise clinic approach.
- I take a clear history and examine the affected joints for swelling, warmth, and motion.
- I use targeted tests—X‑rays, blood work, or ultrasound—when needed to confirm the diagnosis.
- Physiotherapy‑guided recovery and lifestyle steps often protect function and reduce the need for surgery.
If you are unsure, that is okay. My job as your doctor is to narrow the cause methodically so we can reduce pain, restore function, and avoid unnecessary operations.
What Osteoarthritis Is and What “Wear and Tear” Really Means
Simple tasks like climbing stairs or typing can tell us a lot about how a joint is wearing down. I describe this process so patients understand why pain often starts slowly and with movement.
Cartilage breakdown and joint space narrowing
I define osteoarthritis as a common condition where cartilage—the smooth cushion inside a joint—gradually thins and frays. When that cushion reduces, the space between bones on an X‑ray looks smaller; we call this joint space narrowing.
Bone changes over time, including bone spurs
The body reacts to cartilage loss by changing bone shape. Small bony growths, or bone spurs, can form and limit motion or irritate nearby tissues.
Common joints involved
I see this pattern most often in the knees and hips, where load and posture matter a lot. Knee pain while walking or climbing is a frequent complaint.
Spine wear can cause low back and neck discomfort. Hand problems often start at the thumb base or end finger joints.
OA usually develops slowly. Early care focuses on activity modification, physiotherapy, weight management, and posture or ergonomic changes. I emphasize non‑surgical steps first because many patients maintain good function with consistent rehab and lifestyle changes.
What Rheumatoid Arthritis Is and How the Immune System Affects Joints
When the immune system turns on joint tissue, the result is a clear pattern of swelling, warmth, and long morning stiffness. I explain this calmly so patients focus on timely care rather than fear.
Autoimmune attack on the synovial lining
Rheumatoid arthritis is an autoimmune disease in which the immune system targets the synovial membrane that lines joints.
This leads to persistent inflammation and a cycle of tissue irritation unless we interrupt it with medical therapy.
How inflammation harms cartilage and bones
Active inflammation can erode cartilage and erode nearby bones over time. That damage reduces function and can cause deformity if missed.
Early diagnosis matters because treatments aim to stop inflammation and protect cartilage and bones before irreversible change occurs.
Why symptoms can go beyond the joints
The same inflammatory process can affect the whole body and, in some people, involve organs such as the lungs, eyes, or heart.
I work with rheumatologists to spot red flags, guide safe physiotherapy, and set realistic goals so patients regain function and avoid unnecessary procedures.
- Recognise patterns on exam and imaging.
- Refer early for specialist disease‑modifying treatment.
- Focus on joint protection, exercise, and coordinated follow-up.
rheumatoid arthritis vs osteoarthritis Compared Side by Side
A clear side-by-side view helps you spot which problem is driving joint pain and what to do next. I will contrast root cause, speed, pattern, stiffness, and whole‑body signs so you can see why treatment differs.
- I explain the cause: mechanical wear and tear versus immune-driven inflammation.
- I show speed: one usually develops slowly, the other can progress faster without control.
- I highlight pattern and stiffness to guide diagnosis and care choices.
| Feature | osteoarthritis rheumatoid (mechanical) | osteoarthritis rheumatoid arthritis (inflammatory) |
|---|---|---|
| Root cause | Cartilage wear and joint loading | Autoimmune inflammation of the joint lining |
| Onset speed | Gradual over years | Can appear and worsen more quickly |
| Joint pattern | Often asymmetrical, one side worse | Often symmetrical, same joints both sides |
| Morning stiffness | Brief, eases with movement | Typically >1 hour, improves later in day |
| Systemic signs | Rarely causes fatigue or fever | May cause fatigue, low fever, reduced appetite |
Why this matters: I tailor treatment to the cause. Immune‑driven disease needs medicines to slow inflammation. Mechanical wear focuses on joint protection, exercises, weight control, and pain relief.
Symptoms You Might Notice With Osteoarthritis
Day-to-day chores often reveal the earliest changes in a joint’s comfort and strength.
Mechanical pain commonly worsens with activity and eases with rest. You may feel it after climbing stairs, standing for long periods, or doing housework. The pain can return once you start moving again.
Stiffness is usually brief after waking or sitting for a while. Gentle movement loosens the joint. After heavy use you may notice a returning stiffness that fades with activity.
Many people hear grinding or cracking when they bend a joint. This crepitus happens when smooth cartilage surfaces become irregular.
Swelling can appear but is often milder than inflammatory conditions. The joint may feel less stable or a bit weak over time. These functional changes increase stress on nearby muscles and can limit tasks.
Left unattended, long-standing symptoms may contribute to disability. Early physiotherapy and targeted non-surgical care can protect motion and reduce the risk of joint damage. I recommend an orthopedic check if pain or swelling lasts for weeks or daily activities become hard.
| Symptom | Typical Pattern | First steps I suggest |
|---|---|---|
| Pain | Worse with use, better with rest | Activity changes, analgesics, physiotherapy |
| Stiffness | Brief after inactivity; returns after overuse | Gentle movement, heat therapy, exercise |
| Grinding / Swelling | Crepitus common; mild puffiness after use | Strengthening, joint protection, evaluation |
Symptoms You Might Notice With Rheumatoid Arthritis
When several small joints feel tender and stiff for hours each morning, that pattern is important. I watch for signs that point to an inflammatory process rather than simple wear and tear.
Warm, swollen, tender joints with prolonged morning stiffness
Joints may look puffy, feel warm, and hurt to touch. Morning stiffness often lasts more than an hour and slowly eases with movement.
Fatigue and feeling unwell as inflammation builds
Ongoing inflammation can cause tiredness, low appetite, and mild fever. This general unwell feeling often comes before clear joint loss or deformity.
Changes over time: deformity risk without timely control
Persistent inflammation can erode joint integrity and lead to progressive deformity if not treated. Early control reduces the chance of functional loss.
Rheumatoid nodules and why they can appear under the skin
Some people develop small firm nodules near pressure points. They are uncommon but can occur alongside long‑standing inflammatory disease.
I work with rheumatologists and physiotherapists to control inflammation and protect movement. Prompt evaluation is wise when multiple joints are swollen, stiffness is prolonged, or fatigue is persistent.

| Feature | Common finding | What I do |
|---|---|---|
| Morning stiffness | Typically >1 hour | Recommend specialist review and early therapy |
| Systemic signs | Fatigue, low fever, appetite loss | Check blood markers; coordinate care |
| Progression | Risk of deformity if untreated | Protect joints, start disease‑controlling treatment |
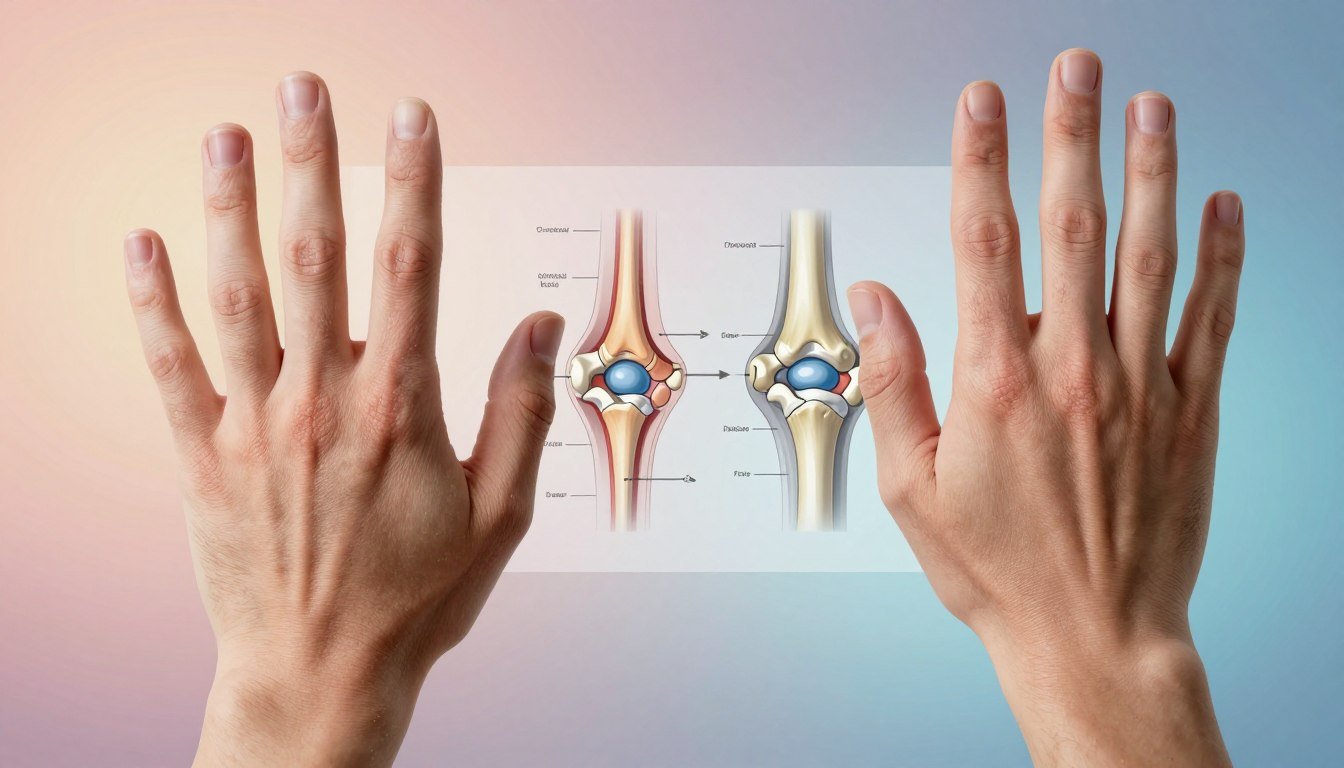
Hands, Fingers, and Wrists: How RA and OA Look Different
Visible differences in the hands often tell me whether the problem is inflammatory or mechanical. I look for which joints are swollen, which fingers are stiff, and whether signs appear on both sides of the body.
Patterns I see with inflammatory disease
Inflammation commonly hits the wrists and the knuckles (MCP joints) on both hands. Swelling can make the whole finger look uniformly puffy — a “sausage-like” appearance.
Over time, uncontrolled inflammation may change finger position and weaken grip. These changes affect fine tasks like buttoning or writing.
Patterns I see with mechanical wear
Wear-related changes tend to focus at the thumb base (CMC joint) and the end finger joints near the nails (DIP joints). Pain and stiffness here often come with bony bumps.
Those bony growths show bone and cartilage remodeling rather than active immune swelling.
- I explain that hands and finger patterns help separate causes during an exam.
- Don’t rely on online photos alone—seek a hands-on evaluation and imaging if needed.
- Early splinting, hand therapy, and targeted treatment reduce symptoms and protect function.
Risk Factors That Increase the Chances of RA or OA
Understanding personal and environmental risks can change how we prevent joint damage. I use risk assessment to guide early checks and simple prevention steps.
Shared risks to watch for
Family history and excess weight raise the risk of both forms of joint disease. That does not mean you will develop a problem, but it signals who may need earlier evaluation.
Risks I see most with wear‑related disease
Age is a major factor: cartilage thins over time. Prior injuries — sports injuries or fractures near a joint — also increase risk. Repetitive overuse and poor alignment speed mechanical wear.
Risks linked to immune‑driven disease
The inflammatory form is more common in women. Smoking and certain environmental exposures, such as silica, raise risk. Gum disease has also been discussed as a possible association with immune misfiring.
- Extra weight increases stress on knees, hips, and low back and can speed symptom progression.
- Early weight management, safe exercise, and quitting tobacco lower long‑term risk.
- Lifestyle steps help, but diagnosed inflammatory disease usually needs disease‑controlling drugs under specialist care.
If you have several risk factors, consider an early check. I favour timely assessment so we can protect function and build a prevention plan together.
How I Diagnose OA vs RA During an Orthopedic Evaluation
When a patient walks in, the first thing I do is listen to how the pain began and which joints trouble them most.
What I ask in your history
I ask which joints hurt, whether one side or both are affected, and how long stiffness lasts each morning.
I also ask what makes pain better or worse, prior injuries, and any family history of joint disease.
What I look for on examination
I examine for swelling, warmth, tenderness, joint stability, and range of motion. I watch how you walk and how you use your hands.
Imaging and what it shows
Plain X-rays are the first test. Mechanical loss often shows joint space narrowing and osteophytes. Inflammatory disease may show erosions and early joint damage.
Blood tests and advanced imaging
Blood tests for inflammation markers and rheumatoid factor support the clinical picture but do not replace it.
I order ultrasound or MRI when soft-tissue or early inflammatory changes are suspected.
Joint fluid analysis when needed
If a joint is very swollen or the presentation is unusual, I sample fluid to exclude gout or infection before starting treatment.
| Step | Purpose | Typical finding |
|---|---|---|
| History | Guide likely cause | Pattern: one side vs both, morning stiffness |
| Exam | Confirm inflammation or mechanical signs | Swelling, warmth, limited motion |
| X‑ray | Detect structural change | Joint space narrowing, osteophytes or erosions |
| Blood/Imaging | Support diagnosis | Raised markers, MRI/ultrasound soft‑tissue changes |
| Joint fluid | Rule out infection/gout | Crystals, microbes, cell count |
I use a step-by-step approach so tests back up what I find at the bedside. Correct diagnosis guides safer, more effective treatment and helps avoid unnecessary drugs or procedures. If needed, I refer you to a specialist while coordinating ongoing care as your doctor.
Non-Surgical Treatment Approaches I Commonly Recommend First
Before any surgery is considered, I focus on practical steps that reduce pain and restore function. For most patients, a structured conservative plan brings the best early gains and helps avoid unnecessary procedures.
Pain control and safe drugs
I start with simple pain control: acetaminophen and short-term NSAIDs when appropriate. I warn patients about stomach, kidney, and heart risks and avoid long-term opioid use due to dependency and side effects.
Topicals, injections, heat and cold
Topical creams or gels can ease superficial joint pain with fewer systemic risks. For selected cases, targeted joint injections reduce symptoms and allow focused rehab rather than serving as a cure.
Use heat for stiffness and gentle loosening. Use cold packs to calm swelling. Apply each for 10–20 minutes and protect skin with a cloth.
Physiotherapy, weight, and posture
Guided physiotherapy is central to my plan. Strengthening muscles around the joint cuts joint stress and improves function. I prescribe simple exercise routines that patients can do at home.
Gradual weight loss reduces load on knees, hips, and the low back. I pair realistic goals with supervised exercise and diet advice. Posture and ergonomic fixes at work ease neck and back strain and lower daily stress on joints.
- I prioritise non-surgical care and realistic timelines.
- Consistent movement, targeted strengthening, and smart pain control often make the biggest difference.
| Intervention | Purpose | When I use it |
|---|---|---|
| Acetaminophen / NSAIDs | Reduce pain | Short-term, with risk review |
| Topical agents / injections | Local symptom relief | Superficial joints or selected OA cases |
| Physiotherapy & exercise | Improve function, reduce stiffness | Default for most patients |
| Weight & ergonomics | Reduce joint stress | Knees, hips, back and neck complaints |
When Medications and Surgery Come Into the Plan
When joint symptoms persist despite therapy, we consider stronger medical options and, sometimes, surgery. My aim is to limit loss of function and reduce long‑term disability while minimising risk.
Medications that slow disease activity
For immune‑driven disease I work with rheumatology colleagues to start DMARDs and, when needed, biologic drugs. These medicines calm inflammation and aim to stop joint damage rather than simply masking pain.
Short‑term steroids and careful use
Corticosteroids can rapidly ease flare symptoms. I use them sparingly while a longer‑term plan starts, because side effects rise with prolonged use.
When surgery is considered
Surgery becomes an option if pain and loss of function persist despite well‑delivered conservative care, or when structural joint damage is severe. Procedures include synovectomy or joint replacement, chosen only after shared decision‑making.
Recovery and rehabilitation
Recovery timelines vary by age, bone health, fitness, and how closely patients follow rehab. Physiotherapy is essential to restore movement, rebuild strength, and improve recovery outcomes.
| Aspect | What I assess | Typical goal |
|---|---|---|
| Advanced drugs | Response, safety, specialist coordination | Control inflammation and prevent joint damage |
| Surgery | Pain, function, imaging, failed conservative care | Restore function, reduce disability |
| Rehabilitation | Strength, range, adherence | Speed recovery and protect results |
Conclusion
Knowing the cause of joint pain is the first step toward restoring daily function. The two main types of arthritis differ in cause, symptom pattern, and treatment goals.
Look for practical clues: osteoarthritis often feels like activity-related mechanical pain with brief stiffness. In contrast, rheumatoid arthritis commonly brings prolonged morning stiffness, swelling, and sometimes whole-body symptoms.
Don’t guess. A structured diagnosis leads to safer, more effective treatment. I start with the safest options, emphasise physiotherapy-guided recovery, and reserve surgery for clear medical need.
Every patient’s recovery timeline differs. If you have persistent pain, swelling, stiffness, or trouble with routine tasks, book an appointment or visit me at Boss Multispeciality Hospital, Magadi Main Road, Bangalore (near Kamakshipalya and RR Nagar) for a proper orthopedic evaluation.